Search API
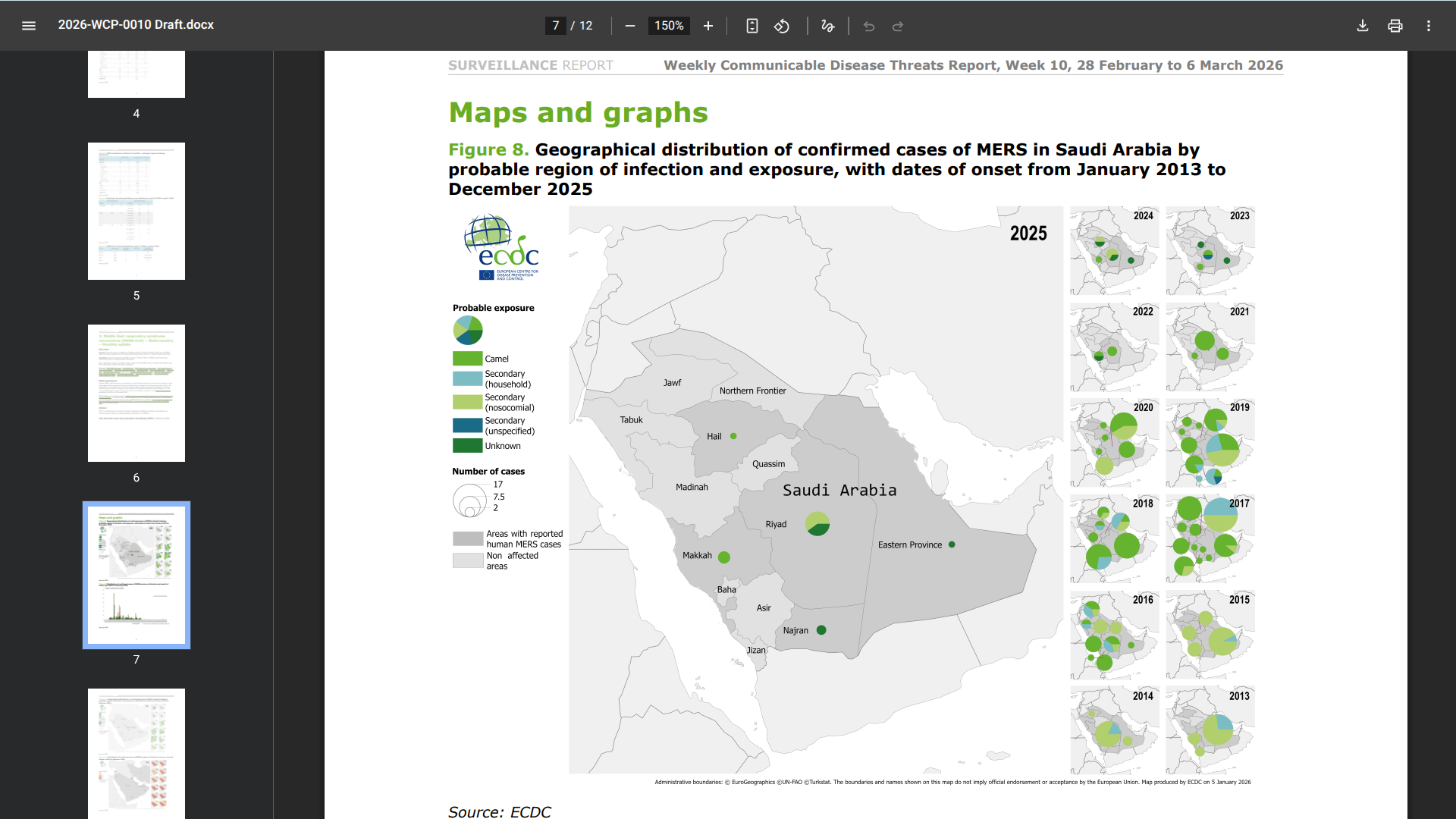
Human cases of Middle East respiratory syndrome coronavirus (MERS) continue to be reported in the Arabian Peninsula. However, the number of new MERS cases detected and reported through surveillance has dropped to the lowest level since 2014.
