India has recently increased in popularity as a destination for United States travelers. Last year, the U.S. National Travel and Tourism Office tanked India as the second most popular international travelers destination.
While tourism has increased, so has the number of Chikungunya virus outbreaks in India.
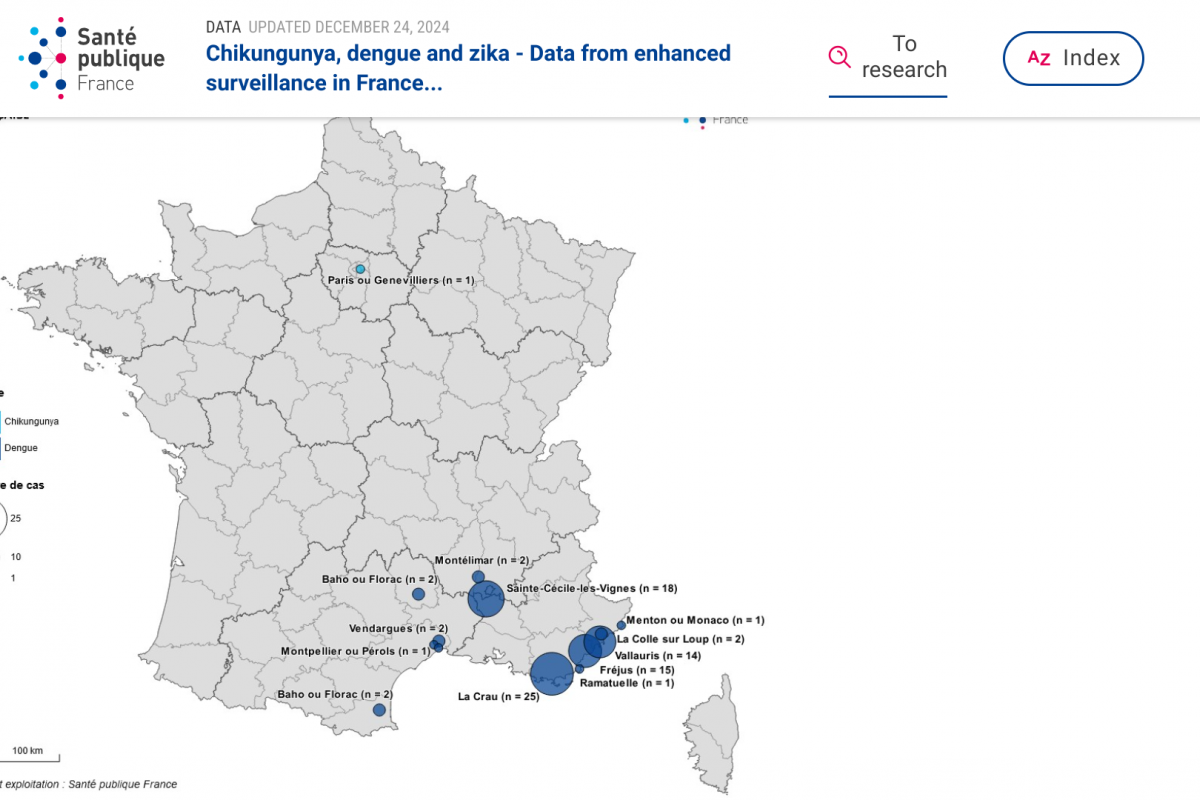
On December 19, 2024, the U.S. CDC reported an outbreak of Chikungunya in India's Maharashtra and Telangana states.
According to India's National Center for Vector-Borne Diseases Control, 192,343 CHIKV cases were reported in 2024. Those infected with this mosquito-transmitted disease develop some symptoms and many report long-term symptoms.
Pune's National Institute of Virology has indicated that Chikungunya virus variants are causing more cases and lingering symptoms in 2024.
A study published on October 19, 2024, determined that the incidence of post-chikungunya chronic rheumatism and fatigue and the impact on quality of life and chronic fatigue in adults seven years after infections were significant.
These experts have identified Chikungunya's "Indian Ocean lineage," first identified in 2006, as the primary cause of the recent surge in cases and lingering symptoms. This novel lineage has also spread globally.
