Search API
In a significant step toward enhancing global epidemic preparedness, the Serum Institute of India (SII), today announced it has partnered with the University of Oxford under the support of the Coalition for Epidemic Preparedness Innovations (CEPI) to establish an investigational reserve of the ChAdOx1 RVF vaccine candidate against Rift Valley fever (RVF).
This is an essential initiative as no RVF vaccine is currently available.
Confirmed on January 13, 2026, SII will produce up to 100,000 doses of the investigational ChAdOx1 RVF vaccine. An initial 10,000 doses are earmarked for a potential upcoming clinical trial to evaluate the candidate's safety and immunogenicity in outbreak-affected regions. The remaining doses will be maintained as a strategic investigational reserve, ready for rapid deployment in future outbreaks to generate critical clinical data and accelerate evidence for licensure.
ChAdOx1 RVF has completed Phase I trials. Results published from the UK and Uganda trials show it was safe and generated an immune response. A CEPI-supported Phase II trial, separate from the upcoming planned trial, began in Kenya in 2025.
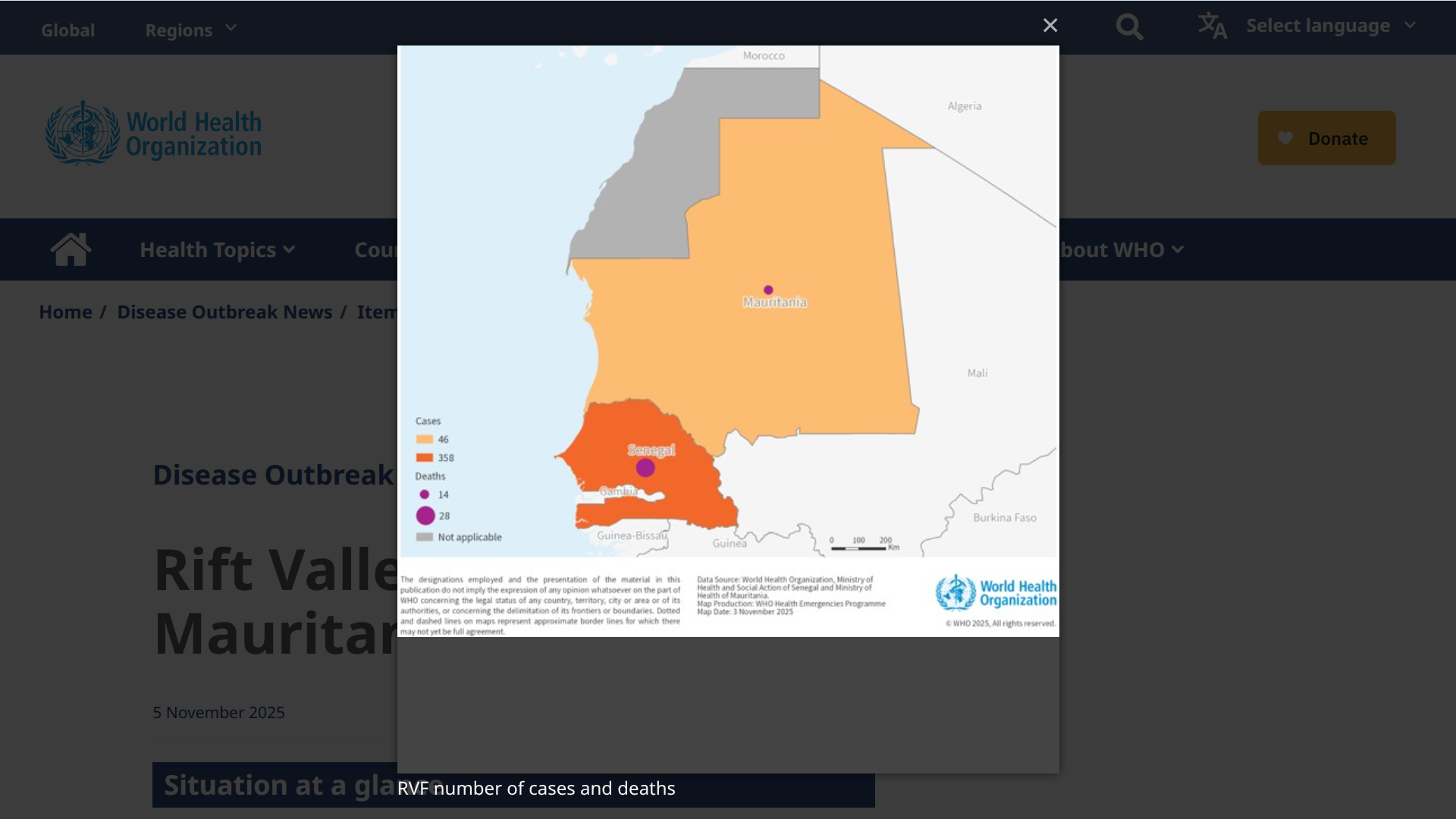
This collaboration arrives as a deadly RVF outbreak continues to impact communities in West Africa, particularly in Sénégal and Mauritania.