According to the European Centre for Disease Prevention and Control (ECDC) report dated March 6, 2026, the probability of sustained human-to-human transmission among the general population in Europe remains very low, and the impact on the general population is considered low.
Since 2012, a total of 2,647 MERS cases, including 959 deaths, have been reported by health authorities worldwide. The Kingdom of Saudi Arabia has reported the most MERS cases.
Most MERS cases are related to interactions with dromedary camels, says the ECDC.
As of March 10, 2026, no MERS vaccine has been approved.
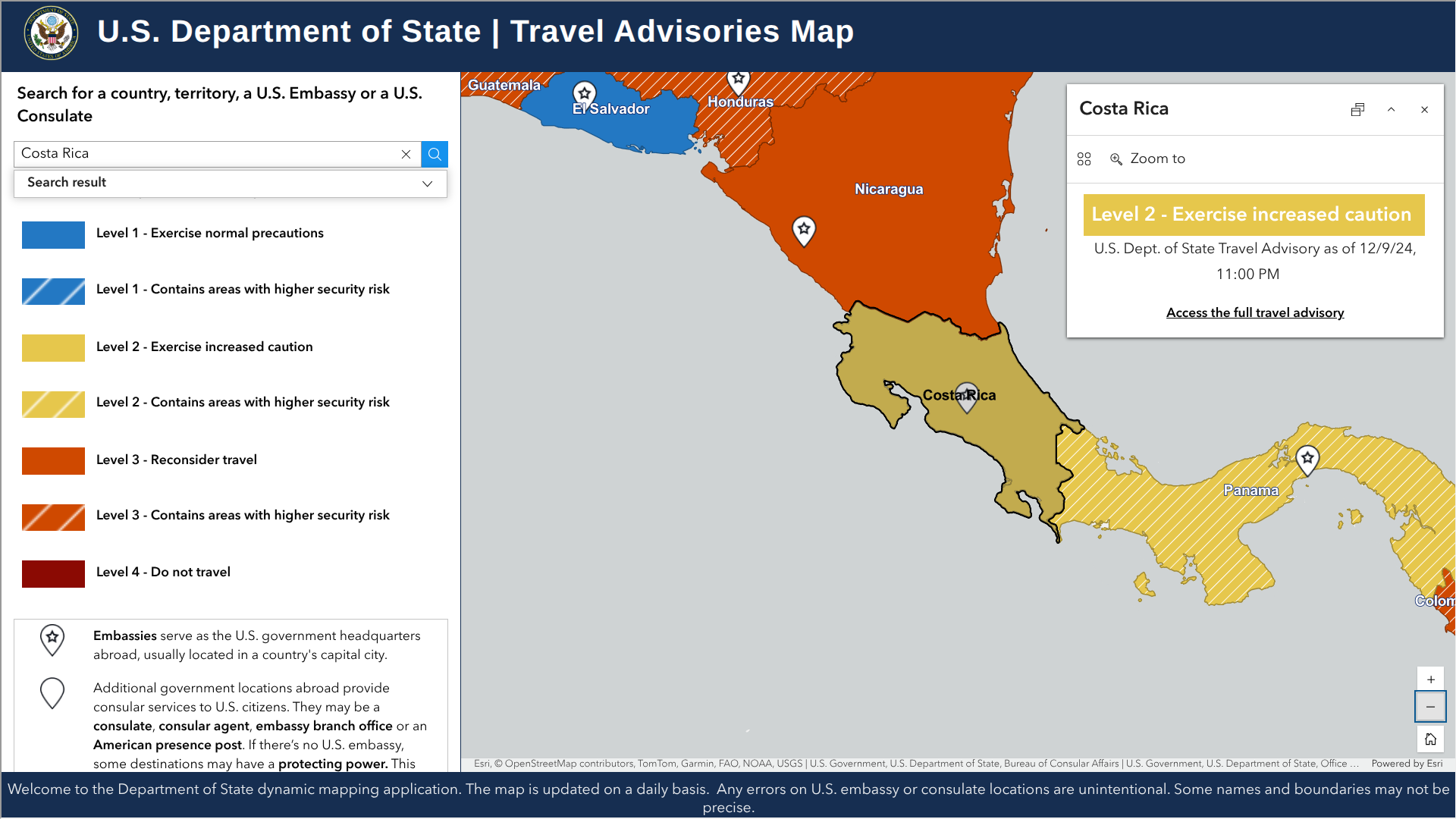
As spring break 2026 approaches, many American families and students are heading to the beaches and eco-adventures in the Republic of Costa Rica.
