Search API
The Republic of Colombia Ministry of Health recently posted on Facebook that it has seen a rise in yellow fever cases over the past two years.
From 2024 to January 4, 2026, Colombian officials reported 142 confirmed cases. This includes 63 deaths.
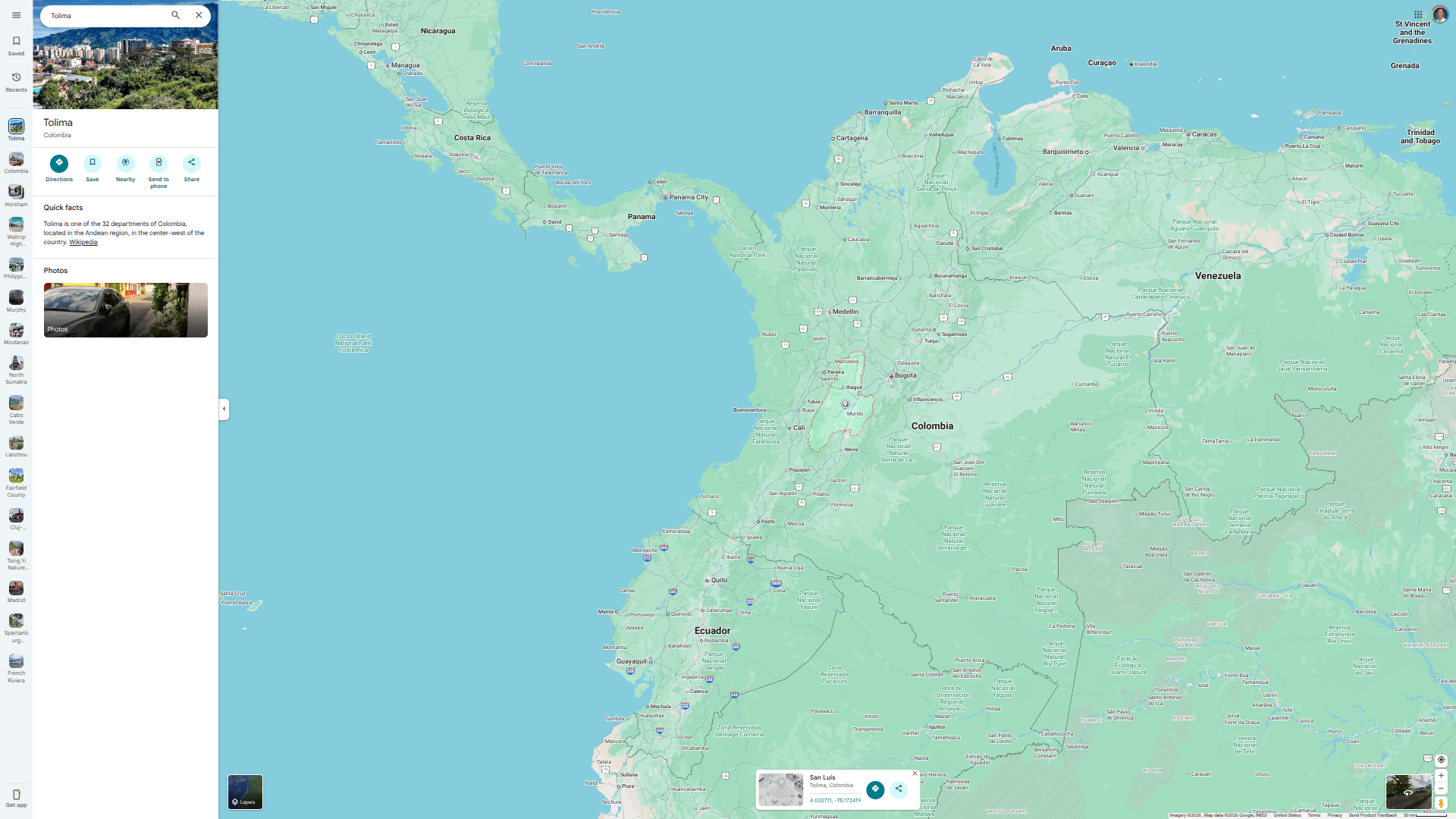
The mosquito-transmitted disease has been detected in ten departments, each with at least one death from yellow fever. These are Caldas, Caquetá, Cauca, Guaviare, Huila, Meta, Nariño, Putumayo, Tolima, and Vaupés.
While some of these yellow fever cases have occurred in forest areas, others have been reported near Bogotá, the capital city and a tourist destination.
Over the last few years, Tolima, located west of Bogota, has been the most affected area, often accounting for over 80% of yellow fever cases.
According to the World Health Organization and the U.S. Centers for Disease Control and Prevention, the yellow fever vaccine is among the most effective available. It is a live, attenuated vaccine that provides lifelong protection with a single dose for most people.
No booster doses are routinely needed. However, as of January 5, 2026, travel vaccine experts are available to provide insights on yellow fever immunization.