According to the latest available World Health Organization (WHO) data, DON584 from 2025, over 600 confirmed human cases, including 47 related deaths, have been reported.
Under the licensing agreement, CEPI is providing up to $3.5 million to support the development, manufacturing, and creation of a reserve for this RVF vaccine candidate.
In a press release, Dr. Umesh Shaligram, Executive Director at SII, added, "Producing these doses at speed is a necessary step to ensure that vaccine candidates like ChAdOx1 RVF can be delivered when and where they're most needed."
Rift Valley fever is a mosquito-borne zoonotic disease that primarily affects livestock but can spill over to humans through contact with infected animals or bites from infected mosquitoes. While most human cases are mild, severe infections can lead to brain inflammation, hemorrhagic fever, and death.
The disease also devastates pastoral communities by causing massive livestock losses, impacting livelihoods and food security in affected regions across Africa and the Middle East.
This collaboration exemplifies proactive "100 Days Mission" principles, positioning the world to respond more effectively to emerging infectious threats like RVF.
Until a vaccine becomes available, the U.S. CDC, WHO, and others recommend that travelers to affected areas follow guidance on mosquito prevention and avoiding contact with potentially infected animals.
The Texas Department of State Health Services (DSHS) today announced it is enhancing wildlife rabies prevention efforts in far West Texas.
Announced on January 13, 2026, the 32nd annual Oral Rabies Vaccination Program (ORVP) aims to protect both people and animals by vaccinating wildlife along the Texas-Mexico border.
Funded by the State of Texas and others, the ORVP has successfully reduced rabies cases significantly since it began over 30 years ago.
Last year, DSHS reported 19 confirmed positive rabies cases in animals from January to June 2025.
Additionally, the ORVP is now expanding to address the Arizona fox rabies variant from New Mexico, located 150 miles away.
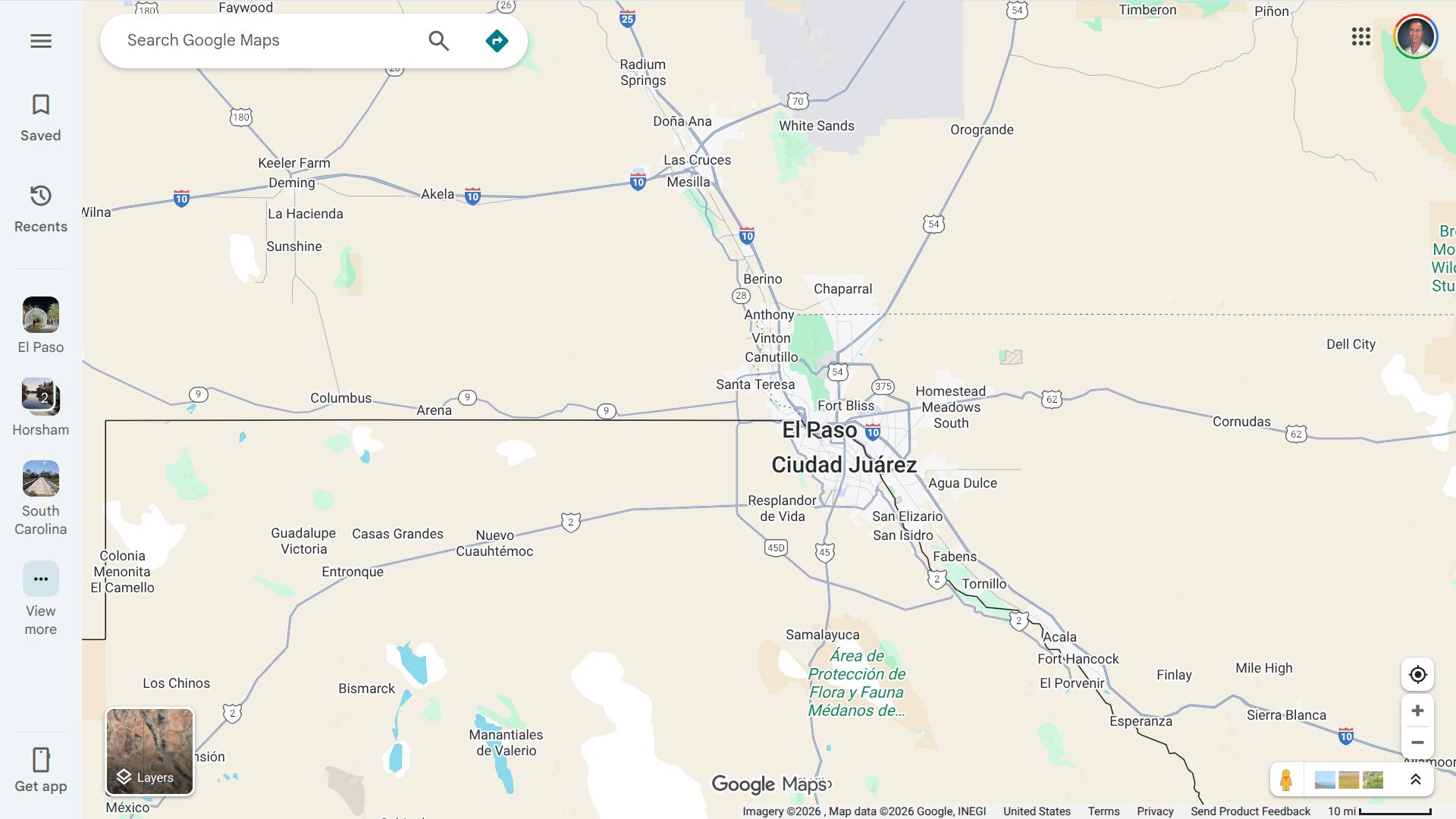
Aerial bait distribution, a key component of the program, will begin from Alpine on January 16, 2026, and from Del Rio International Airport on January 21, weather permitting.
