Search API
In conjunction with the Regional Health Agencies (ARS) and mosquito control operators, Public Health France recently updated that indigenous (local) transmissions of the Chikungunya virus have been identified in mainland France.
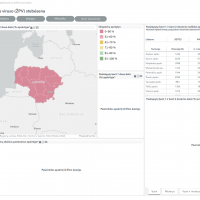
As of July 22, 2025, 38 Chikungunya cases have been confirmed in the Provence-Alpes-Côte d'Azur, Corsica, Occitanie, and Auvergne-Rhône-Alpes regions, which were already affected in previous years, and for the first time in the Grand Est and Nouvelle-Aquitaine regions.
Public Health France reiterates that the number of transmission hotspots illustrates the significant risk of indigenous transmission of these viruses in mainland France. Additional cases are likely to be identified, including those outside the usual transmission areas.
Additionally, since May 1, 2025, 833 imported cases of Chikungunya have been confirmed; many of these travelers had visited the French departments of Réunion and Mayotte.
Currently, the U.S. CDC's Level 2 - Practice Enhanced Precautions, Chikungunya Travel Health Advisory does not include southern France. However, the CDC recommends vaccination for many travelers before visiting areas with Chikungunya outbreaks.
According to recent research, preventing Chikungunya infections is essential.
Published in the Journal of Infectious Diseases on June 16, 2025, this study provides the first evidence that the chikungunya virus directly infects chondrocytes, the cells responsible for producing cartilage and may contribute to chronic musculoskeletal diseases by affecting the function of cartilage cells.
In the United States, as in Europe, two Chikungunya vaccines have been approved and are commercially available.
The ARS Auvergne-Rhône-Alpes states that most dengue cases reported in mainland France involve international travelers who were infected with the mosquito-transmitted virus while visiting a tropical region.
If people return to France infected, dengue symptoms occur on average within 4 to 7 days after the infective bite. These are considered imported cases.
However, recent reports suggest that a local outbreak may occur in July 2025.
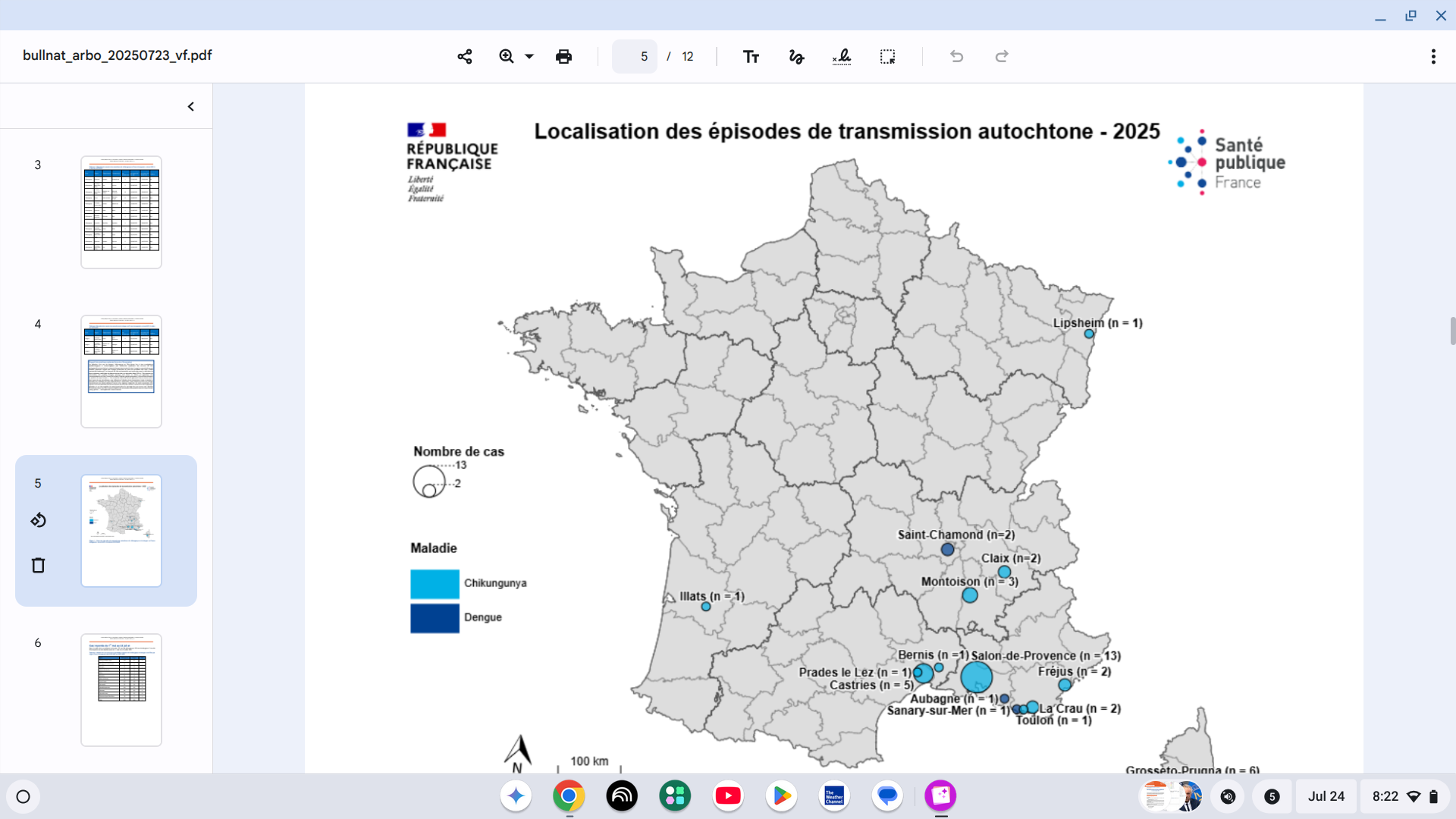
Approximately 50 kilometers southwest of Lyon, France, Saint-Chamond, in the Auvergne-Rhône-Alpes region, has confirmed a second locally acquired case of Dengue as of July 15, 2025.
'At this stage, it is not possible to establish a link with the first indigenous case identified in Saint-Chamond, as the investigations are still ongoing,' wrote ARS Auvergne-Rhône-Alpes.
An entomological survey conducted on July 18, 2025, confirmed the presence of tiger mosquitoes in areas frequented by the infected person and informed residents of an adulticide treatment. These mosquitoes carry dengue viruses.
Around one hundred homes in the affected area have been informed.
As of July 23, 2025, Sante Publique France reported a total of four locally acquired cases of Dengue for 2025.
