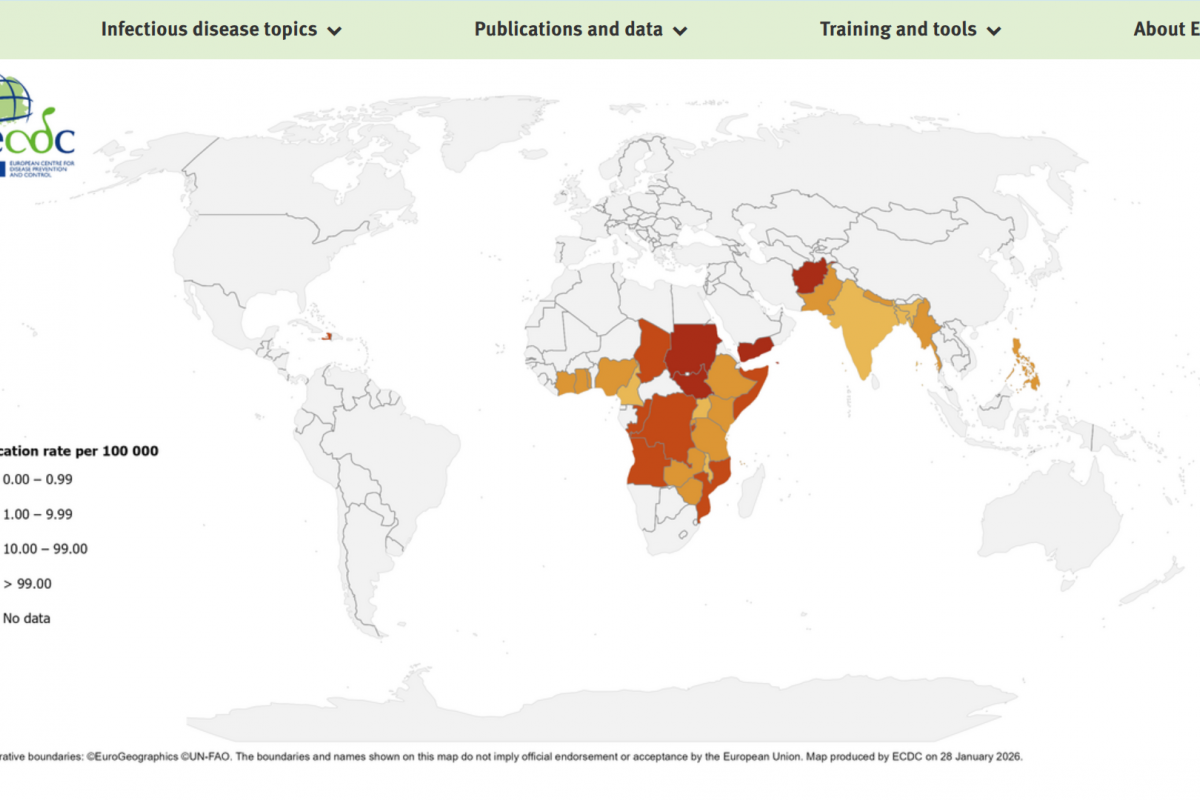
Chikungunya is a viral disease spread through the bites of infected mosquitoes. Since 2013, the virus has been detected in the Americas, and it has rapidly spread throughout Brazil.
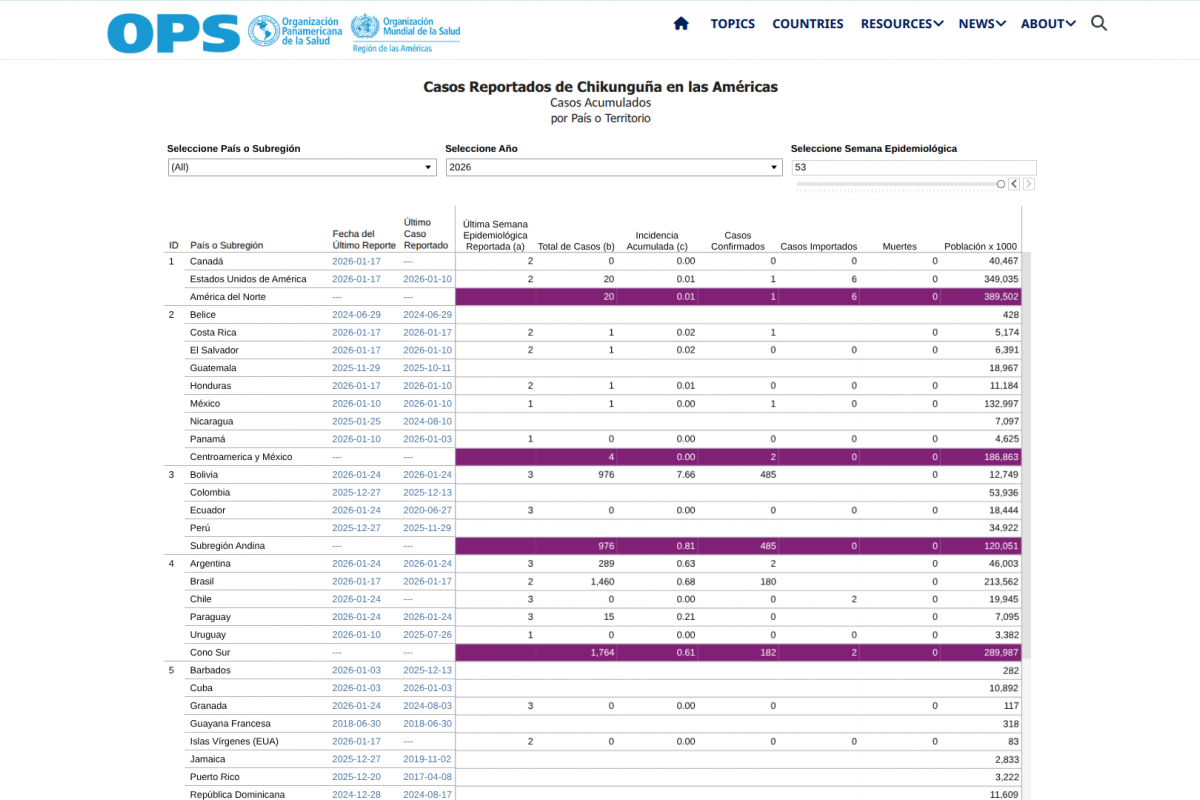
Brazil has reported the highest number of chikungunya cases worldwide, including 246 related fatalities in 2024.