These efforts will occur in the Border Maintenance Zone, covering 19 counties, including El Paso, Hudspeth, and Cameron, as well as targeted urban areas around El Paso.
The vaccine baits, small plastic packets dipped in fish oil and fishmeal, are designed to attract wildlife like coyotes and foxes but pose no threat to pets or livestock.
The two-week operation will involve six to nine flights per day, dropping about 693,600 baits at a density of 50 baits per square mile. Residents should leave found baits undisturbed and can report any concerns to DSHS at 1-877-722-6725 or 512-776-7676.
DSHS continues to monitor all Texas counties for rabies outbreaks, such as red foxes near Austin, Texas.
For more information, visit the DSHS Oral Rabies Vaccination Program page.
Furthermore, rabies vaccines are available from various clinics throughout the United States.
The South Carolina Department of Public Health (DPH) recently reconfirmed that an ongoing measles outbreak in the Upstate region during 2025 has extended into 2026.
On January 9, 2026, DPH reported 310 cases of measles in the current outbreak. Most of these measles cases were concentrated in Spartanburg County. Currently, about 256 infected people in SC were unvaccinated before infection.
DPH wrote Some cases are travel-related exposures or close contacts of known cases. Other cases have no identified source, suggesting that measles is circulating in the community and could spread further.
DPH has identified new public exposures at Jesse S. Bobo Elementary and began notifying potentially exposed students, faculty, and staff on December 30, 2025. Students from Jesse S. Bobo Elementary, Sugar Ridge Elementary, and Boiling Springs Elementary who quarantine successfully without becoming ill are scheduled to return to classes on January 10, 2026.
Separately, North Carolina has reported measles cases in early 2026 linked to travel/exposure in South Carolina, including three in Buncombe County, which is located north of Spartanburg County, SC.
As of January 12, 2026, measles vaccines are available at many primary care provider offices and pharmacies, as well as DPH Health Departments and the Buncombe County Immunizations Clinic at 40 Coxe Avenue, Asheville, NC.
