Search API
Despite the United Kingdom (UK) maintaining high vaccination coverage and remaining polio-free for decades, recent detections of poliovirus in wastewater have emerged as a significant early warning signal.
As of January 28, 2026, the Global Polio Eradication Initiative (GPEI) reported the detection of a circulating vaccine-derived poliovirus type 2 (cVDPV2) in an environmental sample in the UK.
This finding was part of routine wastewater surveillance conducted by the UK Health Security Agency (UKHSA) and is part of ongoing efforts to monitor for poliovirus in sewage systems.
This recent detection aligns with a pattern of similar findings in the UK. Previous cVDPV2 detections in the UK during 2025 and late 2024 were linked to specific sites, for example:
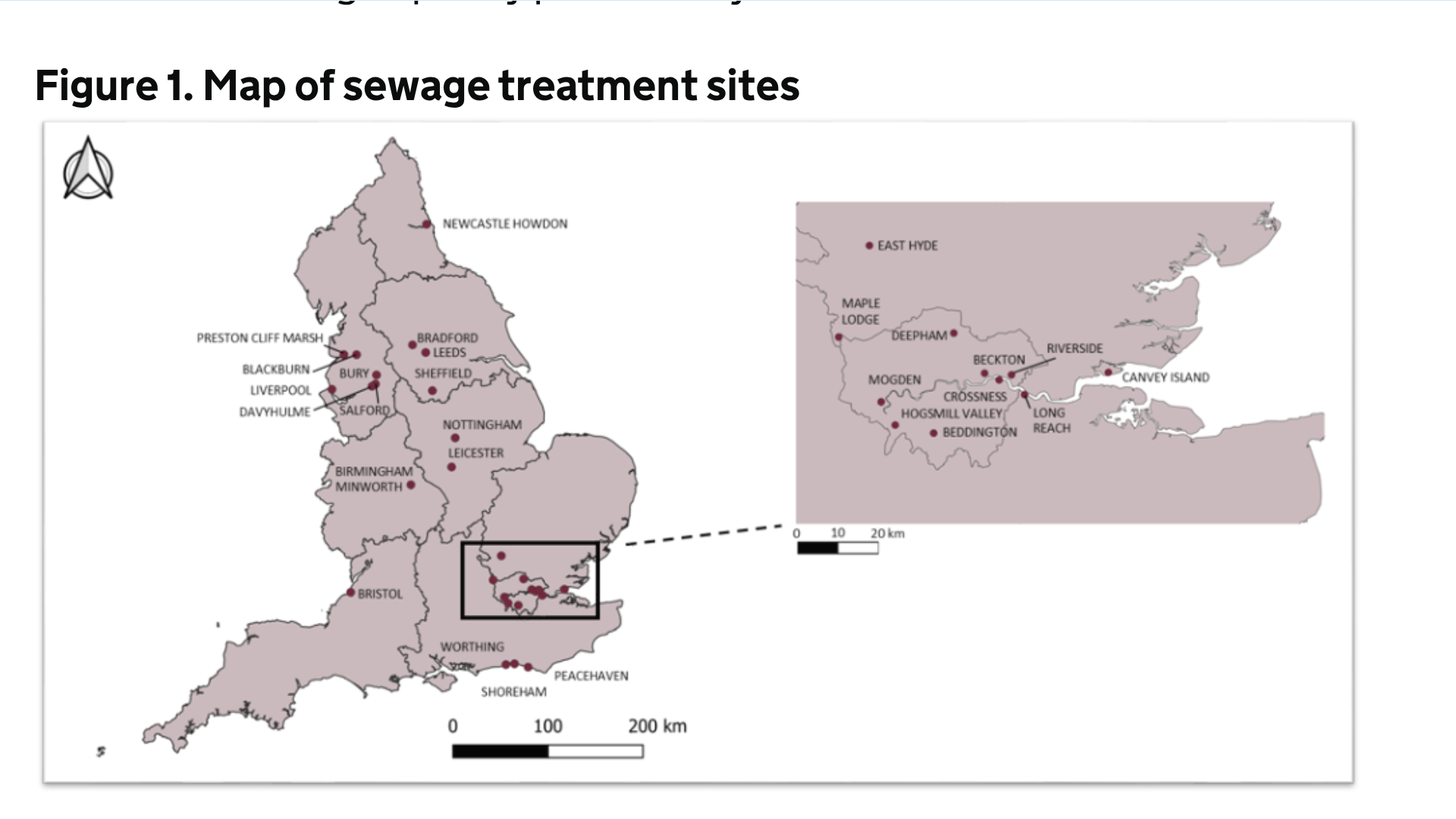
A single sample from Shoreham STW on January 20, 2025 (with follow-up negative).
