Search API
With international travel forecast to increase again in 2026, a group of innovative vaccines is showing positive trends.
Bavarian Nordic A/S today announced its preliminary, unaudited financial results for 2025, highlighting strong demand for its travel vaccines.
On February 12, 2026, the company confirmed that its Travel Health business exceeded its latest financial guidance, reporting a 30% increase compared to 2024.
The demand for its existing rabies and Tick-Borne Encephalitis vaccines continued to grow, with increases of 34% and 20%, respectively.
Additionally, the first-year sales of the chikungunya vaccine (VIMKUNYA®) reached DKK 85 million (approximately $13.4 million).
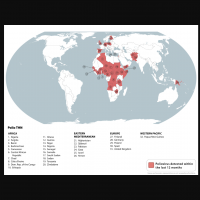
While the mosquito-transmitted chikungunya virus has affected over 100 countries since its emergence, the state of Florida is reporting numerious travel-related cases and even an unusual local case in early 2026.
These increases exceed the global international travel activity, which only increased by 4% from 2024 to 2025, according to data from UN Tourism.
Paul Chaplin, President and CEO of Bavarian Nordic, commented in a press release, "We are encouraged by these extraordinary results."
We remain, however, the leading provider to governments of mpox and smallpox vaccines to support their public health responses, whether during outbreaks or for long-term stockpiling, and we continue to build strong partnerships to expand the base business."
The unedited company press release is found at this link.