In 2024, France reported 82 locally transmitted cases of dengue fever. Outbreaks were identified in the Provence-Alpes-Côte d'Azur, Occitanie, and Auvergne-Rhône-Alpes regions.
The World Health Organization has classified Dengue as a grade 3 emergency, with an estimated 4 billion people at risk in approximately 110 countries, including areas within the United States, such as Florida and Puerto Rico.
While numerous countries offer Dengue vaccinations, only Puerto Rico continues to provide a first-generation vaccine to children.
Note: This article was updated on July 24, 2025.
The South Carolina Department of Public Health (DPH) recently confirmed that a cat and a fox have tested positive for rabies in separate incidents that impacted people.
As of July 17, 2025, rabies is most commonly found in South Carolina (S.C.) wildlife, including raccoons, skunks, foxes, and bats.
However, most rabies cases in the United States are associated with bat bites, not dog bites.
In Greenville County, the cat that tested positive for rabies was found near Holland Ford and Beech Springs roads in Pelzer, S.C.
In 2024, six of the 81 confirmed rabies cases in S.C. were in Greenville County, which has a population exceeding 500,000.
In Marion County, the fox that tested positive for rabies was found near the intersection of Sandhill and Ellis roads in Marion. One person was exposed and has been referred to their healthcare provider. This fox is the third animal to test positive for rabies in that county in 2025.
There have been 45 cases of rabid animals in S.C. in 2025.
Since 2002, S.C. has averaged approximately 144 positive cases a year.
Terri McCollister, DPH, Rabies Program manager, commented in a press release, “Any mammal can carry and transmit the rabies virus to people or pets. Therefore, give wild and stray animals plenty of space.”
According to the DPH, rabies is a treatable and vaccine-preventable disease. Rabies information for local Public Health offices is available at dph.sc.gov/RabiesContacts. For more information on rabies, visit dph.sc.gov/rabies or cdc.gov/rabies.
The WHO Director-General recently determined that the upsurge of mpox cases in Africa continues to meet the criteria of a public health emergency of international concern and issued temporary recommendations to States Parties as of July 10, 2025.
The first human case of mpox was recorded in 1970 in the Democratic Republic of the Congo, which has subsequently spread to other central and western African countries.
According to the U.S. Centers for Disease Control and Prevention (CDC), outbreaks of clade II mpox have been reported in Liberia and Sierra Leone, where mpox is endemic.
The CDC's updated Level 2 - Practice Enhanced Precautions, Travel Health Advisory states that, unlike the ongoing global clade II mpox outbreak, which began in May 2022, these outbreaks have affected males and females approximately equally.