Other 2025 instances in regions such as Yorkshire and the Humber (September 2025 sample).
Detections in late 2024 from East Worthing STW (covering parts of West Sussex), Leeds Knostrop STW, and London Beckton/Crossness STWs.
In June 2022, UKHSA announced that environmental surveillance for polio had consistently detected poliovirus in sewage samples collected from the Beckton Sewage Treatment Works in London.
Additional cases were noted in sources like the GPEI's weekly updates and UKHSA reports.
The strain involved in the recent UK detections has often been genetically linked to broader international clusters. In late 2024 and into 2025, a specific genetic cluster of cVDPV2—originating from lineages first observed in Nigeria—was detected in wastewater across multiple European countries, including the UK.
These detections underscored the risk of importation and silent circulation in under-vaccinated areas, prompting calls from the U.S. Centers for Disease Control and Prevention (CDC).
As of January 30, 2026, the CDC's Level 2 - Practice Enhanced Precautions, Travel Health Notice lists 32 countries, including the UK. The CDC advises speaking with a travel vaccine advisor about immunization options before visiting countries at high risk for poliovirus.
CDC health experts say that as long as the poliovirus circulates anywhere, the risk of importation persists, even in polio-free regions.
Philadelphia health officials are raising concerns about a noticeable increase in chickenpox (varicella) cases among unvaccinated children in the city.
In early 2026, the Philadelphia Department of Public Health (PDPH) reported two separate outbreaks at two schools in eastern Pennsylvania.
On January 5, 2026, the PDPH issued a health advisory to clinicians and the public. The advisory emphasized the importance of recognizing, managing, controlling, and preventing varicella.
In November 2025, PDHP issued a similar health alert about chickenpox cases in schools.
This situation underscores ongoing worries about vaccine-preventable diseases in schools. Currently, the student population in Philadelphia exceeds 1.6 million from kindergarten through 12th grade.
Gayle Mendoza, a spokesperson for the PDPH, told the Inquirer on January 27, 2026, that she had no details on how many cases were reported among vaccinated versus unvaccinated children. It's also unclear which factors have contributed to the rise in chickenpox cases.
Although the current outbreaks are limited in scope, officials stress the necessity of maintaining high vaccination rates to prevent a wider spread of this once-common childhood illness.
During 2025, the U.S. CDC data indicates fewer than 150,000 cases reported annually in recent years. Hospitalizations were under 1,400, and deaths were around 30 or fewer.
Chickenpox can pose serious risks to vulnerable populations, including pregnant individuals, newborns, and those with weakened immune systems.

The Regional Health Agency (ARS) of French Guiana has announced the detection of the territory's first locally acquired case of chikungunya. The individual, who had not traveled in the 15 days before the onset of symptoms, tested positive for the virus on January 21, 2026.
As of January 27, 2026, ARS described this chikungunya case in a press release as isolated, with no evidence of wider transmission of the mosquito-borne viral disease in this French department on the northeast coast of South America.
While no large-scale outbreak was reported in French Guiana during 2025, the new locally acquired case indicates the need for renewed vigilance. Health authorities in French Guiana are implementing standard response measures, including enhanced mosquito control, public education on eliminating breeding sites, and surveillance to monitor for additional cases.
Currently, ARS emphasized that, while this remains an isolated case, continued monitoring is essential given the virus's transmission dynamics and the presence of vectors in the territory.
This development in French Guiana occurs amid significant chikungunya activity in French overseas departments and territories throughout 2025. The virus experienced a considerable resurgence in the Indian Ocean region, particularly in La Réunion, where a large-scale outbreak began in late 2024 and peaked in early 2025.