Health officials in Florida are monitoring a significant increase in chikungunya fever cases, predominantly linked to travel from Cuba, where the mosquito-transmitted virus was associated with more than 50,000 cases in 2025.
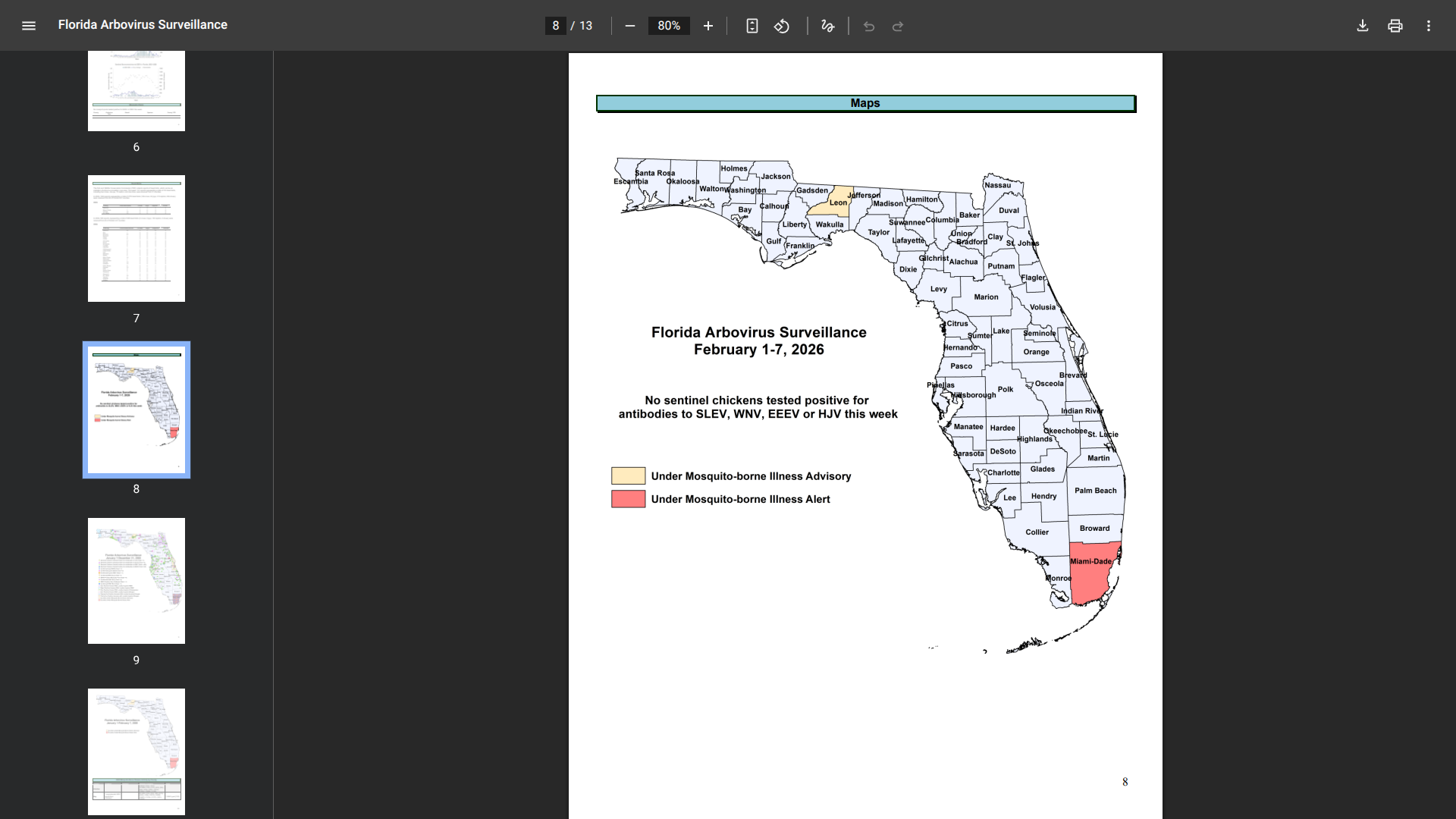
According to week #5 data from the Florida Department of Health (DOH), the state recorded a high number of travel-associated cases this year.
As of early February 2026, health officials have reported 16 cases with onset in 2026 among individuals with a recent travel history from Cuba. The most affected counties include Miami-Dade (10 cases) and Palm Beach (2 cases).
In 2025, Florida reported 370 travel-associated chikungunya cases. Of these, 357 were linked to travel to Cuba.
Furthermore, the DOH reported a rare but notable case of locally acquired chikungunya fever in Miami-Dade County, with symptom onset in December 2025.
This marks the first instance of local transmission in Florida since 2014, when 12 cases were reported.
Local transmission in Florida indicates the virus was passed from an infected traveler to a resident through mosquitoes within the state, raising concerns about the potential establishment of the virus in areas with competent mosquito vectors in 2026.
As of February 12, 2026, the U.S.CDC maintains a Level 2 Travel Health Notice ("Practice Enhanced Precautions") for chikungunya in Cuba, advising travelers to use insect repellent, wear long sleeves and pants, and take other measures to prevent mosquito bites.
Additionally, the CDC advises travelers visiting chikungunya-endemic areas to speak with a vaccine expert about the 2026 immunization option.