Given this peak travel period, visitors arriving at Juan Santamaría International Airport in San José and Daniel Oduber Quirós International Airport in Liberia are advised to stay informed about health precautions.
Today, the Costa Rica Ministry of Health confirmed a second case of measles in 2026. Health authorities, including teams from the Ministry of Health and the Costa Rican Social Security Fund, have activated epidemiological protocols. They are currently investigating potential sources of infection through contact tracing and risk factor analysis.
On March 9, 2026, the Ministry requested the temporary suspension of classes at Moravia High School and halted activities related to a program by the Ministry of Culture and Youth. Earlier this month, a measles patient was isolated to prevent further transmission of the virus.
Last year, there was an imported case of measles recorded in Guanacaste, involving an unvaccinated traveler from Canada.
The Costa Rica health agencies urge travelers, especially families with young children and those without up-to-date measles-mumps-rubella (MMR) vaccinations, to check their vaccination status. However, proof of MMR vaccination is not currently required for airport entry.
The MMR vaccine is routinely available through Costa Rica's national health system, and vaccination campaigns have been intensified due to recent alerts.
So far, no additional cases or outbreaks have been reported in connection with the current incident, and authorities are maintaining surveillance to contain any potential spread.
For the latest updates on the global measles outbreak, visit Vax-Before-Travel.com.
And for security advisories, visit the U.S. Department of State, which has published a Level 2 notice for Costa Rica.
The chikungunya epidemic in Bolivia's Santa Cruz department appears to be easing slightly. The Departmental Health Service (SEDES) has reported a noticeable decline in new cases of this mosquito-transmitted virus.
According to SEDES epidemiologist Carlos Hurtado, the latest epidemiological week recorded 655 positive chikungunya cases, a decrease of approximately 300 cases compared to the previous week.
This brings the cumulative total for 2026 in Santa Cruz, the primary epicenter of the outbreak in Bolivia, to 4,283 positive cases.
Despite this decline, the positivity rate remains high at 51%, indicating that more than half of those tested are infected with the East/Central/South African genotype of the chikungunya virus.
The U.S. Centers for Disease Control and Prevention (CDC) has issued a Level 2 Travel Health Notice for Santa Cruz and Cochabamba due to the outbreak. They advise travelers to use insect repellents, wear protective clothing, and consider vaccination where appropriate.
Bolivia is not alone in reporting chikungunya cases this year.
Recent data indicate that over 29,000 cases and 85 chikungunya-related fatalities have been reported by early March.
As of March 9, 2026, the main available vaccine option in the United States and select countries is VIMKUNYA®, a non-live virus-like particle vaccine produced by Bavarian Nordic A/S.
This travel vaccine was approved by the U.S. FDA in 2025 and is commercially available at travel clinics and pharmacies.