From a security perspective, the United Kingdom (UK) updated its travel advice on January 5, 2026, advising against all but essential travel to parts of Colombia, such as the Colombia-Venezuela border and northern Colombia.
The UK wrote that if you choose to travel to Colombia in 2026, research your destinations and get appropriate insurance.
The U.S. Centers for Disease Control and Prevention (CDC) is hosting today a Clinician Outreach and Communication Activity (COCA) Call titled "From Cave to Clinic: Managing Histoplasmosis in Returning Travelers."
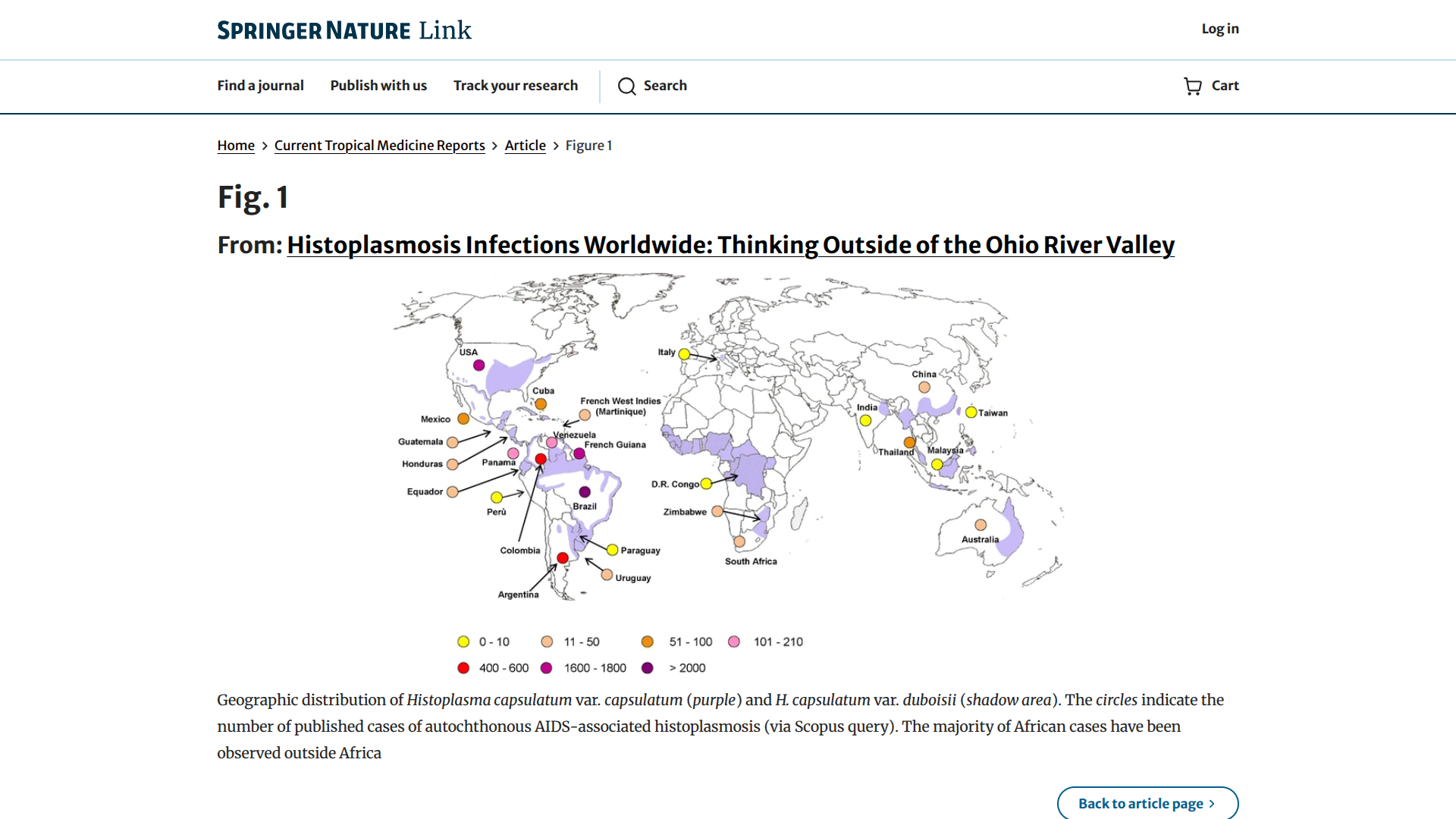
On January 15, 2026, COCA Call presenters will share current evidence on the epidemiology of travel-associated histoplasmosis, with a focus on cave-associated outbreaks, for travelers visiting Central and South America.
Histoplasma, a fungal infection that primarily impacts people's lungs, is endemic, especially in Latin America and the Caribbean, and is often found in the Ohio and Mississippi River valleys in the U.S.
The CDC's MMWR stated in May 2025 that people may be at increased risk for Histoplasma exposure when engaging in adventure activities such as cave exploration, ecotourism, or other activities that disturb contaminated soil or aerosolize fungal spores.
