Search API
The Taiwan Centers for Disease Control (TCDC) continues to report a significant increase in acute viral hepatitis A (HepA) cases.
The surge that began in spring 2025 has led to the highest number of reported cases in nearly a decade and remains unabated as of January 20, 2026.
Official surveillance data from the Taiwan National Infectious Disease Statistics System show that there were a total of 484 confirmed acute HepA cases for the entire year of 2025.
Demographic data from this period reveal that approximately 82.8% of cases occurred in males, with the highest proportion (36.2%) among adults aged 30-39 years. Additionally, 40% of the cases in 2025 were linked to sexual contact.
In the early weeks of 2026, an additional 22 cases have already been recorded, with individuals aged 20-29 accounting for about 28% of these cases.
Historical outbreaks show HepA cases concentrated in northern Taiwan, spreading southward over time.
The TCDC has emphasized that hepatitis A antibody prevalence in Taiwan remains notably low, particularly among younger and middle-aged adults. This leaves large segments of the population vulnerable and contributes to the continued spread of the virus, which spreads through the fecal-oral route, often via contaminated food or water, or through close contact with infected individuals.
For real-time statistics and official guidance, please refer to the Taiwan National Infectious Disease Statistics System or the CDC website. It is crucial to maintain vigilance regarding hygiene, safe practices, and vaccination to mitigate this ongoing increase in cases.
According to the U.S. CDC, unvaccinated travelers aged 1 year or older traveling to Taiwan should speak with a healthcare provider about pre-trip vaccinations. Travelers allergic to a vaccine component should receive a single dose of immune globulin, which provides adequate protection for up to 2 months, depending on the dosage given.
Unvaccinated travelers who are over 40 years old, are immunocompromised, or have chronic medical conditions planning to depart for a risk area in less than 2 weeks should receive the initial dose of vaccine and, at the same appointment, receive immune globulin, says the U.S. CDC.
These HepA immunization services are offered at travel clinics in the United States in 2026.
Clemson University officials were recently informed by the South Carolina Department of Public Health (DPH) of a confirmed case of measles in an individual affiliated with the University.
As of January 17, 2026, the individual has isolated per DPH requirements, and DPH is conducting contact tracing with individuals who may have been exposed and outlining isolation and quarantine protocols.
DPH will provide email notifications to any individuals identified as possible contacts who may need to quarantine. A person infected with measles is contagious for 4 days before and after the rash begins. Isolation of an actively infectious case lasts until four full days after the onset of the rash, and DPH determines the dates of isolation.
If a person without documented immunity receives a dose of the MMR vaccine within 72 hours after the last exposure, they do not have to quarantine.
According to the most recent data from Student Health Services, nearly 98% of main campus Clemson students have provided proof of immunity. Recent data indicated that about 30,000 students and staff were affiliated with the University in 2026.
Statewide, South Carolina is experiencing a significant measles outbreak, with the total reaching 558 cases as of January 19, 2026, centered in Spartanburg County and extending into North Carolina in cities such as Asheville.

As the 2025-2026 influenza season continues, recent data from the U.S. Centers for Disease Control and Prevention (CDC) indicate a significant decrease in flu activity nationwide.
The CDC's assessment framework classifies the current flu season as moderate across all age groups. Typically, flu seasons in the United States peak between December and February, sometimes extending into March or later.