By mid-September 2025, La Réunion had reported over 54,500 confirmed cases and 40 deaths.
In early 2026, the Pan American Health Organization reported that Brazil (180) and Suriname (39) had reported confirmed chikungunya cases in the region this year.
In the United States, one local case was confirmed in Florida as of week #3 in 2026.
And off Florida's southeast coast, Cuba has confirmed a significant number of chikungunya cases.
Chikungunya has no specific antiviral treatment; management focuses on relieving symptoms through rest, hydration, and pain relievers. Prevention through vector control remains the cornerstone of response efforts.
Additionally, a U.S. FDA-approved single-dose aluminum hydroxide-adjuvanted, non-live, virus-like particle vaccine chikungunya vaccine is available at travel clinics in the U.S.
The National Centre for Disease Control (NCDC) today confirmed in a statement that only two cases of Nipah Virus Disease (NiVD) have been reported in West Bengal from December 2025 to date.
These two confirmed cases mark the first reported Nipah incidents in West Bengal in nearly two decades, following a previous outbreak in 2007.
A total of 196 contacts linked to the confirmed cases were identified, traced, monitored, and tested; all were found to be asymptomatic and tested negative for NiVD.
As of January 27, 2026, no additional cases have been detected in West Bengal, a state in eastern India, between the Himalayas mountains and the Bay of Bengal.
The Ministry stated that the situation remains under constant monitoring, with all necessary public health measures in place to prevent any further spread.
Nipah virus, a zoonotic pathogen transmitted primarily from fruit bats or through contaminated food, can cause severe illness in humans. However, human-to-human transmission is possible in close-contact settings.