The CDC highlighted a histoplasmosis outbreak among 12 family members returning from the Central American country of the Republic of Costa Rica after visiting Venado Caves. The same bat-inhabited cave in Costa Rica associated with this 2024 histoplasmosis outbreak was linked to a 1998–1999 outbreak among 51 persons.
Histoplasmosis is a fungal infection caused by the dimorphic fungus Histoplasma, which is found in soil. It also spreads through bird and bat droppings that mix into the soil. Illness can range from asymptomatic or mild respiratory disease to severe acute pulmonary or disseminated disease, especially in immunocompromised individuals.
On January 5, 2025, the CDC wrote that clinicians and healthcare providers are encouraged to join this free webinar to stay informed on emerging risks, particularly following recent outbreaks linked to bat-inhabited caves.
International travelers interested in cave exploration may also attend this digital session.
For more information and to register, visit the COCA Call page at: https://www.cdc.gov/coca/hcp/trainings/from-cave-to-clinic-managing-hist...
Note: an earlier version of this COCA announcement was posted.
In Hong Kong, several mosquito-borne diseases were reported in 2025, including chikungunya fever (CF).
As of January 3, 2026, the Centre for Health Protection (CHP) of the Department of Health announced a total of 82 confirmed CF cases for the previous year.
Among these, 11 were local cases, while the remainder were imported.
Due to some local cases of CF being linked to visits to the Tsing Yi Nature Trails or nearby areas in November of last year, the trails are currently closed until further notice.
The CHP is urging the public to avoid entering the Tsing Yi Nature Trails, located northwest of the city of Hong Kong, to reduce the risk of contracting CF and to prevent exposure to chemicals or interference with mosquito control operations.
The CHP continues to advise anyone who has recently hiked along the Tsing Yi Nature Trails to seek medical attention promptly if they experience any relevant symptoms. This area of Hong Kong has about 190,000 residents.
For inquiries, the CHP says to please call the hotline at 2125 2373.
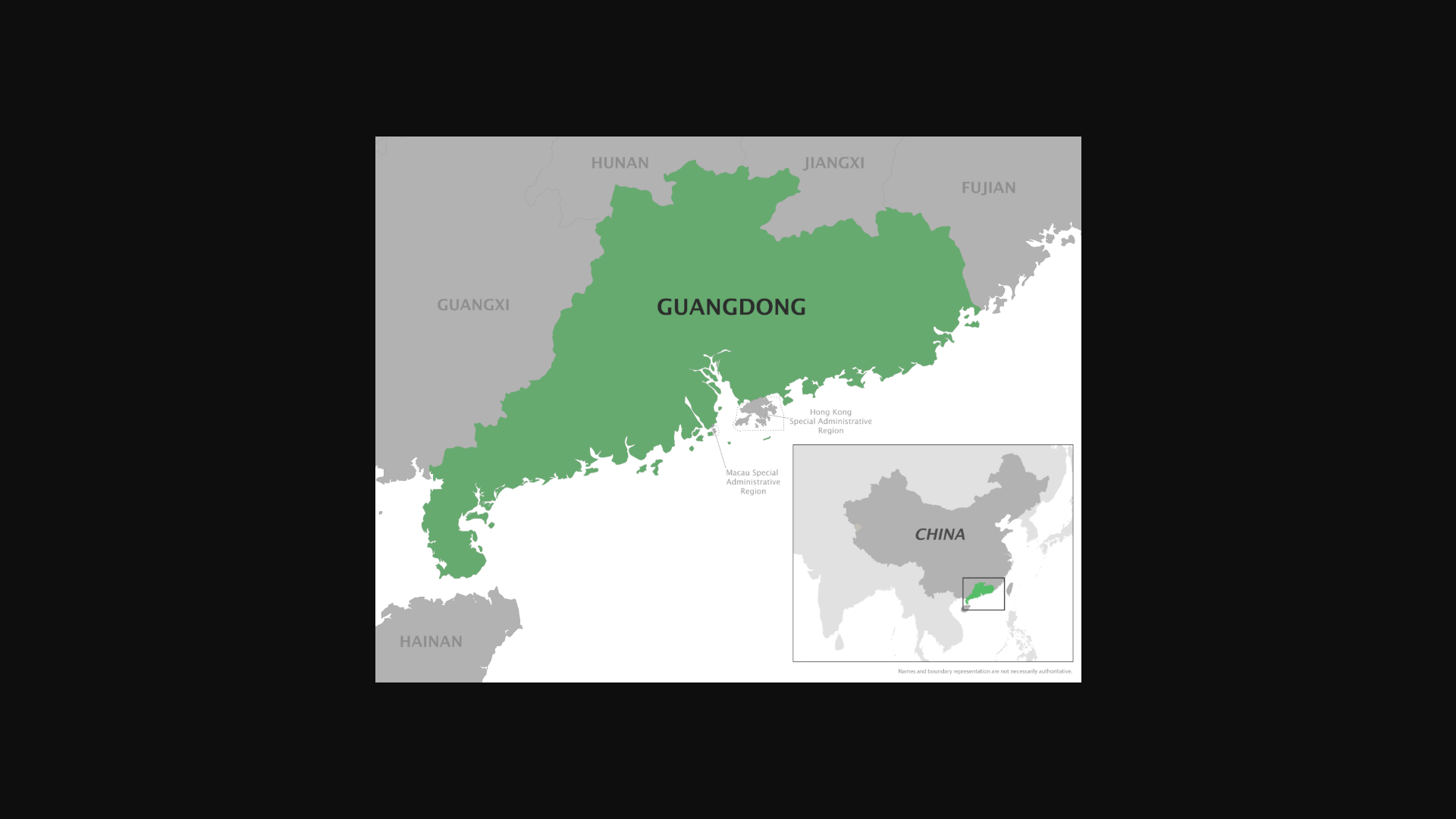
According to the U.S. Centers for Disease Control and Prevention (CDC), the Hong Kong Special Administrative Region is not the only area within China impacted by the spread of the chikungunya virus in 2026.