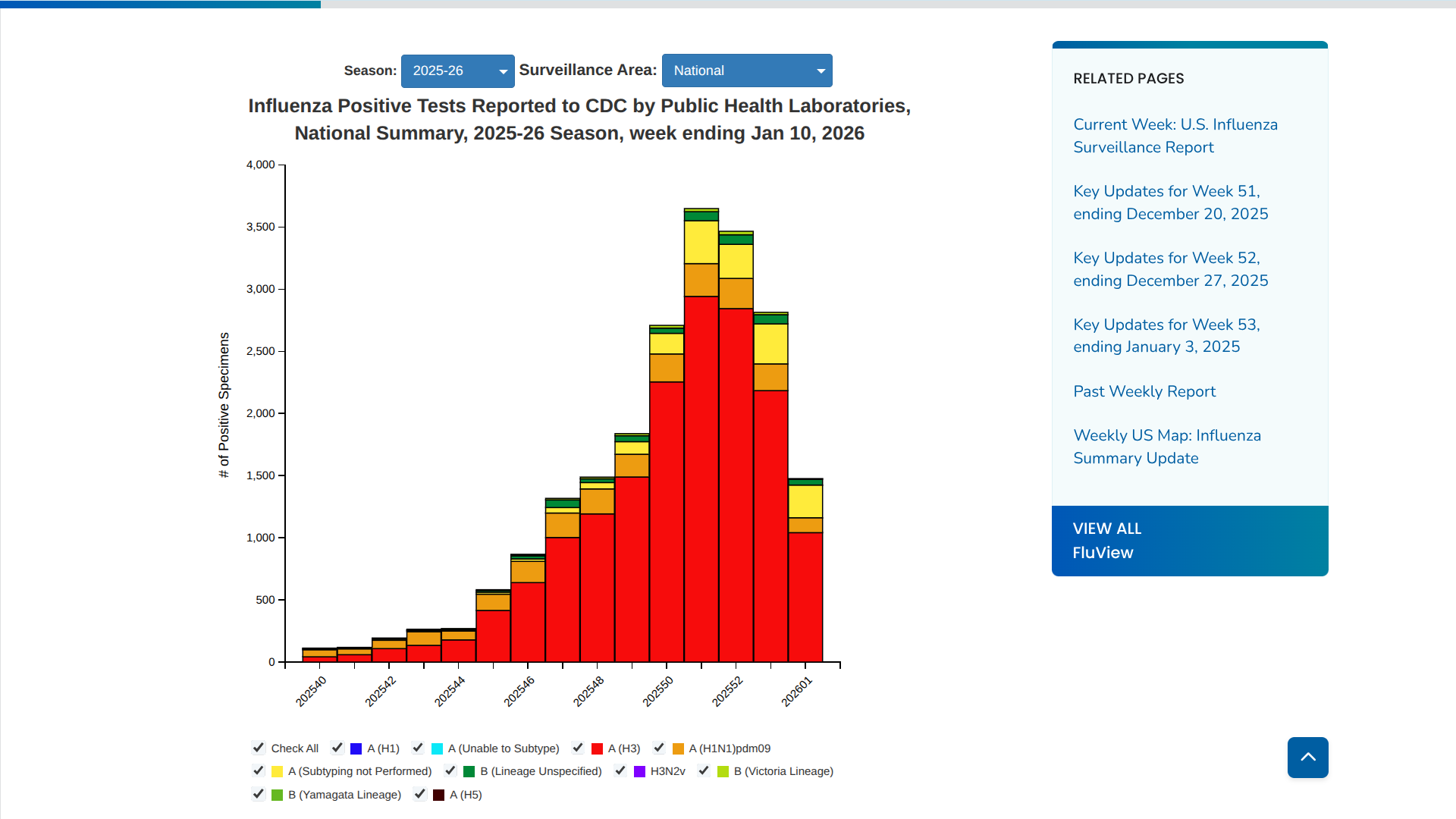
According to the CDC's latest FluView report for the week ending January 10, 2026, the number of confirmed positive influenza tests dropped by approximately 31% compared to the previous week.
This decline marks the most significant drop observed in this season so far.
The flu test positivity rate dropped to approximately 24.7% for the week ending January 3, down from 32.9% the previous week. However, experts caution that this could partially reflect reduced healthcare visits during the holidays rather than an actual peak.
Influenza A(H3N2) viruses are the most frequently reported influenza viruses so far this season.
These data mark a shift from earlier reports, such as the week ending December 27, 2025, when activity was still increasing throughout the USA.
The CDC also reported on January 19, 2026, that about 130 million flu shots had been distributed to clinics and pharmacies this flu season. Furthermore, these healthcare providers continue to recommend and offer flu shot services.
Indian health officials in western Madhya Pradesh recently implemented emergency measures in response to a localized outbreak of Guillain-Barré Syndrome (GBS), a rare autoimmune neurological disorder.
As of January 18, 2026, The Hindu reports indicate that there are at least 14 to 18 cases of GBS (confirmed and suspected), many of which are among children and adolescents.
Two people have died in 2026, and others were on life support, with some cases requiring ICU treatment.
Additional cases have been reported in adults, including a recent diagnosis in Neemuch city.
In response to the outbreak, two rounds of door-to-door screenings have been conducted by Health Department teams, ASHA workers, and Anganwadi staff to identify potential new cases early.
During early January 2026, Deputy Chief Minister Rajendra Shukla, who oversees health, visited the area to inspect preparations and directed that the government cover the treatment costs, including critical medications and injections.
Financial aid is also being provided to some families through the Red Cross Society.
GBS is often triggered by preceding infections, such as Campylobacter jejuni (which can result from contaminated food or water), respiratory viruses, or other pathogens; however, the exact cause of this current cluster is still under investigation.
Past GBS clusters in India have occasionally been linked to water quality issues or acute diarrheal diseases.
