Search API
With about one million people developing herpes zoster (shingles) in the US each year, simplifying the vaccination process is essential for at-risk seniors.
Approximately 99% of older adults have the virus that causes shingles inside their bodies.
With 55 million Americans aged 65 or older, many of whom live in California, Florida, and Texas, accessing the US Food and Drug Administration (FDA)-approved Shingrix® vaccine is a priority.
GSK plc, the manufacturer of Shingrix, announced that the FDA has recently approved a prefilled syringe presentation, which eliminates the need to reconstitute the vaccine separately before administration, thereby simplifying the vaccine administration process for healthcare professionals.
Brigid Groves, Vice President of Professional Affairs at the American Pharmacists Association, stated in a press release on July 17, 2025, "The prefilled syringe presentation of GSK's shingles vaccine is good news, providing a convenient method of administration."
"The FDA approval is a positive step toward driving prevention of this painful disease, and as a practicing pharmacist, I welcome the availability of this new presentation."
The Centers for Disease Control and Prevention (CDC) recommends two doses of GSK's shingles vaccine to prevent shingles and related complications in adults aged 50 years or older. Additionally, two doses are recommended for adults aged 19 years or older who are or will be immunocompromised or immunosuppressed.
The CDC states that as people age, the strength of their immune system's response to infection wanes, increasing the risk of developing shingles.
Additionally, Shingrix vaccination may play a role in delaying the onset of dementia.
Over the past few years, various studies have reported causal evidence that herpes zoster vaccination may prevent a proportion of dementia cases.

Throughout 2025, mpox outbreaks have been reported in various African countries, where the disease has become endemic in forested areas of Central and West Africa.
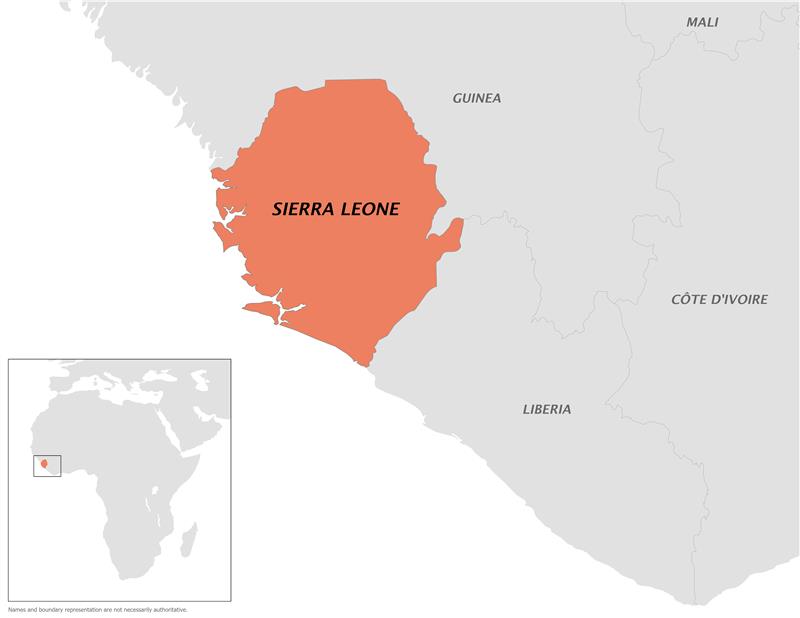
According to the U.S. Centers for Disease Control and Prevention (CDC), an outbreak of clade II mpox is currently occurring in Sierra Leone, where mpox is endemic.
The CDC states that, unlike the ongoing global clade II mpox outbreak, which began in May 2022, this outbreak has affected males and females aged 20 to 39 years similarly.
Furthermore, person-to-person transmission has occurred during this outbreak, including through sexual or other intimate contact.
As of July 17, 2025, Mpox vaccination is recommended for travelers to Sierra Leone who anticipate at-risk activities.
For those recommended to receive the mpox vaccination, two doses of the JYNNEOS® (MVA-BN®, IMVAMUNE®) vaccine, administered at least 28 days apart, are the standard protocol to maximize immunity.