The CDC reports there is a chikungunya outbreak in Guangdong Province.
The CDC's Level 2 travel advisory recommends vaccination for travelers visiting an area with a chikungunya outbreak. When departing from the USA for abroad in 2026, travel vaccines will be available for purchase at various clinics.
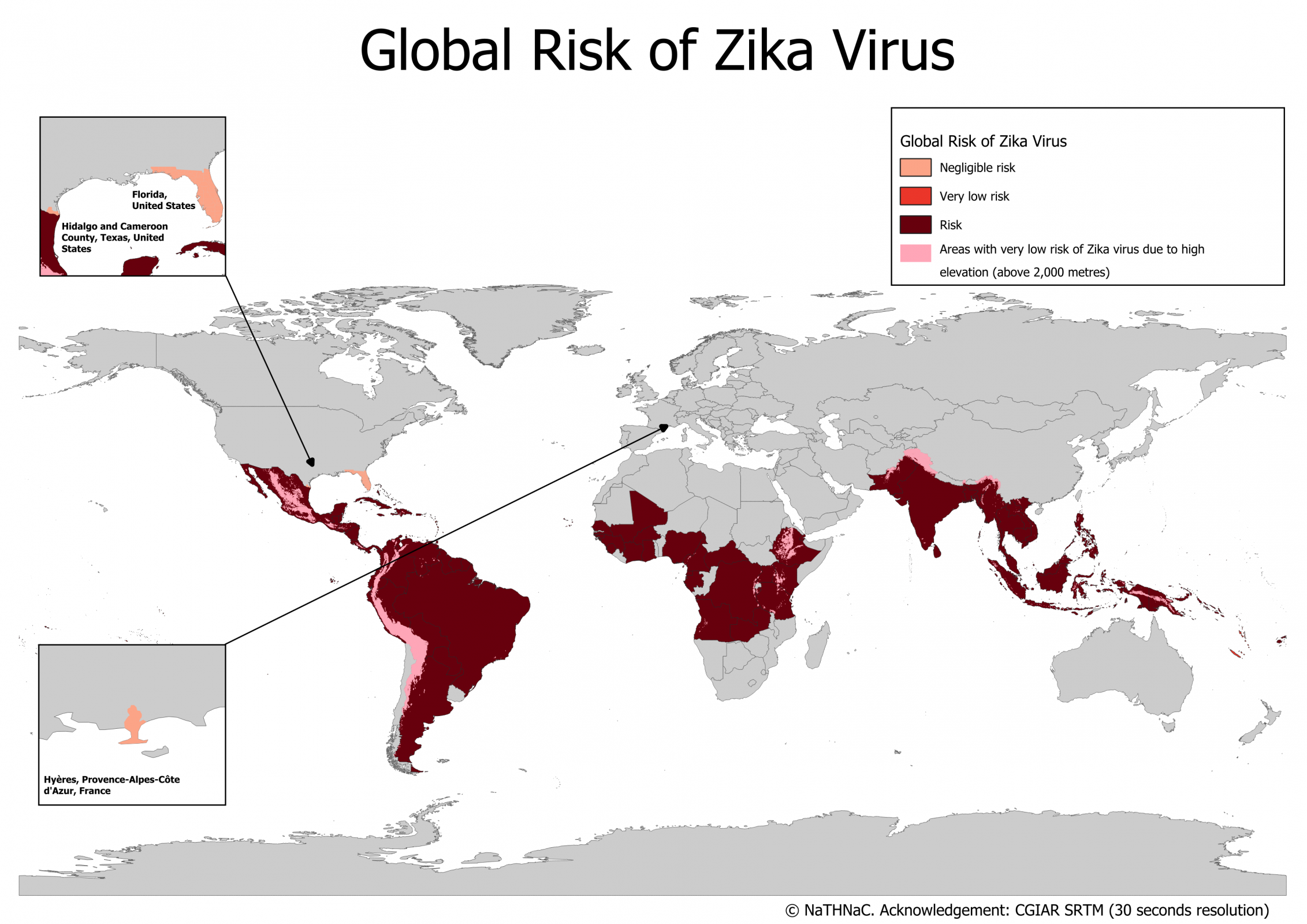
The Zika virus, once a major global health emergency, continues to circulate in the Americas, with the Pan American Health Organization (PAHO) confirming local transmission in 52 countries and territories since 2015.