In 2025, Pune, Maharashtra, reported over 200 cases and 23 deaths linked to contaminated water sources.
For international travelers to India, including Madhya Pradesh, major health authorities such as the U.S. CDC have not issued specific travel health advisories related to this GBS outbreak. Standard travel vaccinations (hepatitis A, typhoid, and rabies, if at risk) are still recommended for travel to India in 2026.
Currently, there is no vaccine available to prevent Guillain-Barré Syndrome.
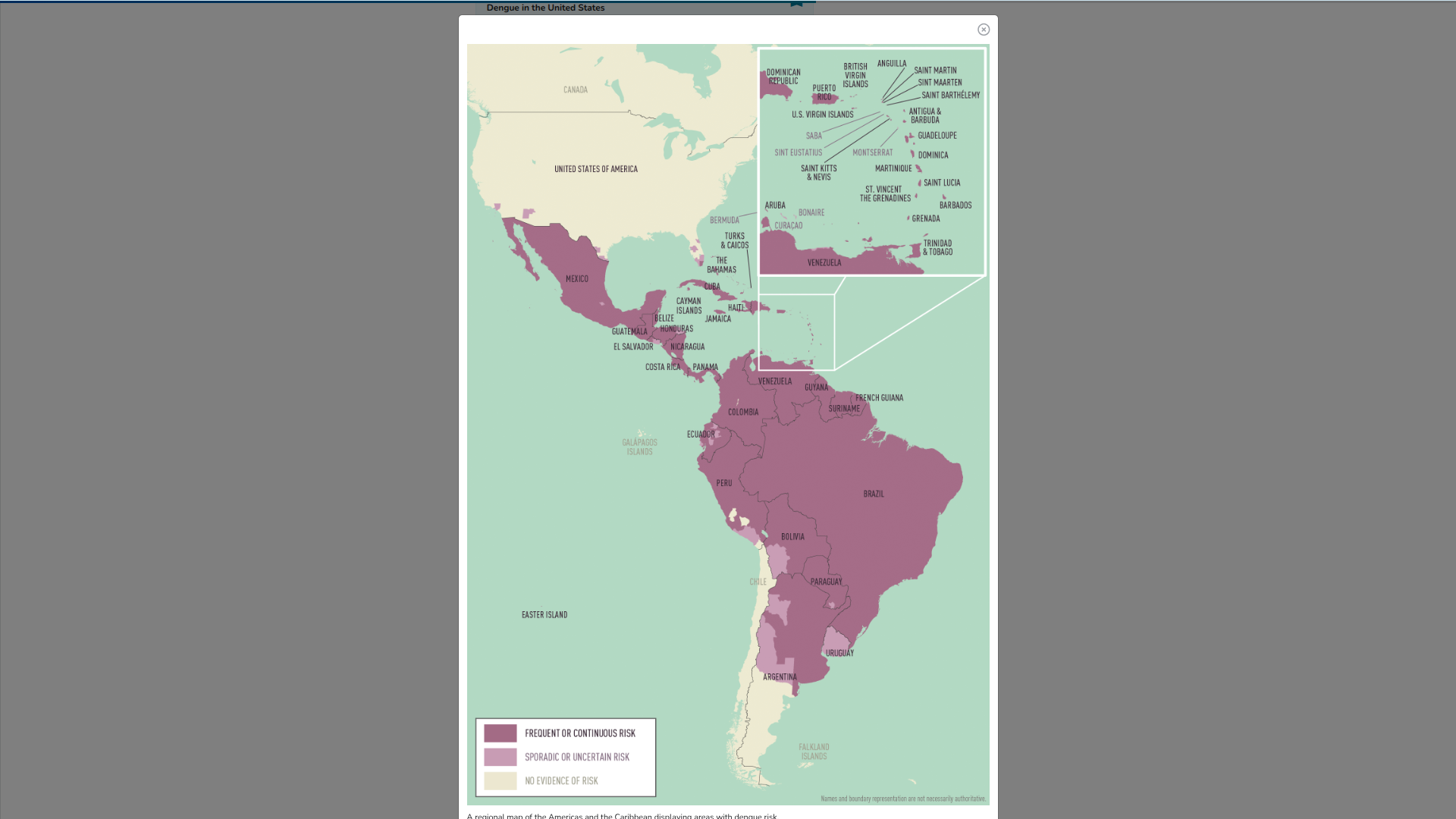
Since 1980, the Pan American Health Organization has been collecting epidemiological data on the incidence of dengue. Following significant dengue fever outbreaks in South America during 2024 and 2025, researchers are investigating the root cause.
For example, Peru has experienced severe national dengue outbreaks.