Both county health departments say vaccination remains the best way to prevent measles and stop these outbreaks
As we enter 2026, cholera outbreaks continue to be a significant global threat, despite decades of progress in controlling this severe disease.
The World Health Organization (WHO) has recorded seven cholera pandemics in the last two centuries, with the current seventh pandemic beginning in South Asia in 1961 and still ongoing.
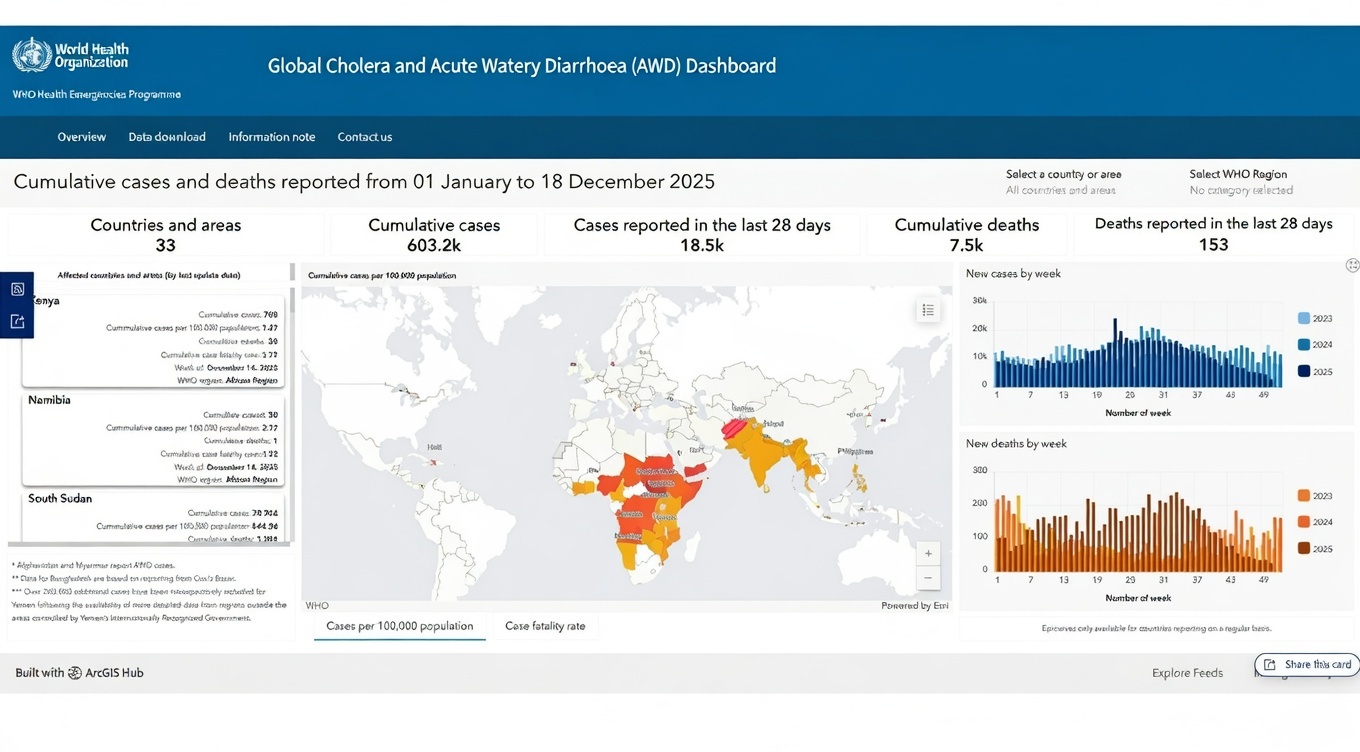
As of December 31, 2025, the WHO has reported a total of 601,845 cholera cases and 7,671 deaths across 31 countries in Africa, Asia, the Middle East, and the Americas.
These numbers indicate persistent transmission across various WHO regions, particularly in the Eastern Mediterranean and African regions, which bear the most significant burden.
Preliminary data for 2025 suggest that case numbers and mortality rates are higher than in previous years. In lower-risk areas, such as the EU/EEA, cholera is uncommon and typically linked to travel from endemic regions.
According to the European Centre for Disease Prevention and Control (ECDC) on January 9, 2026, only 12 confirmed cases were reported across five EU/EEA countries in 2023.