While case numbers have fluctuated in recent years, the Federative Republic of Brazil remains the epicenter, historically reporting the highest number of confirmed cases in the Americas region.
Recent data highlight Brazil's ongoing battle with the mosquito-borne illness.
Brazil recorded 1,801 confirmed Zika cases, maintaining its lead in the Americas.
As of January 2, 2025, PAHO data indicate that Brazil has significantly reduced its number of confirmed Zika cases, with 2,067 cases reported in 2024 and 3,997 in 2023.
Many Zika outbreaks are concentrated in major Brazilian cities, including Rio de Janeiro, a metropolis of millions and a top destination for international travelers. As the city gears up for Carnaval 2026, scheduled from February 13 to 21, concerns about mosquito-borne diseases linger.
PAHO emphasizes that most Zika infections are mild or asymptomatic, but the virus poses serious risks to pregnant women, potentially causing congenital Zika syndrome in newborns. Travelers, especially those planning pregnancies, are advised to take precautions.
With no locally acquired Zika cases in the continental U.S. since 2019, the U.S. Centers for Disease Control and Prevention (CDC) Yellow Book states that international travelers with suspected Zika infection should be tested with real-time polymerase chain reaction or an NS1 antigen test.
This CDC advice is being followed in Hawai'i.
The Hawaiʻi Department of Health announced on May 27, 2025, that it is investigating two travel-related Zika cases.
And in U.S. territories, the CDC says Zika-spreading mosquitoes are found throughout Puerto Rico, where the Department of Health reported 16 cases in 2024, down from 43 in 2023.
From a disease prevention perspective, the CDC says no Zika vaccine candidate has been approved.
However, clinical trials are active in 2026.
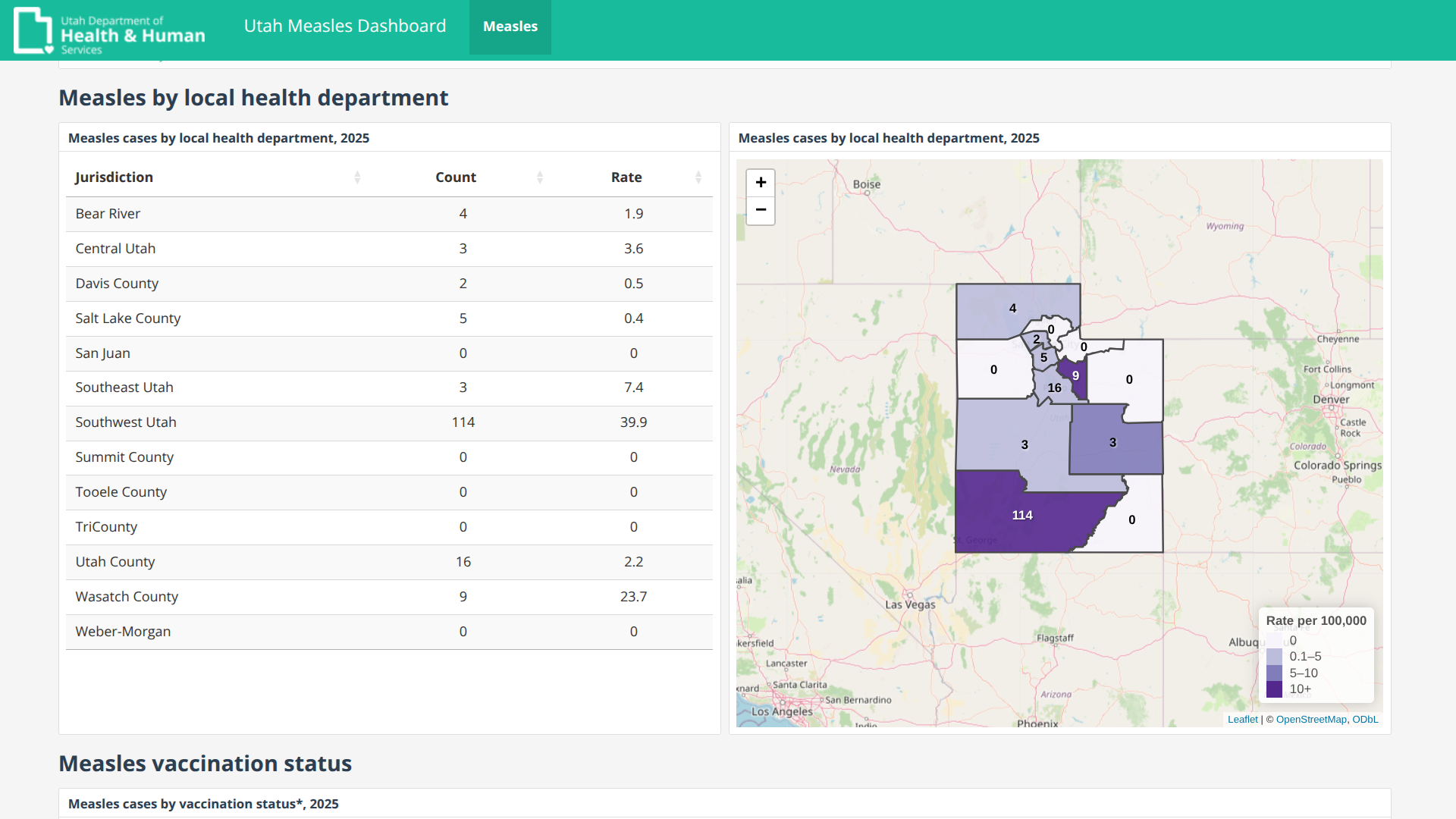
Since mid-November 2025, the Salt Lake County Health Department (SLCoHD) has confirmed measles infections in Utah.