In 2010 and 2011, the Loreto region of Peru experienced an unprecedented dengue outbreak. In 2025, Peru reported over 270,000 cases and 261 deaths, which set records without a known clinical explanation.
A retrospective study (Volume 19, Issue 1) published by ScienceDirect in January 2026 offers new insights into the circulation patterns of dengue virus (DENV) serotypes in the Amazonas region of northeastern Peru from 2021 to 2025.
The research identifies DENV-2 as the dominant serotype driving major outbreaks in this Amazonian area while also revealing unexpected protective effects from prior infections against severe disease manifestations.
Furthermore, DENV-1 and DENV-3 circulated less frequently during the study period.
No direct association was found between specific serotypes and clinical classification, severity, or overall incidence rates.
Notably, prior dengue infection was significantly associated with a reduced likelihood of developing warning signs of severe dengue (p = 0.032), suggesting partial cross-protection during secondary infections.
"These results emphasize the critical role of DENV-2 in driving major dengue surges in Amazonas, while also highlighting how previous exposure to the virus may offer some protection against more severe symptoms," noted the lead researchers.
"This underscores the importance of sustained molecular surveillance to track DENV serotype shifts and inform targeted public health responses."
The findings from the Amazonas region align with broader trends in the Americas, where infection with one serotype does not confer complete immunity to others, and secondary infections can sometimes lead to severe forms of the disease.
This is essential information, as millions of international travelers visit Peru, many of whom visit Machu Picchu.
Regarding which dengue vaccine offers the broadest protection, only one provides equivalent tetravalent protection against all four dengue virus serotypes (DENV-1, DENV-2, DENV-3, and DENV-4). However, the single-dose Butantan-DV vaccine is only available in Brazil.
According to a 2025 survey, most people in Peru are interested in access to a next-generation dengue vaccine.
Since October 2025, several European countries have observed increases in influenza positivity rates among patients tested in community laboratories, beginning as early as week 41 of 2025.
According to a Rapid Communication published in Eurosurveillance (Volume 31, Issue 2), in France, the 2025/26 flu season is characterized by high circulation of influenza A(H3N2) viruses from subclade K, alongside co-circulation of A(H1N1)pdm09 subclade D.3.1.1.
As of January 15, 2026, an early assessment of influenza vaccine effectiveness (VE) against laboratory-confirmed influenza using data from community laboratory surveillance through the first week of January 2026.
The overall interim VE estimate for individuals vaccinated from 15 days to 3 months before testing was 36.4% (95% CI: 29.7–42.5). Among the population aged ≥ 65 years, the point estimate was lower, peaking at 27.7% and overlapping with the 95% CI (16.7–37.3).
These researchers concluded that despite a partial vaccine mismatch this season, interim analyses indicate a statistically significant vaccine VE across all age groups.
In the context of sustained influenza circulation in Europe, it is strongly recommended to reinforce vaccination uptake in the coming weeks.
This new data supports the U.S. CDC's recommendation that most visitors to France get an annual flu shot about two weeks before traveling abroad in 2026. Various flu shots are offered at travel clinics in the USA.

The Delhi Statistical Handbook 2025, published on January 8, 2026, by the Directorate of Economics & Statistics and the Office of the Chief Registrar of the Government of NCT of Delhi, reveals a concerning increase in respiratory-related fatalities in recent years.
The updated handbook highlights the growing health burden from conditions such as asthma, pneumonia, and chronic obstructive pulmonary disease, which are risks for residents and visitors in 2026.
In 2024, Delhi recorded 9,211 deaths from respiratory diseases, an increase from 8,801 in 2023 and 7,432 in 2022.
Additionally, overall mortality in the capital rose to 139,480 deaths in 2024, up from 132,391 in 2023.
Local health experts attribute the severe air pollution in Delhi to factors including vehicular emissions, industrial activity, construction dust, and seasonal stubble burning.
These advocates call for immediate measures, such as improved public transport, stricter regulations, and enhanced regional cooperation, to prevent further loss of life in or around Delhi.
According to data from India's Ministry of Tourism, Delhi remains a very popular destination. There were about 39 million domestic visitors and around 1.8 million international visitors in 2023.
As of January 16, 2026, the U.S. Centers for Disease Control and Prevention (CDC) has not issued a Travel Health Notice focused on Delhi's air pollution. But the CDC has identified several health risks and vaccination recommendations for travelers to India.
The CDC advises future visitors to India speak with a travel vaccine expert about immunization options.

A new large-scale study analyzing healthcare claims data from 2016 to 2022 has revealed that Lyme disease (LD) imposes a substantial economic burden, with direct medical costs significantly higher for patients with disseminated disease compared to those with localized infections.