This is a slight increase from 29 cases in 2022, two cases in 2021, and none in 2020.
All recent cases involved individuals with a travel history to affected areas. The WHO highlights vaccination as a crucial strategy in controlling cholera, especially for high-risk groups.
Oral cholera vaccines (OCVs), including WHO-prequalified options like Dukoral®, Euvichol-Plus®, and Euvichol-S®, are recommended for travelers at higher risk of exposure. Travelers planning to visit regions with active cholera transmission should consult travel health clinics to evaluate their personal risk factors and determine if an OCV immunization is appropriate in 2026.
When departing from the USA, OCVs are available at travel clinics in most states.
However, the WHO noted that increased OCV production has yet to meet growing global needs.
As of early 2026, cases of tick-transmitted Lyme disease continue to be reported in various European countries.
Recently, health authorities in the Free State of Saxony, Germany, noted a significant increase in Lyme disease cases in 2025.
According to the Saxon State Office for Health and Veterinary Affairs, a total of 2,623 infections were reported as of December 29, 2025.
This data marks a 61% increase from the 1,626 cases recorded in 2024, and continues an upward trend from 1,484 cases in 2023.
The data rise aligns with reports of elevated tick-borne infections across multiple German federal states.
During 2016−2020, nine federal states in Germany reported 63,940 LB cases, averaging 12,789 cases annually.
Fortunately, cases of tick-borne encephalitis, another serious tick-transmitted viral illness, decreased in Saxony in 2025 to 47 cases from 63 in 2024.
Currently, there is no approved vaccine for Lyme disease in humans in Europe and the United States.
However, promising developments are underway as Pfizer Inc. and Valneva SE are advancing their candidate VLA15, a multivalent protein subunit vaccine targeting the outer surface protein A of Borrelia bacteria.
VLA15 aims to block transmission from ticks to humans and covers prevalent serotypes in the USA and Europe.