Regarding disease prevention, Nipah virus vaccine candidates include live-attenuated and replication-defective recombinant platforms based on poxviruses, VSV, adenovirus, measles, rabies, and virus-like particles, as well as subunit vaccines.
These vaccines have not been approved by any government agency.
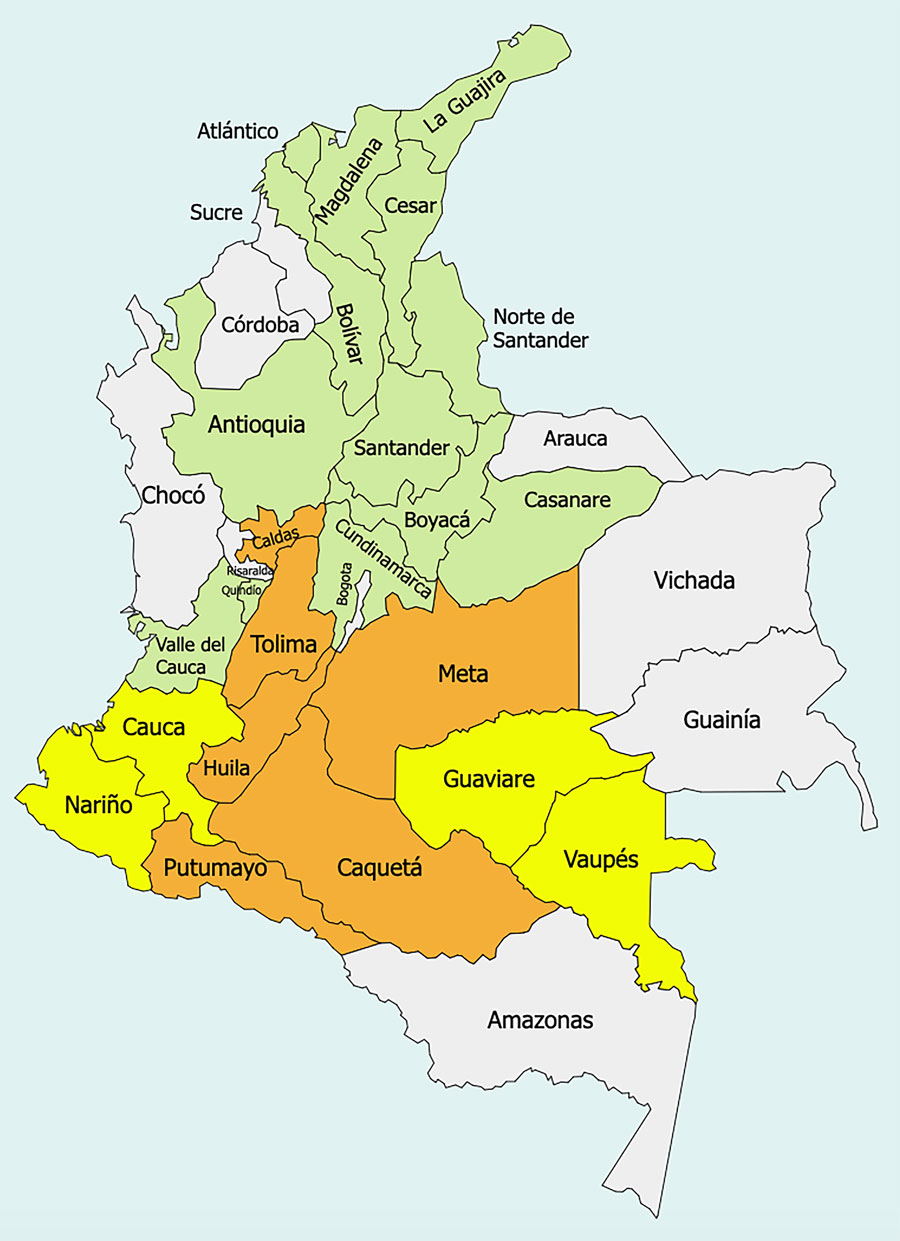
The Republic of Colombia has issued an updated health alert for yellow fever following 13 confirmed cases and 10 deaths in early 2026.
Among the fatalities are three Bogotá residents who contracted the yellow fever virus (YFV) while traveling to endemic areas, such as the department of Tolima.
This data is concerning, given that Bogota has a population of around 8 million.
According to a Ministry of Health bulletin from January 26, 2026, the outbreak's case-fatality rate of approximately 77% underscores its severity.
The Ministry also reported that from 2024 to late January 2026, there have been 161 confirmed cases nationwide, resulting in 73 deaths.
Previously, the U.S. CDC Emerging Infectious Diseases, Volume 31, Number 12—December 2025, confirmed the reemergence of YFV in the Magdalena Valley, Colombia, between 2024 and 2025.
The CDC wrote, Immediate, comprehensive measures, including mass vaccination, genomic surveillance, and integrated One Health frameworks, are urgently needed. Colombia's experience underscores the need to reevaluate risk stratification and preparedness strategies across the Americas to prevent future yellow fever outbreaks in previously unaffected regions.
Health officials stress that yellow fever is preventable with a single-dose vaccine available free of charge in Colombia and commercially offered in the United States.
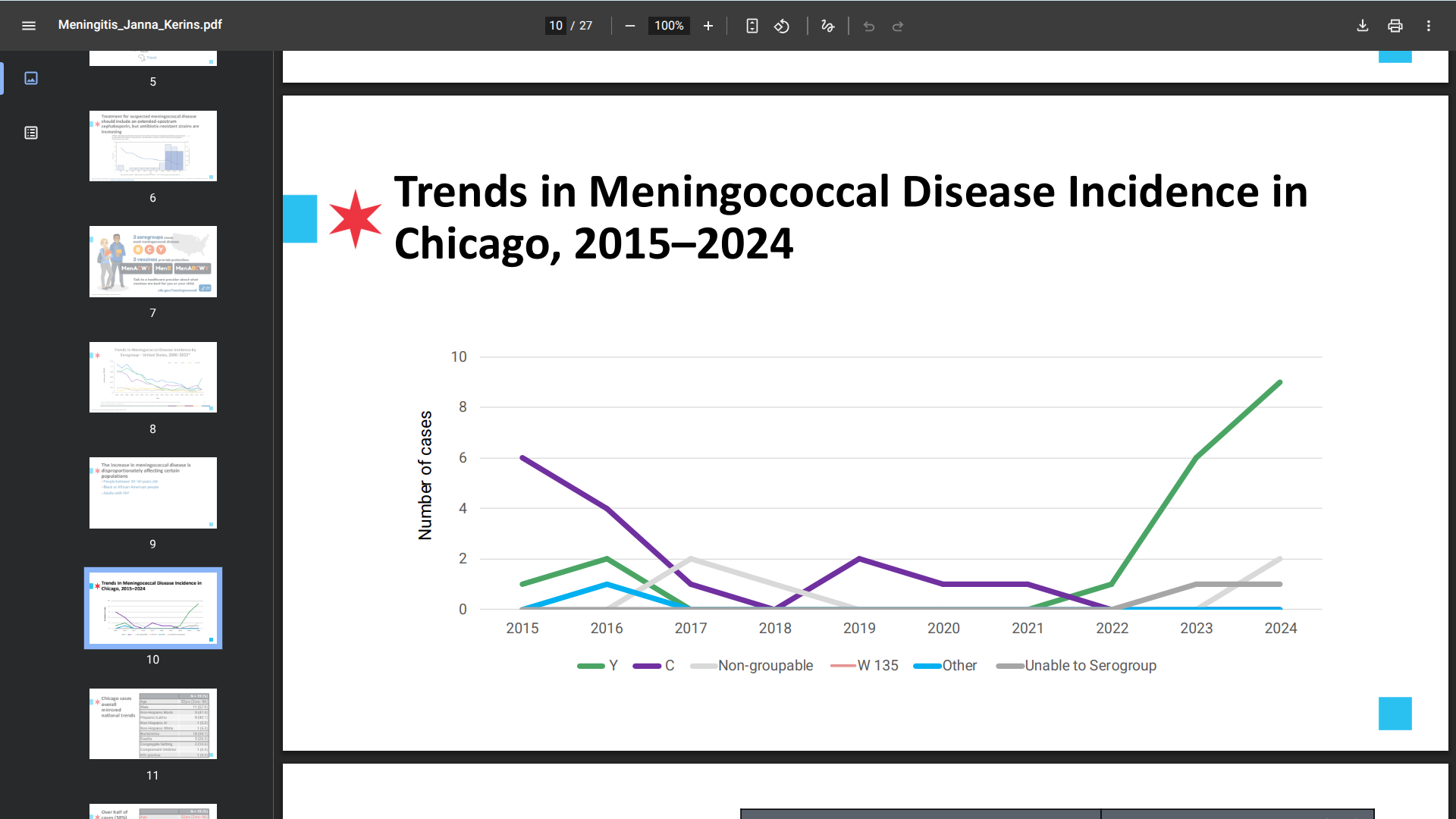