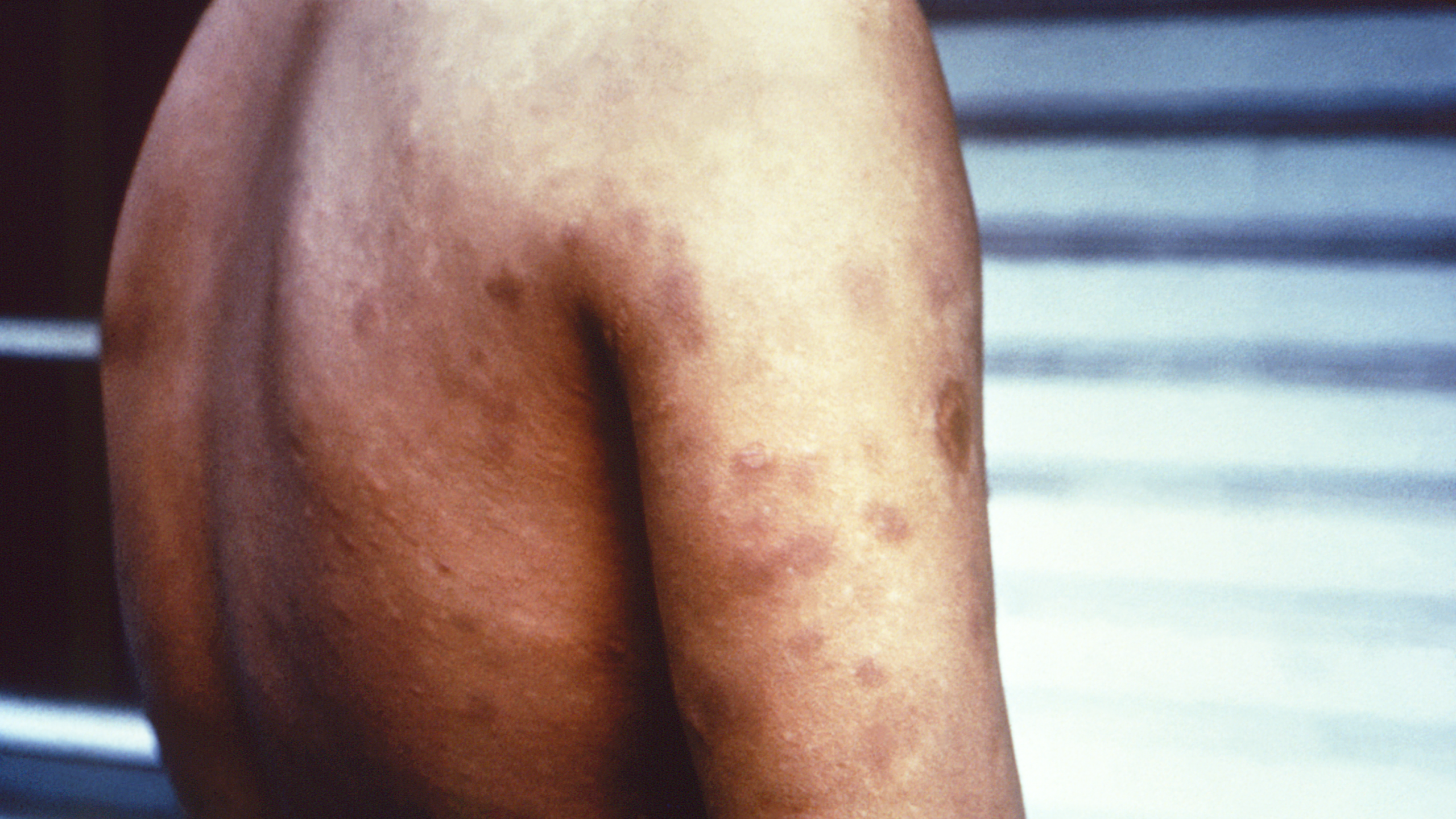
The World Health Organization (WHO), in collaboration with the Pan American Health Organization (PAHO), has officially recognized Chile as the first country in the Americas—and the second worldwide—to eliminate leprosy (Hansen's disease) as a public health concern.
This significant achievement was announced on March 4, 2026, and follows over three decades without any locally acquired cases of the disease.