Initially diagnosed in Lyme, Connecticut, ticks have spread this severe disease throughout the northeast sections of the USA.
As of January 12, 2026, these companies say 'regulatory filings are planned for 2026, subject to positive final clinical trial results.'
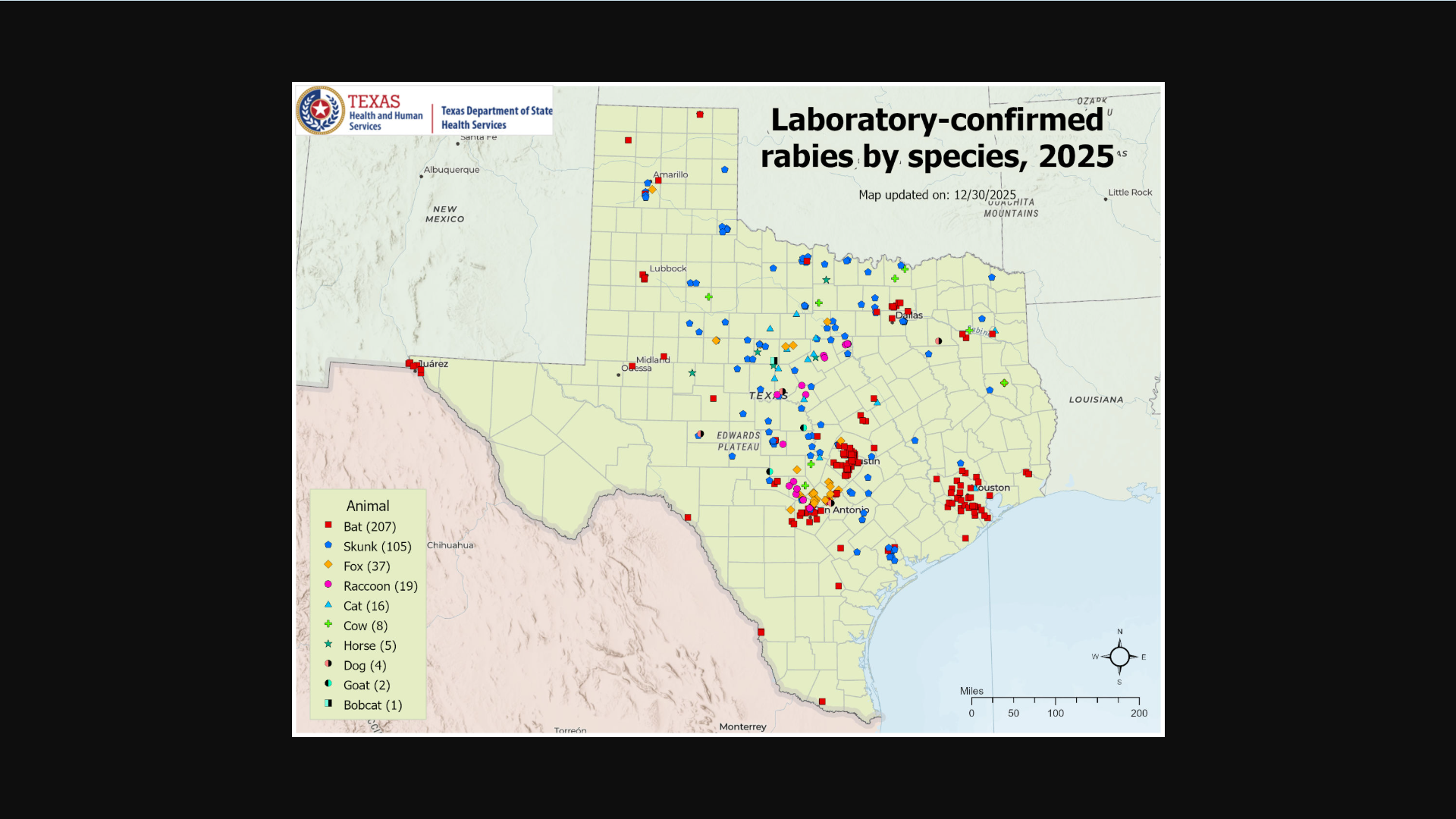
The Texas Department of State Health Services (DSHS) recently confirmed that an outbreak of rabies in wildlife across Hays County and the Austin metropolitan area, primarily affecting red foxes.
Hays County Judge Ruben Becerra issued a public health notice on Facebook on January 10, 2026, to alert residents about the situation. While officials have emphasized that there is no imminent threat to human life, rabies remains a serious and potentially fatal disease that can spread to pets, livestock, and humans through exposure, such as bites or scratches from infected animals.
Texas residents are advised to avoid approaching or handling any wildlife, especially if the animals appear disoriented, aggressive, or unusually tame. Hays County officials are working closely with local healthcare providers, veterinary services, and animal control agencies to monitor the outbreak and ensure readiness.
The Health Department says to protect themselves, their families, and their animals, officials recommend getting pets and livestock vaccinated against rabies as soon as possible. Texas law requires dogs and cats to be vaccinated.
Free rabies vaccination clinics are available in the county for animals, including one on January 17, 2025, at the PALS Clinic in San Marcos, TX.
While foxes are common carriers of the virus in central Texas, most rabies cases in the United States are related to bat bites. Travis County, which includes the Austin metro area, had the highest number of reported rabies cases with 68 cases (63 of which were bats) in 2024.
In 2025, DSHS and the U.S. Department of Agriculture conducted air-dropping of oral rabies vaccines in several states to help reduce wildlife outbreaks.
For humans, DSHS confirms rabies is a vaccine-preventable viral disease. Two types of vaccines protect people against rabies: nerve tissue and cell culture vaccines.