Then, on December 8, 2025, SLCoHD officials and the school district notified everyone in the Bingham High School community of possible measles virus exposures. This followed a confirmed case linked to the Bingham Kopper Kids childcare facility, which is located inside the school in South Jordan.
And on January 1, 2025, Utah's Beaver, Garfield, Iron, Kane, and Washington counties reported their total measles cases reaching 114. These reports contributed to Utah's statewide total, which climbed to 156 confirmed cases at the end of 2025.
Utah's measles outbreak is similar to the current situation in central South Carolina, in that most infected people were unvaccinated.
As of the end of 2025, South Carolina reported 179 cases of measles, centered around Spartanburg County.
'We have seen measles spread quickly in unvaccinated households here in South Carolina. We also know that it can spread rapidly in unvaccinated communities based on outbreaks in other states,' wrote the health department.
As of January 2, 2026, these state health departments and the U.S. CDC recommend MMR vaccination for most people in the USA.
Japan has experienced a dramatic resurgence of syphilis since 2010, reaching epidemic rates again in 2025.
The Japan National Institute of Infectious Diseases (NIID) has reported a significant increase in syphilis cases over the past decade, with the last four years averaging over 13,000 cases annually.
In 2025, the NIID confirmed that this unfortunate trend continued for the fourth consecutive year.
Among Japan's prefectures, Tokyo accounted for 25% of the national total of syphilis cases, followed by Osaka, Aichi, Fukuoka, and Kanagawa.
According to a December 2025 analysis, syphilis risk factors among predominantly heterosexual populations in urban Japan have significantly increased. These findings reveal that casual sexual partnerships and diverse sexual networks facilitated by dating applications and commercial sex services create unique transmission dynamics not adequately captured by previous research.
These researchers stated that promoting preventive measures among sex industry workers and patrons is crucial in Japan's cities.
Syphilis is a sexually transmitted infection (STI) that is generally transmitted by contact with infectious sores, through blood transfusions, or through mother-to-child transmission during pregnancy. This bacterial infection is caused by Treponema pallidum.
Syphilis can be treated with antibiotics such as penicillin. Furthermore, patients can become reinfected, so early antibiotic treatment is necessary.
After decades of clinical trial missteps, a December 18, 2025, study found syphilis vaccine development is beginning to gain momentum due to advances in understanding the outer membrane protein of Treponema pallidum, host–pathogen interactions, and the genomics of syphilis.
Preventing vertical transmission of Treponema pallidum subsp pallidum could be the most consequential target for a vaccine, given the global resurgence of congenital syphilis and adverse pregnancy outcomes.
As of late 2025, the U.S. Preventive Services Task Force and the American College of Obstetrics and Gynecology recommend that pregnant women be tested for syphilis. And in 2026, Alabama, Arizona, Colorado, Georgia, Maryland, Mississippi, Missouri, North Carolina, Tennessee, and Texas require syphilis testing during pregnancy.

The Pan American Health Organization (PAHO) recently reported a concerning increase in cases of hantavirus pulmonary syndrome (HPS) in the Americas, with eight countries confirming a total of 229 confirmed cases and 59 fatalities, a regional case fatality rate of 25.7%.
During 2025, the affected countries include Argentina, Brazil, Bolivia, Chile, Panama, Paraguay, the United States, and Uruguay.
Compared to historical averages, Bolivia and Paraguay have seen sharp rises in incidence.
Paraguay's increase is linked to an outbreak involving occupational exposure.
Meanwhile, Argentina continues to report the highest number of cases in the region.
HPS was first recognized in 1993 and has since been identified throughout the United States.
As of late 2025, the U.S. CDC hasn't released comprehensive totals, but the Southwestern states remain a hotspot.