Furthermore, person-to-person transmission has occurred during this outbreak, including through sexual or other intimate contact.
Previously, the Ministry of Health in Cameroon confirmed the first case of mpox (Clade I) in a child from Ayos district, as of July 9, 2025.
The CDC recommends mpox vaccination (JYNNEOS®, MVA-BN®, IMVAMUNE®) for travelers to Liberia and Sierra Leone.
This advice is essential as millions of international travelers are visiting Africa.
According to the World Tourism Barometer from UN Tourism, Africa attracted approximately 74 million tourists in 2024.
Local media (ANI) reported that the Afghanistan Ministry of Public Health recently launched a polio vaccination campaign targeting 7.3 million children across 19 provinces of Afghanistan.
Healthcare providers have emphasized the crucial role of public awareness and ongoing investment in eradicating polio. Dr. Mojtaba Sufi, a health expert in the Islamic Emirate of Afghanistan, reiterated in a news article, "The only effective way to prevent polio is through vaccination, and the international community provides these vaccines.
This new vaccination campaign is essential as Afghanistan is affected by ongoing endemic wild poliovirus (WPV) transmission.
The total number of WPV1 cases in 2025 is two, which compares to 2024 when 25 cases were confirmed.
As of July 23, 2025, the U.S. CDC and the WHO's International Travel and Health recommend that all travellers to polio-affected areas be fully vaccinated against polio. Residents (and visitors staying for more than 4 weeks) from areas infected with poliovirus, such as Afghanistan, should receive an additional dose of oral or inactivated polio vaccine within 4 weeks to 12 months after travel.
Additionally, a booster dose may be recommended for specific travelers.
Currently, the CDC lists 41 countries as being at risk for poliovirus.
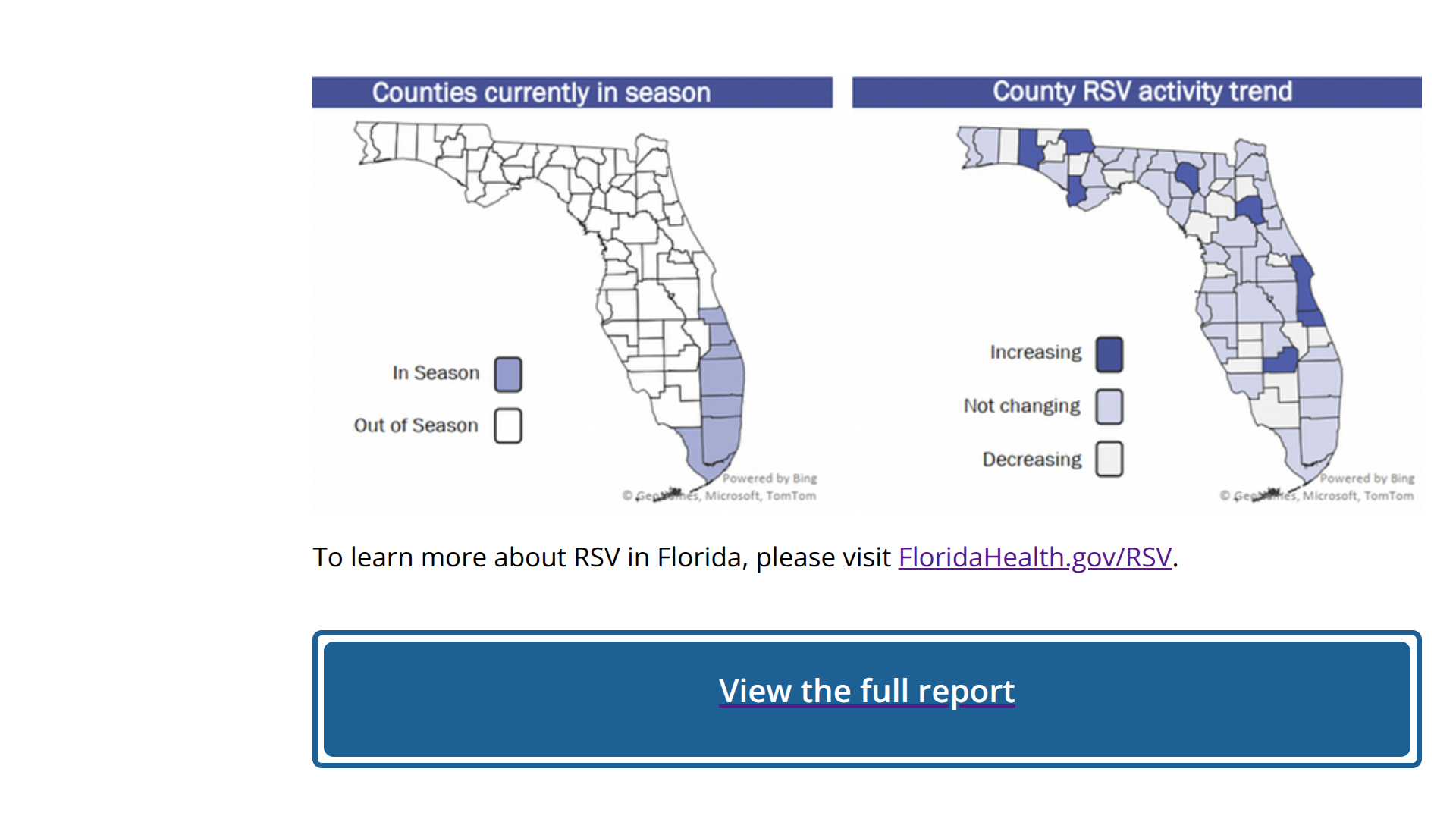
As the respiratory syncytial virus (RSV) season expands in the state of Florida, the most significant US real-world study of a single-dose long-acting antibody designed to help prevent RSV lower respiratory tract disease in infants successfully met both of its co-primary endpoints.
The full results from the "Effectiveness of nirsevimab against RSV and RSV-related events in infants" study have been published in PEDIATRICS®, an official journal of the American Academy of Pediatrics, on July 22, 2025.
Ayman Chit, Head of North America Medical, Vaccines, Sanofi, commented in a press release, "These results support BEYFORTUS (nirsevimab) as a groundbreaking advancement in infant RSV disease prevention."
"With more than 40 real-world evidence studies to date, this latest study further strengthens the well-established body of data that shows that BEYFORTUS protects against RSV disease to help safeguard the health of all babies, regardless of whether they are born before or during the RSV season."