"India's ongoing Chikungunya outbreak is a good reminder for international travelers about this often forgotten mosquito illness and the importance of vaccination. Infection can lead to long-term health issues such as chronic joint pain, and people 65 years and older are especially at risk for complications," Jeri Beales, MSN, RN, informed Vax-Before-Travel.
"The approved vaccine is given as a single dose, and studies show it is highly effective for at least several years after receiving. The U.S. CDC does not recommend every traveler to India get the vaccine. It is only approved for people 18 years and older in the U.S., so be sure to talk to your local travel clinic or physician," added Beales, who leads Destination Health Clinic, a Boston, Massachusets area travel health provider specializing in health education and vaccination for international travelers.
Since 2013, the Asian genotype has led to Chikungyna outbreaks in the Region of the Americas, which will continue in 2026.
Last year, the Pan American Health Organization reported over 421,018 Chikungunya cases and 211 related deaths in the Americas.
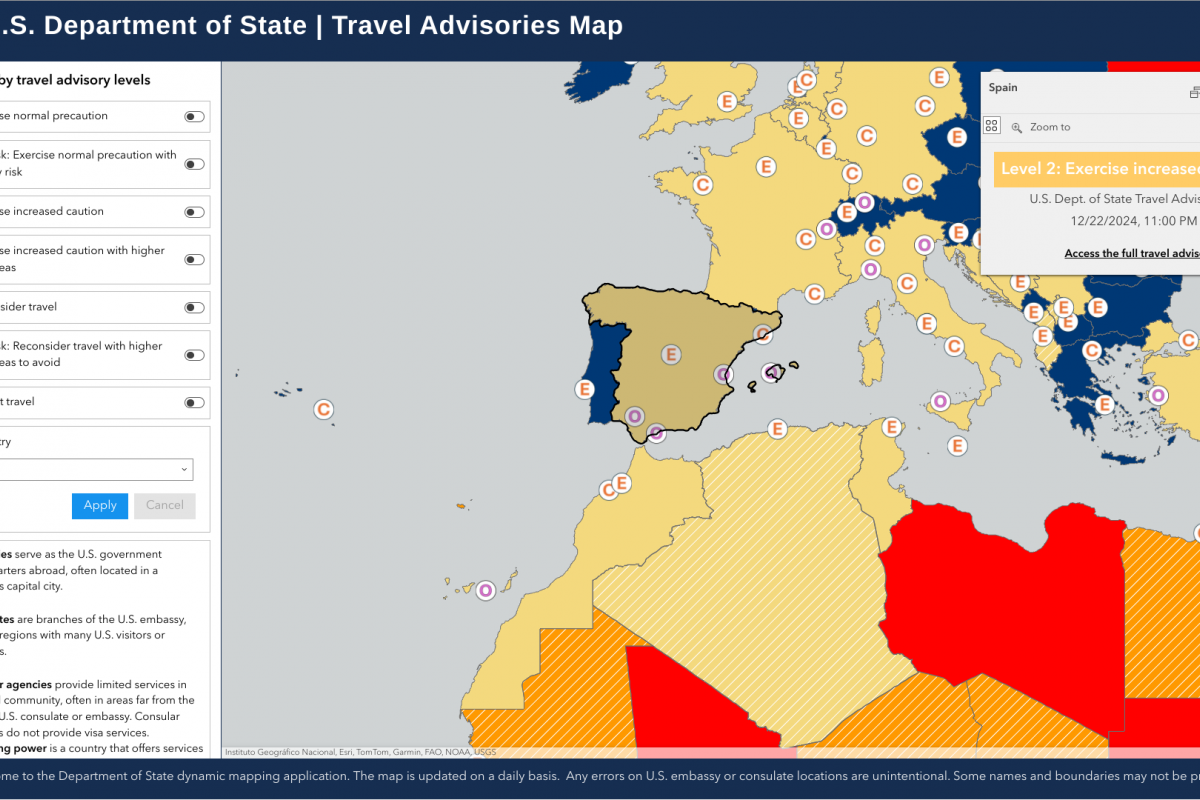
The CDC's Level 2—Practice Enhanced Precautions Travel Health Advisory recommends the FDA-approved Chikungunya vaccine for certain visitors and long-term residents in India and other areas reporting outbreaks.
As of January 2025, Valneva SE's IXCHIQ® (VLA1553) vaccine is offered at many travel clinics and pharmacies in the U.S.