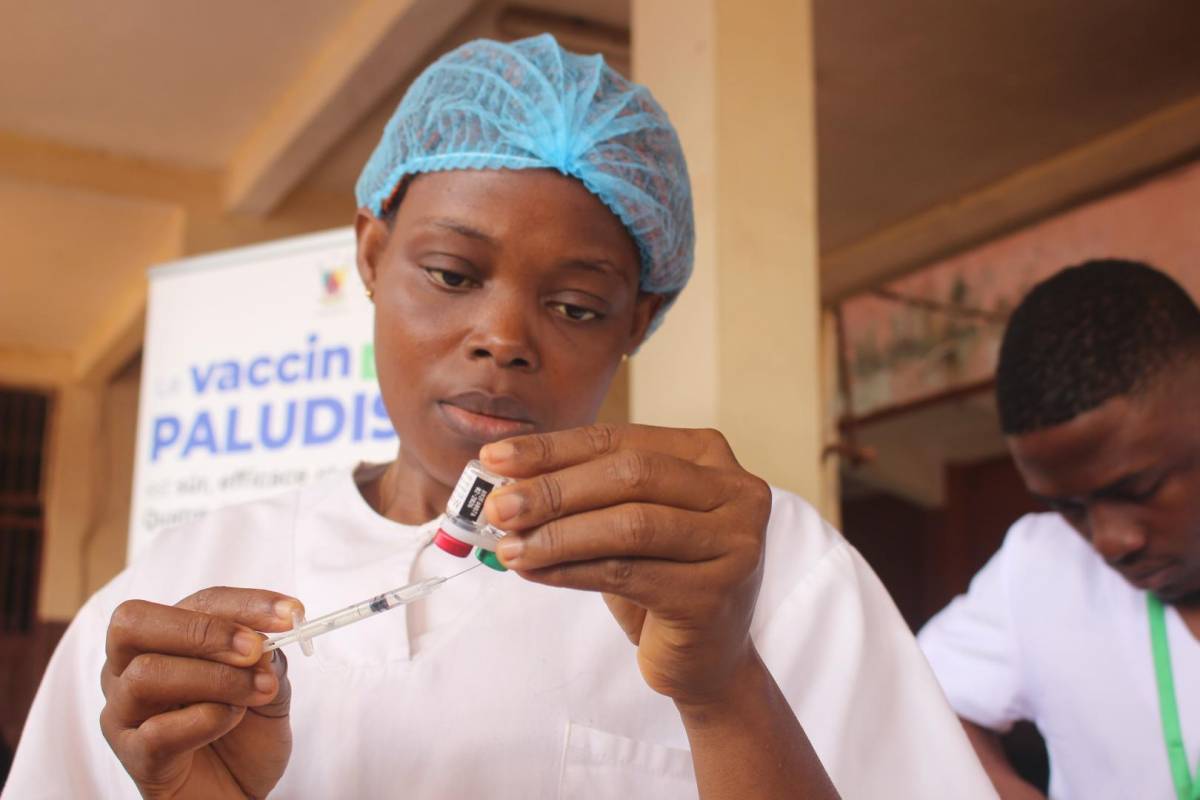
The Republic of Cameroon today launched the Mosquirix™ (RTS,S) malaria vaccine into its routine national immunization services, becoming the first country to do so outside the malaria vaccine pilot program previously carried out in the African countries of Ghana, Kenya, and Malawi.
The launch on January 22, 2024, came after Cameroon received 331,200 Mosquirix doses in November 2023. Additional malaria vaccines are expected in 2024.
“The vaccine is an additional tool for malaria control. The country has chosen it (Mosquirix) based on its pre-qualification, ensuring guaranteed quality, efficacy, and safety for inclusion in the vaccination program,” said Dr. Shalom Ndoula, Permanent Secretary of the Expanded Programme on Immunization in Cameroon, in a press release.
“It will specifically target all children aged six months as of December 2023.”
In 2023, the Pan American Health Organization estimated that approximately 41 million people in twenty-one Latin American countries are at risk for malaria.
In the U.S., the Centers for Disease Control and Prevention confirmed about ten locally-acquired malaria cases in 2023.
Two approved malaria vaccines are available in certain countries in 2024 but not in the United States.