As of early February 2026, Brazil has reported 1,480 suspected and 180 confirmed cases of chikungunya.
In response to this serious public health issue, Brazil is taking additional measures to secure access to chikungunya vaccines.
Valneva SE today announced the launch of a Pilot Vaccination Strategy (PVS) in Brazil in collaboration with Instituto Butantan, one of the world's largest biomedical research centers. The companies initially signed a technology transfer agreement in January 2021.
This new PVS program will utilize Valneva's single-dose chikungunya vaccine, IXCHIQ®.
The goal of this program is to support post-marketing commitment studies that will assess the effectiveness and safety of IXCHIQ® in real-world conditions, providing valuable data from a large population.
Esper Kallas, M.D., Ph.D., The Director of the Instituto Butantan outlined the path toward the PVS program on February 3, 2026, stating: "With ongoing engagement from the Ministry of Health, regional health secretaries, and ANVISA, I am confident that we have established a program that is both robust and compliant with regulatory standards."
"These combined efforts are expected to ensure timely access to vaccination and alleviate the significant public health burden associated with this arboviral disease."
This initiative follows an announcement in January 2026 by Eurofarma. This Brazilian pharmaceutical company stated that it had acquired the rights to sell and distribute Bavarian Nordic's chikungunya vaccine, CHIKV VLP (VIMKUNYA®), in Brazil.
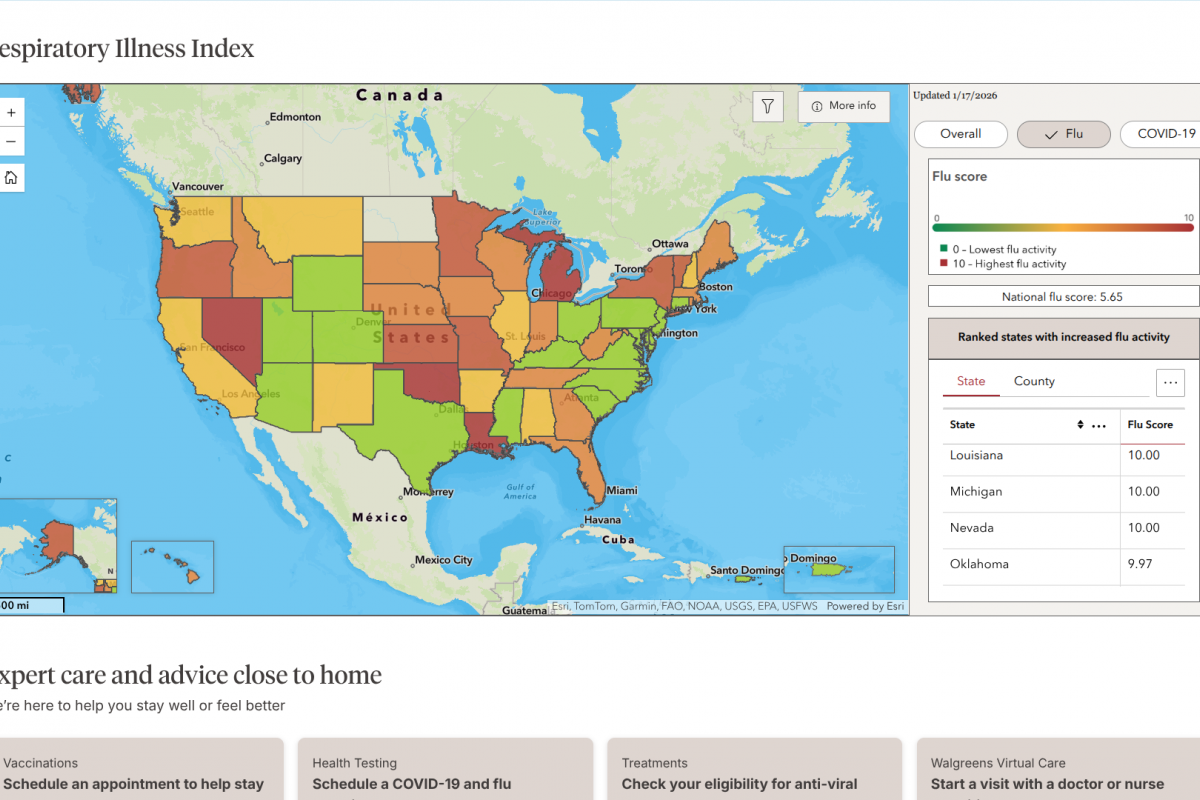
These actions in Brazil may help the state of Florida reduce the number of travel-related chikungunya cases. As of December 2025, 328 travel-related chikungunya cases have been confirmed, many in Miami-Dade County.
Furthermore, 14 cases of chikungunya fever were reported in 2026 among persons who had traveled internationally, with one local case in southeastern Florida.