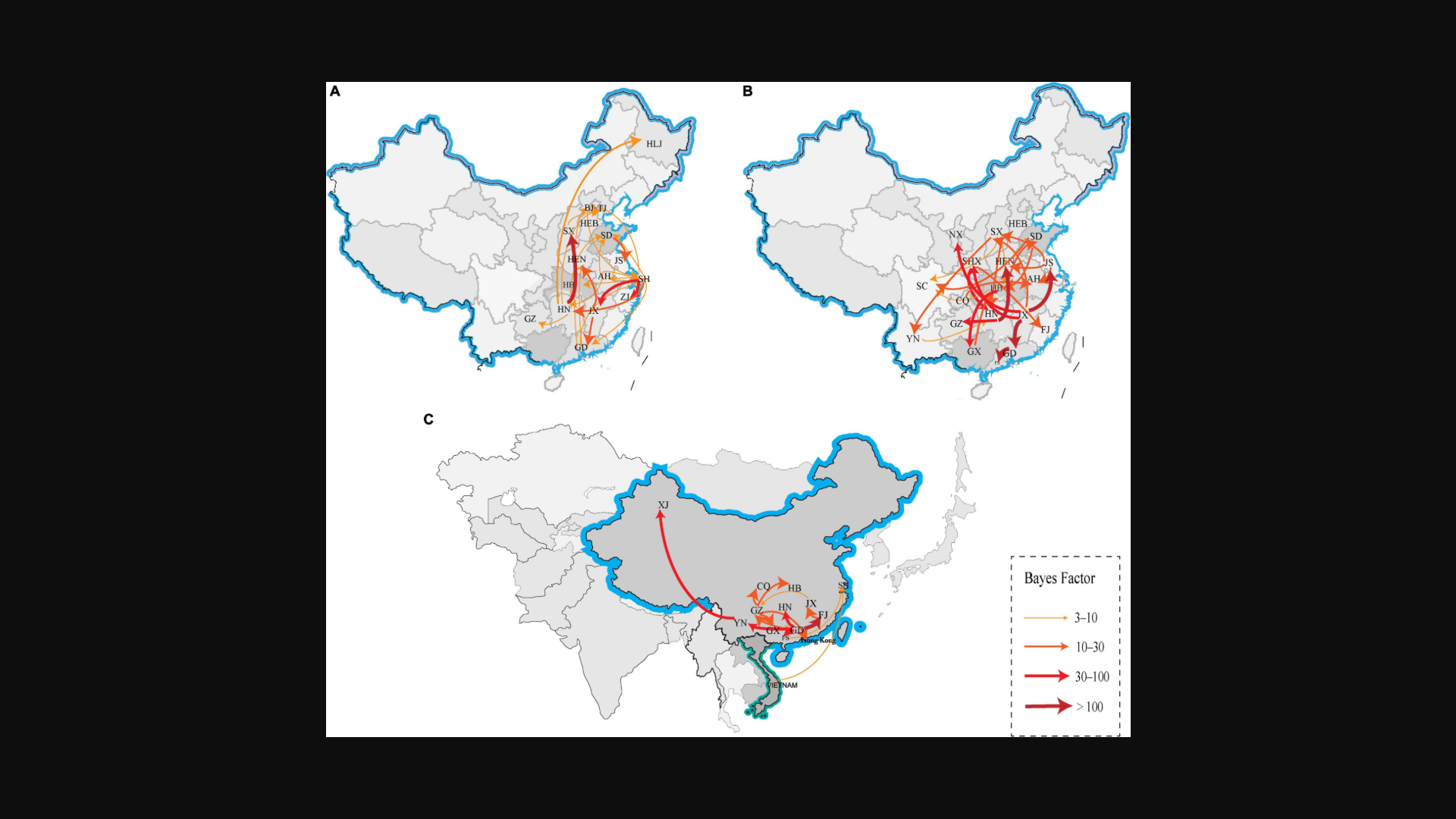
Hong Kong's Centre for Health Protection (CHP) reported two new human cases of H9N2 avian influenza infection from mainland China, with symptom onset in late December 2025 and mid-January 2026.
The announcement, published on February 10, 2026 (Week 6), highlighted ongoing sporadic detections of the low-pathogenic bird flu virus in humans.
These cases in Hubei, Guangxi, and Jiangsu provinces coincided with the reporting of an additional human infection involving avian influenza A(H10N3) in a 34-year-old man from Guangdong Province, whose symptoms also began on December 29, 2025.
If confirmed, this would mark only the seventh known human case of H10N3 globally.
According to CHP data, 20 H9N2 cases have been reported in China over the past six months.
Unlike highly pathogenic strains like H5N1, H9N2 has not shown sustained human-to-human transmission.
In the entire year of 2025, mainland China recorded 29 H9N2 cases, which marks a significant increase compared to previous years (11 cases in 2024).
While global human H9N2 infections remain relatively low, they have risen in recent years, primarily in China, with occasional reports from neighboring regions.