Leprosy was first recorded in Chile at the end of the 19th century on Rapa Nui (Easter Island), where it became more established, affecting hundreds of residents at its peak—historical reports indicate that up to 460 cases were detected among the island's population of approximately 2,800 during earlier periods.
On mainland Chile, located on South America's east coast, cases remained sporadic and were managed through isolation, treatment, and containment efforts.
"Chile's achievement demonstrates that eliminating leprosy is possible and requires the establishment of strong systems to detect, respond to, and provide comprehensive care for those affected by the disease, including individuals living with chronic disabilities," stated PAHO Director Dr. Jarbas Barbosa in a media release.
"Being the first country in the Americas to be confirmed as having eliminated leprosy sends a powerful message to the region—that diseases strongly linked to vulnerable populations can be eradicated, thereby disrupting the vicious circle between disease and poverty."
In the United States, the CDC reported 205 new leprosy cases nationwide in 2024.
Florida specifically recorded 20 confirmed cases.
While there is no specific vaccine for leprosy, the Bacille Calmette-Guérin (BCG) vaccine, primarily used against tuberculosis, has been shown in global studies to offer partial protection (20% to 80%) due to antigenic similarities between the bacteria.
BCG vaccination value depends on factors such as age, dosage, and particularly when administered in childhood.
However, Chile's success was achieved primarily through integrated strategies focused on treatment, surveillance, and transmission prevention, rather than relying solely on vaccination.
Recent detections of poliovirus in London's wastewater have led the U.S. Centers for Disease Control and Prevention (CDC) to update its global travel health notice to include the United Kingdom.
This CDC advisory, classified as Level 2 – Practice Enhanced Precautions, was issued on March 3, 2026, and highlights the ongoing risk of poliovirus circulation in over 30 countries, where environmental surveillance has found traces of the virus in sewage samples.
In the UK, detections have primarily been concentrated around the Beckton Sewage Treatment Works, which serves millions of residents in northern and eastern London. According to the UK Health Security Agency (UKHSA), a circulating vaccine-derived poliovirus type 2 (cVDPV2) was identified in an environmental sample collected around January 28, 2026.
Investigations into the source of the cVDPV2 detections in London are ongoing and may be linked to international arrivals.
This indicates a continued presence of poliovirus in the UK's wastewater system, following earlier discoveries in late 2024 in locations such as East Worthing, Leeds, and London's Beckton and Crossness treatment plants.
Notably, similar UKHSA detections in London's sewage began in 2022.
While no cases of paralytic polio have been reported in the UK since 1984, these environmental detections suggest potential silent transmission in communities with low vaccination rates. Health officials emphasize the importance of maintaining high vaccination coverage to prevent any resurgence of the virus.
Vaccine-derived poliovirus occurs when the weakened live virus used in oral polio vaccines (OPV) mutates and regains the ability to spread in under-immunized populations. Although the UK switched to the inactivated polio vaccine (IPV) in 2004, which does not carry this risk, global travel and migration can introduce strains from regions where OPV is still used.
The updated CDC advisory includes endemic hotspots like Afghanistan, Pakistan, and Nigeria, as well as non-endemic countries such as the UK, Germany, Finland, and Spain, where wastewater detections have been reported. CDC experts highlight that wastewater surveillance acts as an early warning system, enabling public health officials to intervene before outbreaks occur.
The notice states, "Some international destinations have circulating poliovirus," urging travelers to ensure they are up to date on their polio vaccines before any international trip.
The CDC advises clinicians to prioritize completing the IPV series for individuals who are unvaccinated or incompletely vaccinated and planning to travel. They emphasize that polio can lead to lifelong paralysis or death in rare cases.
The CDC also recommends a single lifetime IPV booster dose for adults who have completed the full routine polio vaccine series before visiting affected areas.
In numerious countries, the novel OPV (nOPV2) vaccine has been administered over 2 billion times in the past few years.
With global efforts intensifying, there is hope that these early alerts will keep the UK and other nations one step ahead of the virus, according to the CDC.
The U.S. Department of State's Worldwide Caution remains in effect, advising U.S. citizens to exercise increased caution globally due to potential security risks.