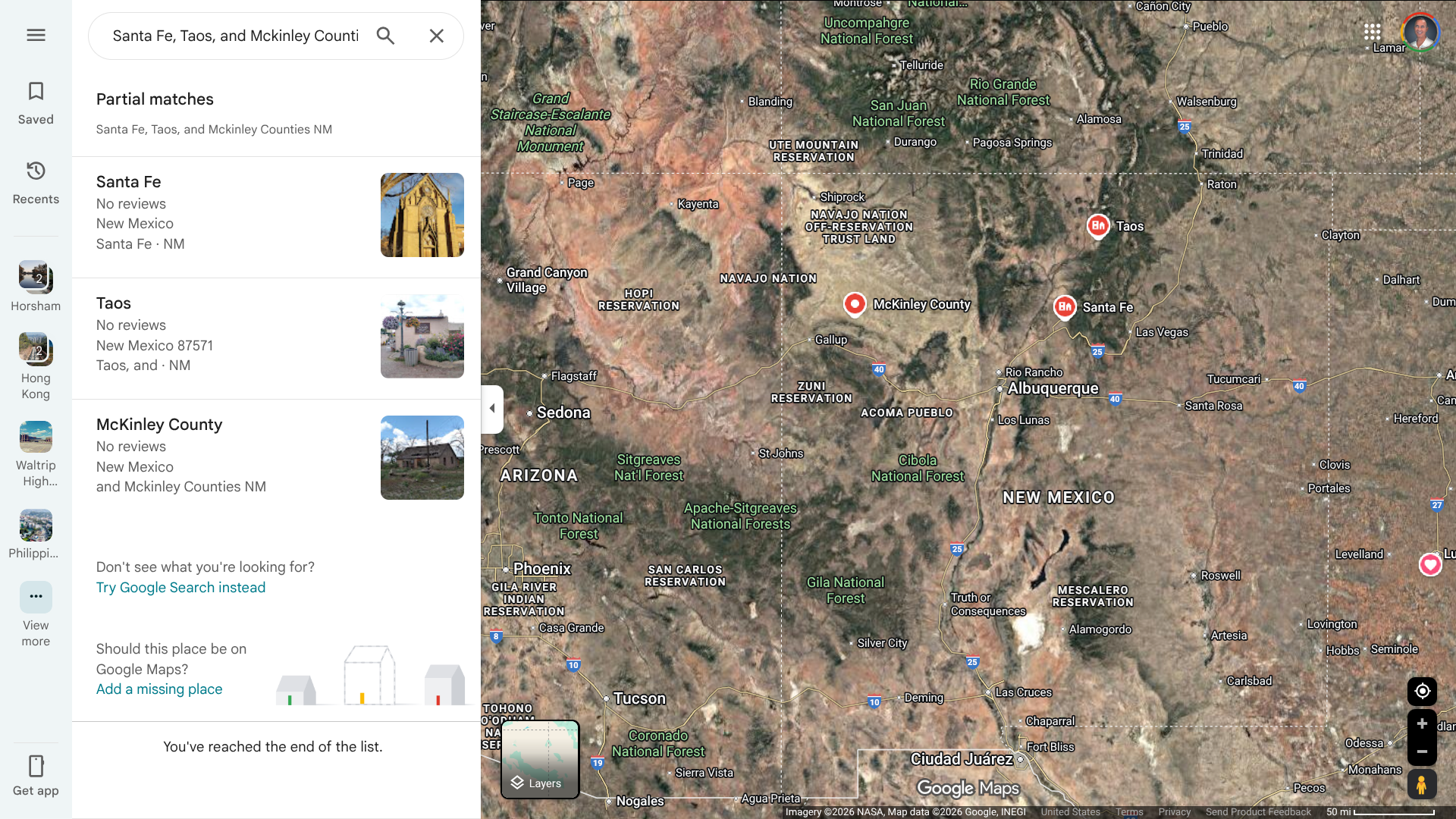
Reports show sporadic HPS cases, notably 7 in New Mexico (Santa Fe, Taos, McKinley, and Bernalillo counties) and a few in other states, including Arizona, Colorado, Nevada, Washington, and Wisconsin.
HPS is primarily a zoonotic respiratory disease transmitted through contact with infected rodents or their excreta. Furthermore, humans can contract the disease when they breathe in aerosolized virus. Rare person-to-person transmission has been documented in the Southern Cone, associated with the Andes virus strain, says the PAHO.
Rodent control in and around the home remains the primary strategy for preventing Hantavirus infection.
As of January 2, 2026, no vaccine is currently available.
With the global spreading of the Chikungunya virus expected to continue in 2026, Valneva SE and Serum Institute of India today announced that they have mutually agreed to discontinue their license agreement for Valneva's IXCHIQ® single-shot chikungunya vaccine.
As of December 31, 2025, Valneva's strategic intent in regaining full rights is to assume direct control over its supply chain and commercialization for endemic high-risk countries, thereby accelerating access for regions most affected by the disease.
According to the European Medicines Agency, IXCHIQ was shown to be effective at triggering the production of antibodies against the chikungunya virus in two primary studies. This is expected to reduce the risk of getting this mosquito-transmitted disease caused by the Chikungunya virus.
Supporting access to the vaccine in low-and middle-income countries falls within the framework of the funding agreement Valneva signed with the Coalition for Epidemic Preparedness Innovations in July 2024, with co-funding from the European Union.
Currently, the U.S. CDC has issued various Travel Health Notices for Chikungunya outbreaks, including a Level 2 alert for China in mid-December 2025.