Since the first confirmed human case in 1998 (Hong Kong), officials stress that although H9N2 infections are uncommon in humans, continued surveillance is essential because the virus circulates in poultry and can reassort with other influenza strains.
H9N2 is a low-pathogenic avian influenza virus commonly found in poultry, particularly in live bird markets across parts of Asia. Human infections are generally mild, resembling the seasonal flu, with symptoms such as fever, cough, and sore throat; most patients recover fully without severe complications.
Another virus subtype is notable for causing severe illness in people, despite being classified as low pathogenic in birds. As previously reported, between March 2013 and September 2019, a total of 1,568 human cases of avian influenza A(H7N9) have been reported globally.
As of February 12, 2026, the CHP and the World Health Organization (WHO) (January 2026) say the overall public health risk from these cases is assessed as low. The WHO does not advise special traveller screening at points of entry or restrictions about the current situation of influenza viruses at the human-animal interface
Furthermore, these agencies say vaccination options are currently limited.
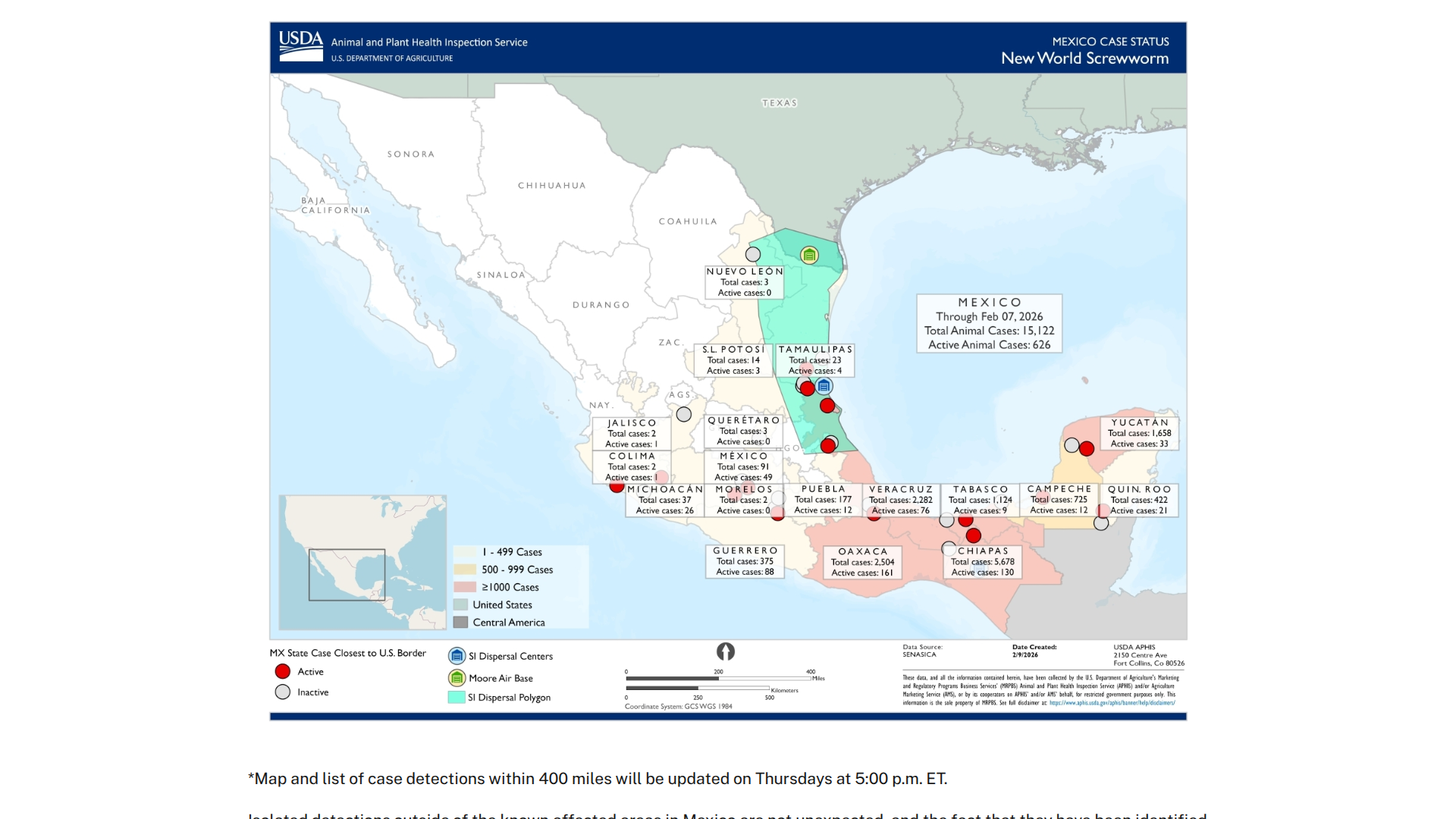
The Mexican Ministry of Health has confirmed six new human cases of myiasis caused by the New World screwworm (NWS, Cochliomyia hominivorax), bringing the total number of reported human cases to 141 across eight states.
According to Epidemiologic Surveillance Report #4, the majority of cases—103—have been reported in Chiapas, where environmental conditions have facilitated ongoing transmission.
While human cases are relatively uncommon compared to infections in animals, as of February 9, 2026, over 600 cases have been reported in livestock and other animals nationwide, highlighting the broader impact of this serious health risk.
The NWS is a parasitic fly native to parts of the Americas. It lays its eggs in open wounds or on the mucous membranes of warm-blooded animals, including humans. The eggs hatch into larvae that burrow into living tissue, feeding on flesh and causing severe damage, pain, and potential secondary infections.
If left untreated, infestations can lead to serious complications and, in rare cases, may be fatal.