Some countries, such as France, are offering mpox vaccine booster doses in 2025.
Additionally, current research is focused on the risk/benefit of mpox vaccination in infants, breastfeeding, and pregnant women.
This CDC-recommended vaccine is commercailly available in clinics and pharmacies throughout the United States.
The Pacific Community has recently reported that mosquito-borne diseases, such as dengue fever, are rising sharply throughout the various island nations in the Western Pacific Region.
As of July 16, 2025, the SPC reported American Samoa, Australia, Cook Islands, French Polynesia, New Zealand, Samoa, Tonga, and Tuvalu had confirmed dengue cases in 2025.
Of note, the American Samoa Department of Health declared the dengue outbreak in the country a public health emergency as of early July. A red alert for DENV-1 and DENV-2 serotypes has been added.
To alert international travelers of this serious health risk, the U.S. Centers for Disease Control and Prevention (CDC) reissued its Level 1 - Practice Usual Precautions, Travel Health Advisory on July 17, 2025.
For 16 countries, the CDC recommends that travelers visiting dengue outbreaks should prevent mosquito bites by using an EPA-registered insect repellent, wearing long-sleeved shirts and long pants when outdoors, and sleeping in an air-conditioned room or a room with window screens.
While many of these countries offer access to dengue vaccines, the United States does not, except for children in Puerto Rico, where dengue has become endemic.

Over the past two years, the Oropouche virus has been reported in regions of South America, Central America, and the Caribbean, raising substantial concerns among international travelers and healthcare providers attempting to diagnose the disease.
Oropouche viral disease presents clinically with symptoms that overlap with those of other mosquito-transmitted diseases such as Chikungunya, Dengue, Malaria, and Zika.
To address this need, Quest Diagnostics, based in New Jersey, announced the launch of a new diagnostic laboratory test for the Oropouche virus.
Beginning later this summer, Quest's advanced laboratory in San Juan Capistrano, California, will perform the test using polymerase chain reaction (PCR) technology, with serology testing to follow later this quarter.
Reverse transcription PCR testing can identify the RNA of the virus during the early stages of infection to aid diagnosis.
Serology testing, which identifies antibodies produced by the immune system in response to the virus, can aid in diagnosing the virus in later stages of infection.
"As one of the leading providers of laboratory testing, Quest plays an essential role in ensuring the U.S. is prepared to respond to potentially dangerous emerging diseases, such as Oropouche virus," said Yuri Fesko, MD, Senior Vice President and Chief Medical Officer at Quest Diagnostics, in a press release on July 15, 2025.
"By developing this test, we are prepared to act quickly to offer scalable testing to complement public health labs should this virus become a public health threat."
Oropouche and other virus testing are commercially offered by Ulta Labs Tests.
From a prevention perspective, the U.S. CDC recommends avoiding outbreaks, such as those in Brazil, Cuba, and Panama, and taking steps to limit mosquito bites.
Brazil has reported cases of Oropouche virus being passed from a pregnant woman to their fetus. These cases are currently under investigation.
The CDC says pregnant travelers should talk to their healthcare provider about travel plans, why they're traveling, steps to prevent insect bites,
As of July 17, 2025, no vaccine is available to prevent this disease, nor are there any medicines to treat Oropouche infections.

During the summer of 2025, the global Chikungunya outbreak continues to expand, with reported travel-related cases on the southeast coast of the People's Republic of China.
China's Centre for Health Protection (CHP) of the Department of Health (DH) announced today that an outbreak of the mosquito-transmitted Chikungunya fever (CF) has occurred in Shunde, Guangdong, which began in July 2025 and was triggered by imported cases.
As of July 15, 2025, a total of 478 confirmed cases have been reported, all of which exhibited mild symptoms.
According to the information provided by Guangdong Province, the current CF outbreak mainly occurred in the towns of Lecong, Beijiao, and Chencun in Shunde, which are not popular tourist destinations for Hong Kong citizens.