This new research, published in JAMA Network Open on January 14, 2026, identified over 70,000 Lyme disease cases and employed multiple analytical approaches to estimate costs, all adjusted to 2022 dollars.
Key findings highlight the mean LD-specific direct medical cost per episode at $2,227.
Furthermore, costs varied dramatically by disease stage:
- Localized, early-stage disease: $695 per episode compared with $695,
- Disseminated disease: $6,833 per episode,
- In a self-control approach, patients incurred an average of $3,304 higher all-cause costs in the 6 months following diagnosis than in the prior 6 months,
- Case-control comparisons showed differences ranging from $4,098 to $5,571 in projected 6-month total all-cause costs after multivariable adjustment for baseline characteristics.
According to these researchers, these estimates were generally higher than those from prior studies, potentially due to longer episode durations allowed in this analysis, the use of standardized insurance-allowed amounts, and inclusion of diverse insurance types and all age groups.
These findings emphasize the need for enhanced prevention strategies, prompt diagnosis, and awareness to mitigate escalating healthcare expenditures. Early intervention could substantially reduce the disproportionate costs driven by disseminated disease, these researchers added.
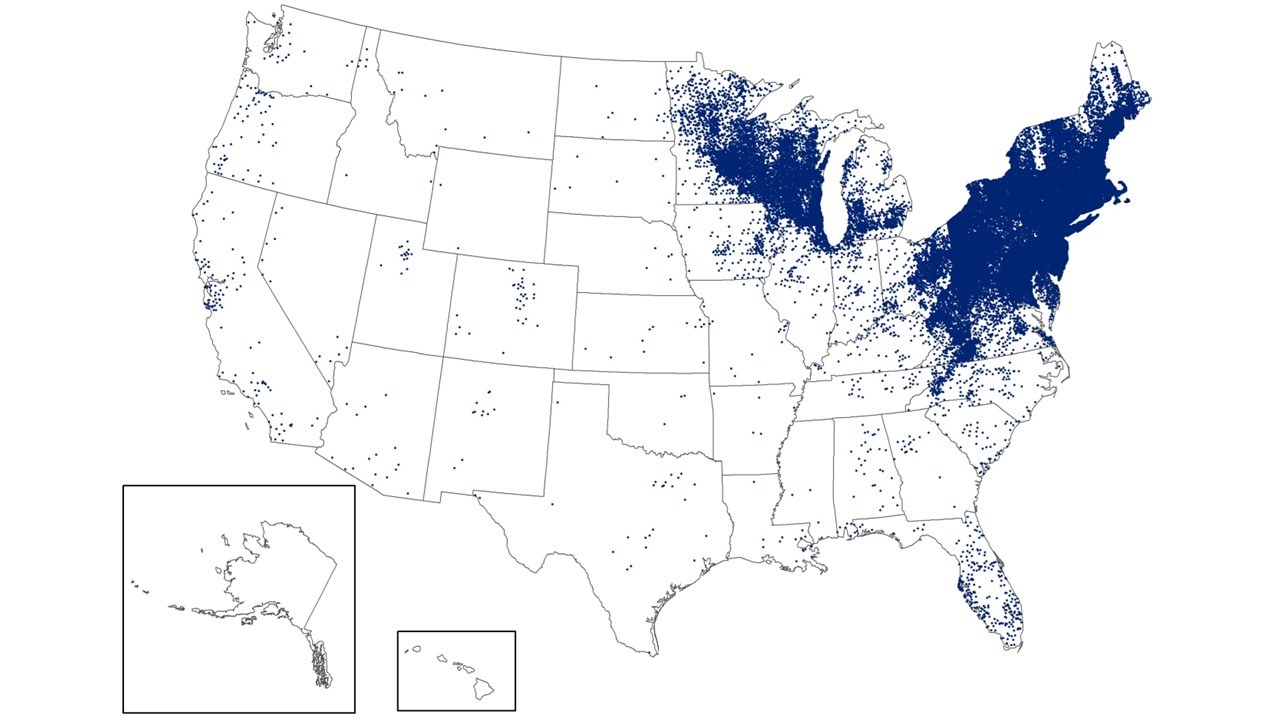
The U.S. CDC says Lyme disease remains the most common vector-borne illness in the United States, with an estimated 476,000 people diagnosed and treated annually. In 2025, most LD cases were reported in the northern states in the east and the Midwest.
From a disease prevention option, one Lyme disease vaccine candidate (VLA15) is progressing in phase 3 clinical trials. However, the approval date for this innovative vaccine has not yet been announced.