Health officials in Chicago are investigating a concerning cluster of invasive meningococcal disease (IMD) cases since January 15, 2026. This investigation is essential as IMD, caused by Neisseria meningitidis, has a case-fatality rate of 10–15%.
The Chicago Department of Public Health (CDPH) recently reported that four patients developed septicemia, with one also showing symptoms of meningitis. Three individuals required intensive care due to septic shock.
Importantly, the two community-acquired cases have no known links to each other or a temporary shelter, prompting ongoing investigations. Laboratory analysis confirmed that three cases belong to serogroup Y, the predominant strain in Chicago since 2022.
Previously, Janna Kerins, VMD, MPH, Medical Director at CDPH, reported 19 cases of N. meningitidis among Chicago residents in 2022-2024, compared with 1–3 cases annually from 2017 to 2022.
The Health Alert advised healthcare providers to maintain a high index of suspicion for N. meningitidis in individuals presenting with clinically compatible symptoms.
To contain the outbreak in late January 2026, the CDPH is providing post-exposure prophylaxis to close contacts of the affected individuals and coordinating educational efforts and vaccination clinics at the shelter and a newly relocated facility.
Seperately, the U.S. Centers for Disease Control and Prevention (CDC) says cases of meningococcal disease have increased sharply since 2021. In 2024, 503 confirmed and probable cases were reported, according to preliminary data.
As of January 28, 206, this is the most significant number of U.S. meningococcal disease cases reported since 2013.
The CDC confirms meningococcal vaccines are the best way to protect people against meningococcal disease, but side effects can occur.
For more information about Chicago's latest outbreak, visit the CDPH website or contact local health services.