While no confirmed cases of CF have been reported in Hong Kong so far this year, the risk of imported cases has increased due to frequent travel between Guangdong and Hong Kong.
Hong Kong is a favorite destination for international travelers, welcoming over 40 million visitors in 2024.
Between 2016 and 2019, the number of imported CF cases recorded in Hong Kong ranged from one to 11 each year. There have been no CF cases in Hong Kong since 2020.
The CHP is closely monitoring the trend of CF in neighboring areas.
Off China's east coast, Taiwan has reported Chikungunya cases in 2025.
As of July 16, 2025, Chikungunya vaccines were unavailable in China; however, they have become commercially available in various countries, such as the United States. Since Chikungunya is a vaccine-preventable disease, health agencies recommend vaccination before visiting Chikungunya outbreaks.
The Romanian Government recently posted on Facebook that a confirmed case of malaria has been reported by the Public Health Directorate of the Municipality of Bucharest, in a resident with no history of recent travel abroad.
As of July 10, 2025, the Ministry of Health reported that there have been 21 travel-related malaria cases this year, and this new case is the first locally acquired case.
Since malaria is a mosquito-borne disease, this report raises concerns regarding potential additional local cases in Romania.
Currently, malaria vaccines are offered in various African countries, but not in Romania or the United States.
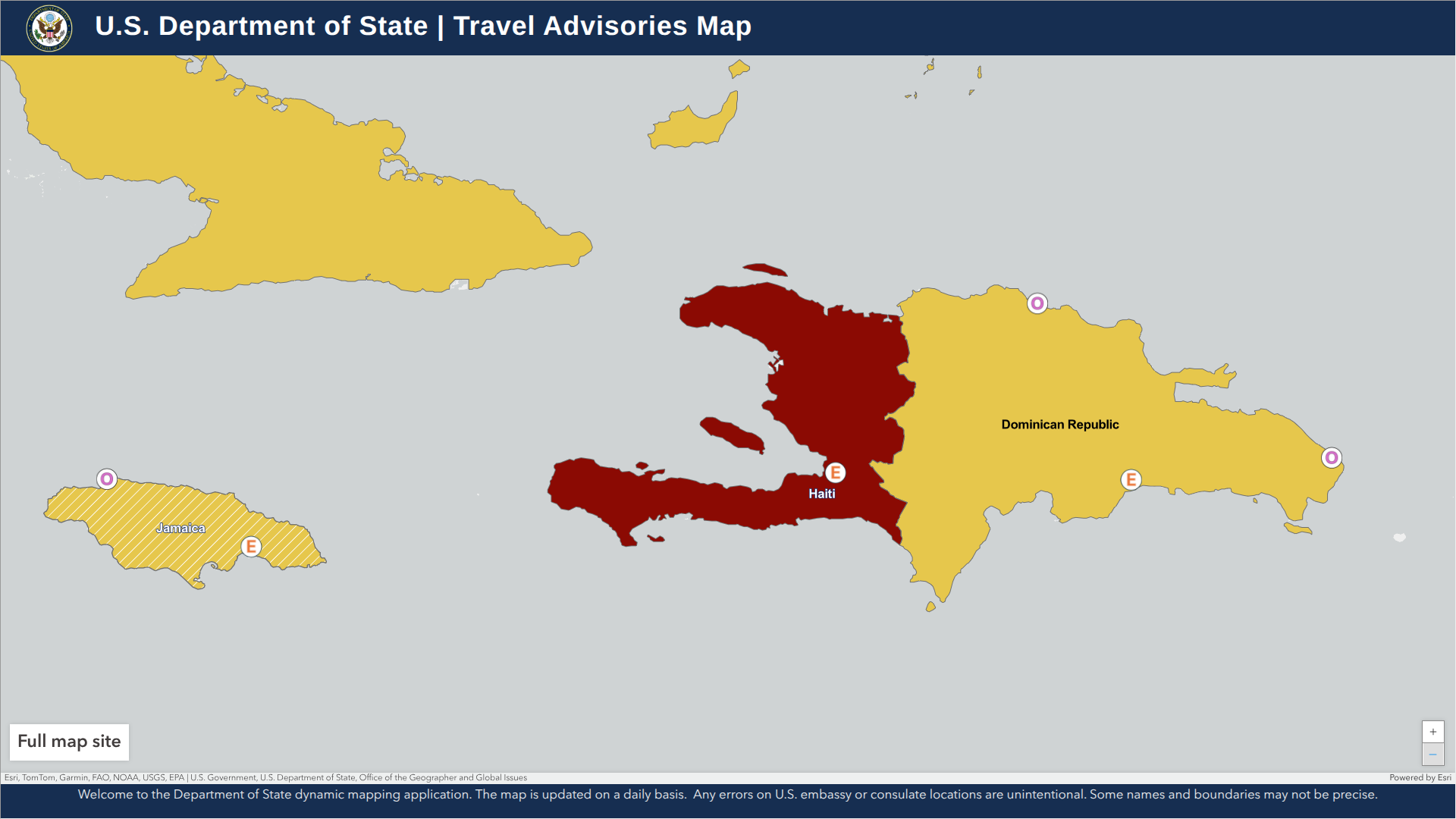
As the prolonged civil unrest continues to challenge the government of Haiti, the western part of the island of Hispaniola remains at risk for international visitors.
Haiti has been under a State of Emergency since March 2024.
According to the U.S. Department of State's updated Level 4: Do Not Travel advisory, as of July 15, 2025, civil unrest continues, and access to healthcare services in Haiti remains very limited for both residents and visitors.
Furthermore, the U.S. government has limited ability to assist U.S. citizens in Haiti. Local police and first responders often lack sufficient resources.
U.S. government employees working in Haiti must obtain special permission to travel outside the embassy compound due to security risks, and Embassy personnel are prohibited from traveling on foot in the capital city of Port-au-Prince.