On March 7, 2026, the U.S. Embassy in Abu Dhabi issued an urgent security alert, urging American citizens in the United Arab Emirates (UAE) to prioritize their safety while traveling in the Middle East.
This region is a popular international destination; for instance, in 2025, Dubai welcomed 1.4 million visitors from the Americas, accounting for approximately 7% of the emirate's 19 million international overnight visitors.
The embassy stated that it is actively working to provide additional departure options for U.S. citizens wishing to leave the Middle East. Limited international flights continue to operate from major UAE airports, including those in Abu Dhabi and Dubai.
Currently, airport access is restricted to confirmed passengers only, and travelers should proceed to the airport only if they have a confirmed ticket and explicit instructions from their airline.
If air departure is not feasible or not chosen, the embassy recommends sheltering in place at a secure location, such as a residence or safe building. Individuals should prepare supplies of food, water, medications, and other essentials to sustain themselves during potential disruptions.
Americans are encouraged to monitor their email closely for updates or last-minute changes, remain vigilant, follow instructions from local UAE authorities, and review ongoing embassy guidance. To receive tailored assistance and timely updates, U.S. citizens should complete the Department of State's crisis intake form at https://mytravel.state.gov/s/crisis-intake if they have not already.
For the most current information, Americans should refer directly to the U.S. Embassy in Abu Dhabi's website (ae.usembassy.gov) or the State Department's travel advisories page.
Seperately, the U.S. CDC advises various routine and travel vaccinations for visiting this area of the Middle East in 2026.
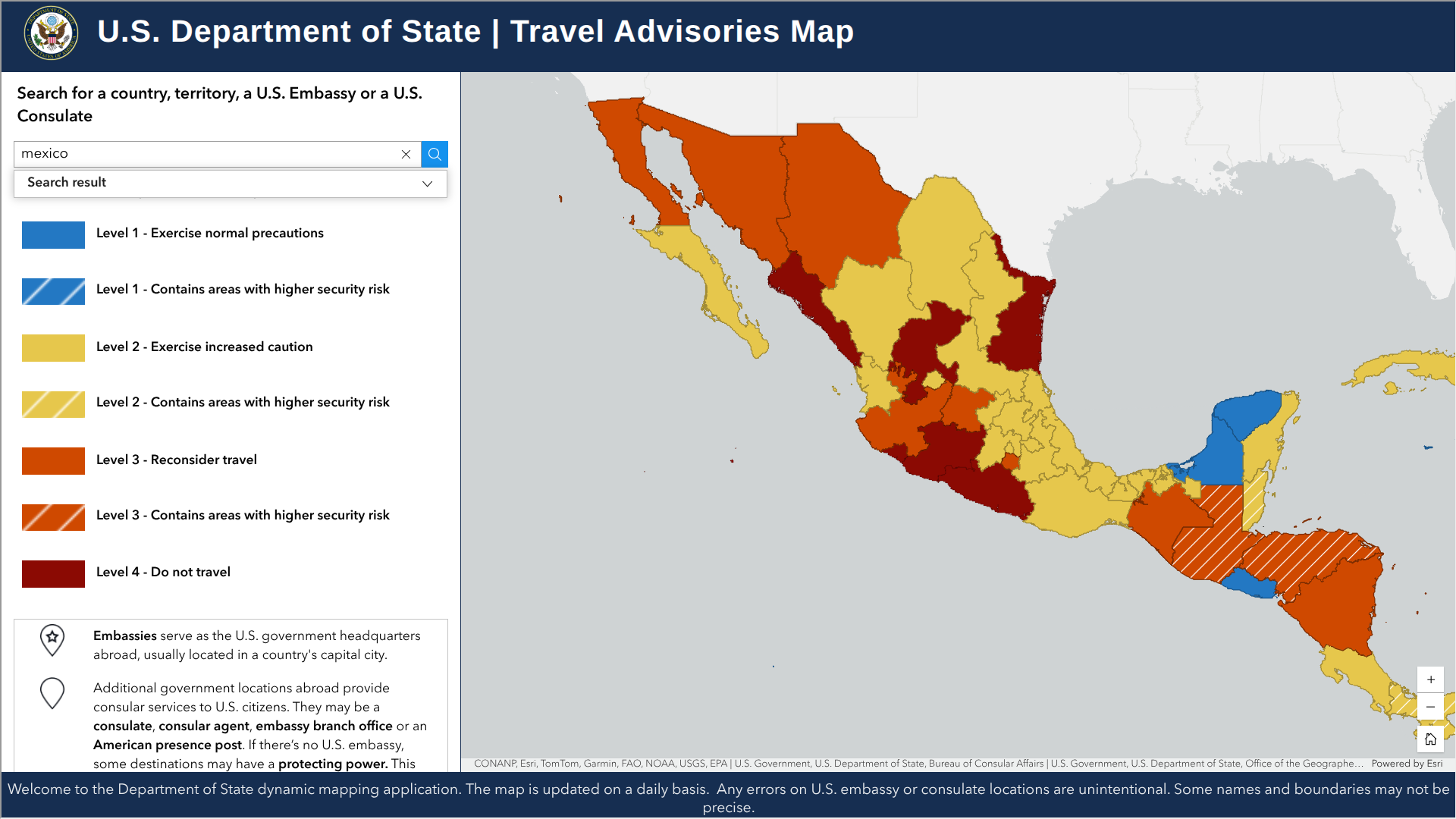
The U.S. Department of State has issued an important reminder for Americans planning spring break trips to Mexico. Travelers are urged to remain aware of ongoing safety risks, even though recent widespread violence has lessened.
In a Message to U.S. Citizens released on March 2, 2026, the U.S. Embassy in Mexico emphasizes the importance of personal responsibility with the slogan: "Travel Smart – Be Informed."
The State Department advisory states that while large-scale unrest, triggered by Mexican security operations on February 22, 2026, has subsided, risks such as crime and kidnapping persist.
As spring break 2026 attracts large crowds to Mexico's beaches and resorts, officials stress the importance of reviewing the full advisory and the country information page at travel.state.gov. Travelers are encouraged to stay informed by closely monitoring updates, as security situations can change quickly.
Mexico currently holds an overall Level 2 advisory: Exercise Increased Caution. However, conditions vary greatly by region, with six states classified as Level 4: Do Not Travel in 2026.
Furthermore, the U.S. CDC has identified a significant number of health risks in Mexico.
For emergencies when visiting Mexico, contact the U.S. Department of State's Consular Affairs line at +1-888-407-4747 or +1-202-501-4444.