According to the Florida Department of Health, RSV is a common respiratory virus that typically causes mild, cold-like symptoms. Young children and older adults, especially those with certain underlying health conditions, are at higher risk for severe illness from RSV.
Florida’s RSV season is longer than that of the rest of the nation and exhibits distinct regional patterns. For this reason, the state is broken up into five RSV regions, each with its own RSV season.
Austin Public Health (APH) announced yesterday that its wastewater surveillance in Travis County has detected the presence of the measles virus collected during the first week of July 2025.
As of July 21, 2025, this detection may indicate an undetected case or cases of measles in the local community that exceeds 1 million residents.
Furthermore, Austin adds another 50,000 college students each year during August and hosts over 100,000 football fans most weekends in the Fall.
So far in 2025, only two measles cases have been confirmed among Travis County residents, both of which were linked to exposure during international travel.
However, the State of Texas has reported numerous measles cases in western counties, as well as in Dallas and Houston counties.
Measles is highly contagious and is spread through the air when an infected person coughs or sneezes. The disease can actively linger in the air and on surfaces for up to two hours. If someone breathes contaminated air or touches infected surfaces and then their eyes, nose, or mouth, they can become infected.
APH says if one person has measles, 9 out of 10 unvaccinated people nearby will become infected if they are not protected.
APH offers the MMR vaccine for uninsured and underinsured Austinites at its Shots for Tots and Big Shots clinics.

With an unexpected number of chikungunya outbreaks reported in the Region of the Americas in 2025, Canada is taking action to ensure an ample supply of vaccines available.
In the past 20 years, the mosquito-transmitted chikungunya virus has emerged across many popular travel destinations.
Bavarian Nordic A/S announced today that Health Canada has accepted for review the Company's application for licensure of the single-dose, virus-like particle (VLP) chikungunya vaccine candidate, CHIKV VLP, for immunization to prevent disease caused by chikungunya virus infection in individuals 12 years of age and older.
The Directorate's acceptance of the application screening confirms that the New Drug Submission is complete, initiating a standard review procedure that may support approval of the vaccine in the first half of 2026.
Paul Chaplin, President and CEO of Bavarian Nordic, stated in a press release on July 22, 2025, "Pending approval, this vaccine will further strengthen our offering for Canadians seeking protection against serious diseases when traveling the world."
The VLP vaccine was approved by the U.S. Food and Drug Administration, the European Commission, and the United Kingdom in May 2025 under the trade name VIMKUNYA®.
In the U.S., VIMKUNYA is commercially available at clinics and pharmacies.