Additionally, do not cross the land border between Haiti and the Dominican Republic, as the roads from major Haitian cities to the border pose significant dangers.
In addition to the U.S., the UK's Foreign, Commonwealth & Development Office has issued similar advice for Haiti in 2025. If you choose to travel, obtain appropriate travel insurance that covers your itinerary, planned activities, and expenses in the event of an emergency.
From a health perspective, the U.S. CDC recommends that international travelers planning to visit Haiti speak with a travel vaccine consultant at least one month before departure to obtain the necessary vaccinations and medical supplies.
The CDC highlights travel vaccines, including those for chikungunya, cholera, and rabies, before visiting Haiti.
This year, four people in Florida have died from an infection caused by a bacterium commonly known as the "flesh-eating" bacterium. To date, 11 infections in various countries have been reported this year from this waterborne and foodborne pathogen.
As of July 11, 2025, the Florida Department of Health reported that fatalities had occurred in Hillsborough, Bay, Broward, and St. Johns counties.
In 2024, Citrus, Hernando, Hillsborough, Lee, Pasco, Pinellas, and Sarasota Counties experienced an unusual increase due to the impacts of Hurricane Helene. Florida reported 82 cases and 19 fatalities last year.
During 2024, Pinellas County (Tampa Bay) led all Florida counties with 15 cases and three deaths.
The disease is caused by Vibrio vulnificus, a bacterium that thrives in warm water and is termed "halophilic" because it requires salt to survive, as stated by the U.S. Centers for Disease Control and Prevention (CDC).
Importantly, individuals who are immunocompromised or have a weakened immune system should wear proper foot protection to prevent cuts and injuries caused by rocks and shells on the beach, according to the CDC.
Additionally, thousands of cases are related to the consumption of contaminated food.
The CDC estimates that approximately 80,000 cases occur each year, leading to about 100 deaths annually.
The CDC recommends avoiding contact with open wounds from brackish water, salt water, and raw seafood, and thoroughly cooking oysters and other seafood before eating, to prevent infection and illness.
As of July 15, 2025, there are no approved vaccines to prevent Vibrio vulnificus-related illness.