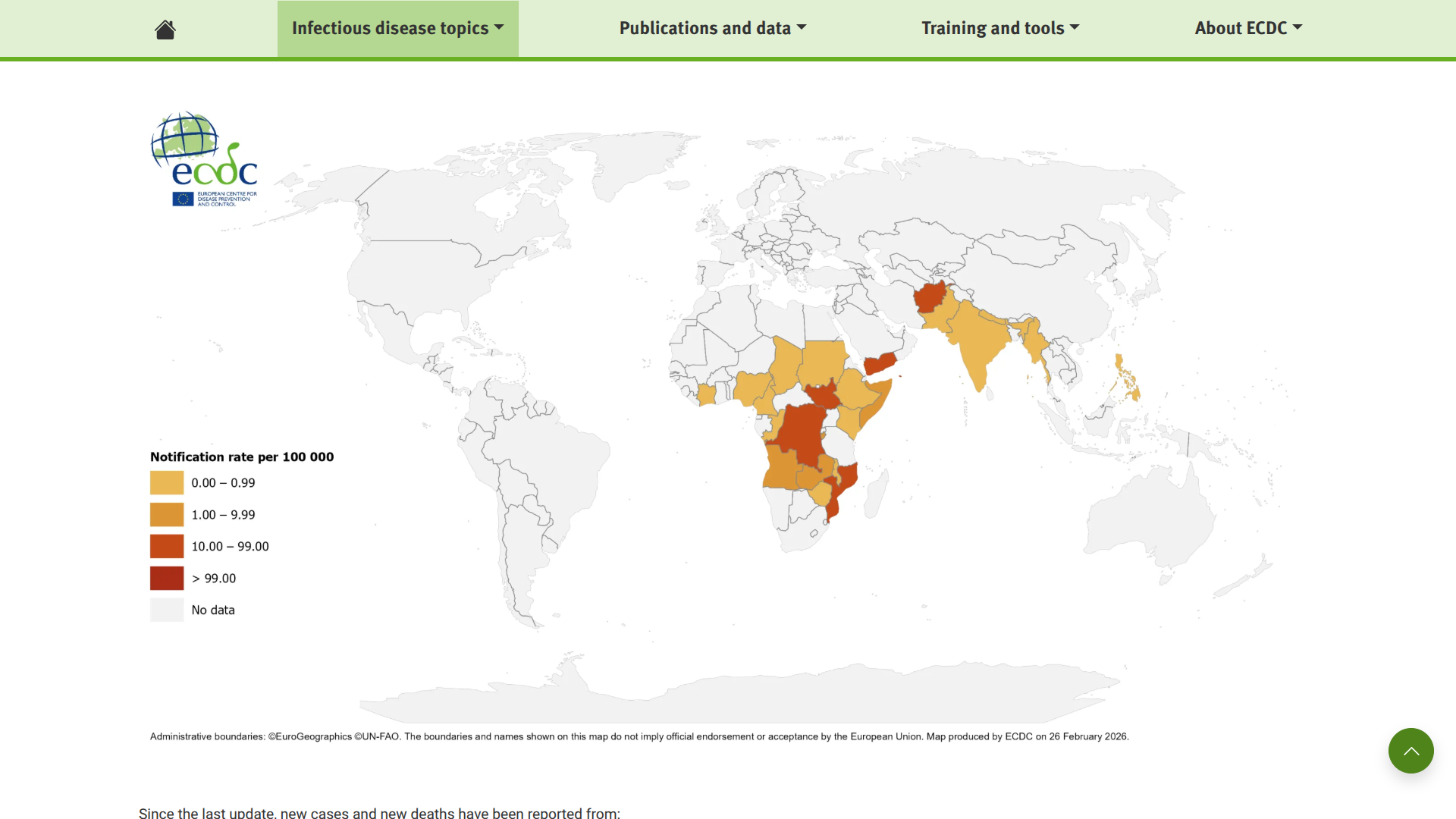
Cholera outbreaks continue to impact multiple regions, according to the latest data from the World Health Organization (WHO) and the European Centre for Disease Prevention and Control (ECDC).
Despite some fluctuations in global cases, cholera remains a significant public health concern in early March 2026.
According to the have been over 25,000 reported cholera cases worldwide this year, including 282 related deaths.
For the entirety of 2025, the WHO reported a cumulative total of 614,828 cholera cases and 7,598 deaths across 33 countries in five regions, with the Eastern Mediterranean and African regions experiencing the heaviest burden.
For most other travelers, vaccination is not routinely advised.
The WHO emphasizes that cholera is both preventable and treatable with prompt rehydration.
The WHO prequalifies several oral cholera vaccines (OCVs), including Dukoral®, Shanchol™, and Euvichol®, as well as variants such as Euvichol-Plus® and Euvichol-S®.
These OCVs generally require two doses to provide full protection and are utilized in both travel settings and mass vaccination campaigns through the Global OCV Stockpile.
In early 2026, preventive vaccination programs resumed with an initial allocation of 20 million doses, including deliveries to high-burden countries like Mozambique, the Democratic Republic of the Congo, and Bangladesh.
The WHO and ECDC say travelers planning to visit affected areas should consult travel health clinics for personalized risk assessments and potential vaccination.