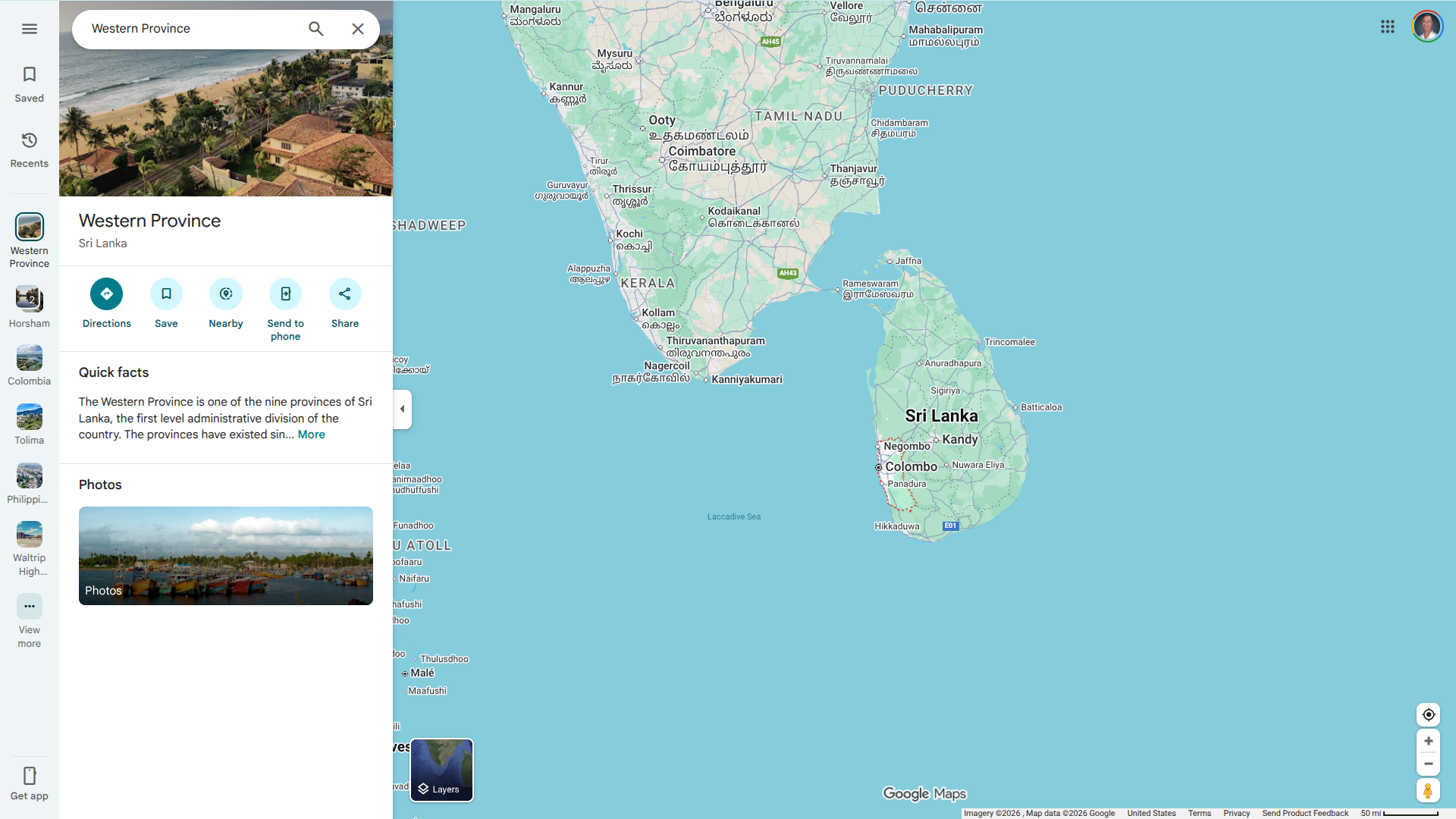
Health officials in Sri Lanka have reported a surprising surge in dengue fever cases early in the year, with 2,170 confirmed infections recorded during the first nine days of January 2026.
According to a report by Xinhua on January 10, 2026, Prashila Samaraweera, a Community Medical Specialist at the National Dengue Control Unit, indicated that there is a "high-risk dengue situation" across 41 Medical Officer of Health divisions.
The Sri Lankan Western Province has the highest number of cases, including the cities of Colombo, Gampaha, Kandy, Galle, Ratnapura, and Jaffna.
This early spike follows a challenging year in 2025, during which Sri Lanka reported around 50,000 dengue cases.
The World Health Organization (WHO) states that dengue is endemic year-round in Sri Lanka, which is located off India's southeast coast. Seasonal disease peaks are often associated with monsoon rains, as virus-carrying mosquitoes thrive in stagnant water.
Currently, there is no widely available dengue vaccine recommended for all travelers to Sri Lanka. Currently, three dengue vaccines are approved for use.
However, travelers and residents are advised to take preventive measures, such as eliminating standing water around homes and communities.
The WHO recommends that travelers planning to visit Sri Lanka prioritize mosquito protection measures to ensure their health from other diseases, such as chikungunya.
If departing from the United States for Sri Lanka, the CDC recommends vaccination for travelers visiting an area with a chikungunya outbreak in 2026. International travelers can obtain personal vaccination advice at local travel clinics in the USA.