The CDC advises international travelers to speak with a travel vaccine consultant regarding immunization options before visiting outbreak areas in 2026.

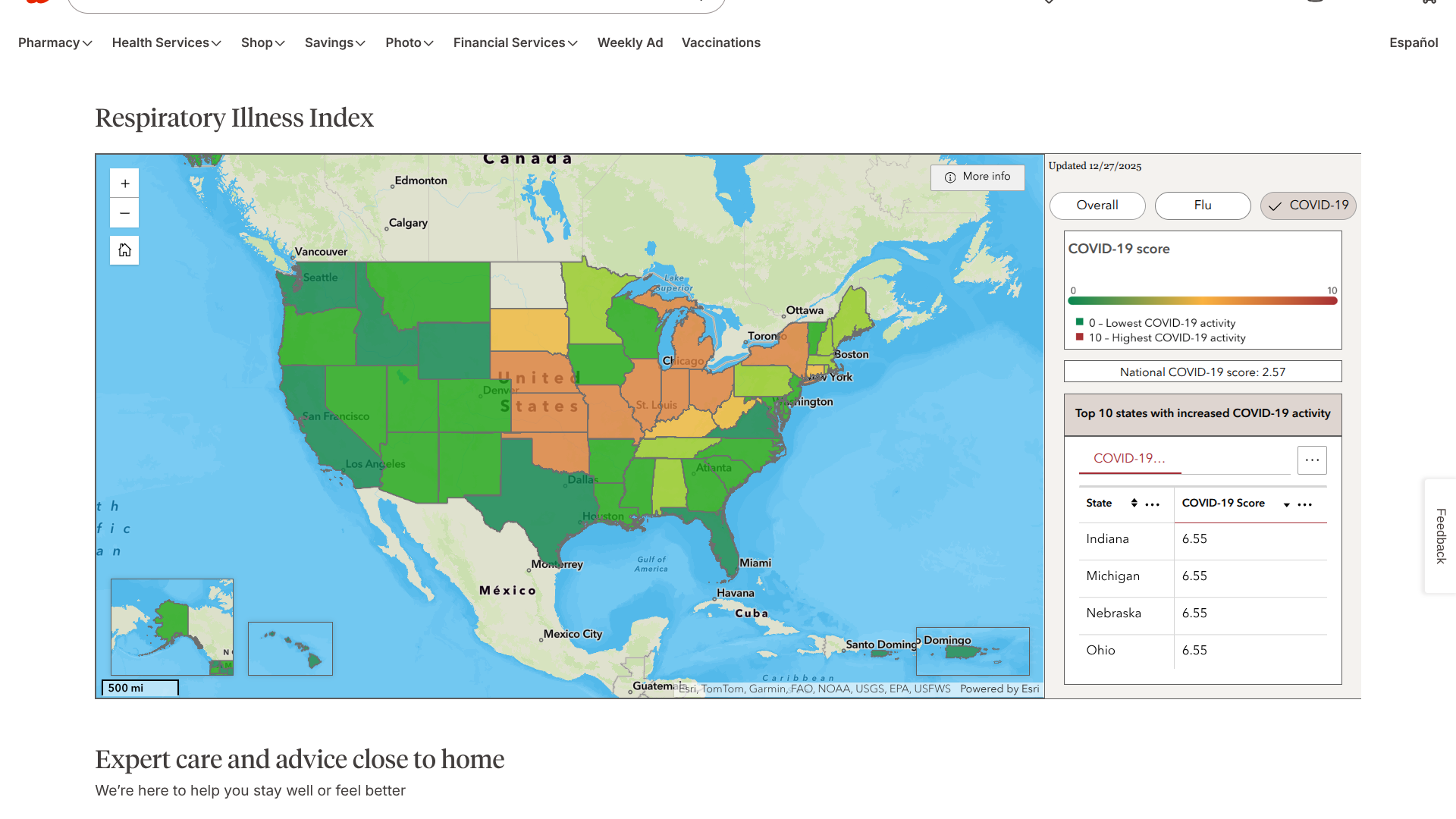
With a winter storm bringing chilly weather to the central states, keeping more people inside, the Walgreens Respiratory Index has also identified an unhealthy trend as 2025 draws to a close.
As of December 31, 2025, the leading states reporting COVID-19-related medications and vaccinations utilization at Walgreens pharmacies include Indiana, Michigan, Nebraska, and Ohio.
Recently, the U.S. CDC reported that COVID-19 vaccination is an effective option for protecting children in these Heartland states and throughout the USA.
In early December, the CDC confirmed that the 2024–2025 COVID-19 vaccination offered additional protection against COVID-19 for children in a population where some individuals had preexisting immunity from previous vaccinations, prior infections, or both, compared to those who were not vaccinated.
The CDC's MMWR also noted on December 11, 2025, that the impact of transitioning from universal vaccination to shared clinical decision-making (individual-based decision-making) on COVID-19 vaccination coverage or effectiveness in children is not well understood. This highlights the need for ongoing monitoring of the effectiveness of COVID-19 vaccines.