International health authorities are actively monitoring the situation through enhanced surveillance efforts.
Currently, the U.S. government is involved in regional initiatives that include sterile insect technique programs aimed at reducing fly populations and preventing further northward spread.
Animal cases (primarily in livestock) have been detected close to the Texas border, raising concerns about potential northward spread:
Tamaulipas has reported 8 active animal cases, and Nuevo León has had confirmed animal cases, including one in Sabinas Hidalgo, less than 70 miles from the Texas border.
Officials emphasize that the risk to the general public remains low with proper hygiene and wound care; however, vigilance is essential in endemic and outbreak areas.
As of February 12, 2026, no vaccines are available to protect people from this health risk.
According to the Argentine Ministry of Health, there has been an increase in hantavirus cases in early 2026, particularly affecting the Central Region of the country.
This region, which includes provinces such as Buenos Aires, Entre Ríos, and Santa Fe, has consistently reported the highest number of cases in recent seasons.
As of February 2, 2026, national health authorities confirmed a total of 14 cases in the new year, with 7 in Buenos Aires Province, 5 in Salta, 1 in Entre Ríos, and 1 in Río Negro.
The current epidemiological season (from week 27 of 2025 to the present) has shown heightened activity. Argentina has recorded approximately 70 confirmed cases, resulting in 20 deaths, which gives a case fatality rate (CFR) of around 34.5% — the highest rate seen in the past seven years.
The Ministry of Health emphasizes the importance of preventive measures, including avoiding contact with rodents, ensuring proper ventilation in enclosed spaces before entering, using protective gear when cleaning rodent-infested areas, and securely storing food items.
Currently, there is no vaccine for hantavirus. Still, clinical research is focused on DNA and mRNA candidates, with a Phase 2 study evaluating HTNV/PUUV DNA vaccines and new MVA-Hanta trials testing a modified vaccinia Ankara vector.
Furthermore, treatment is primarily supportive.
Early diagnosis within the critical 48-hour window after the onset of symptoms is essential for improving outcomes. Symptoms typically begin with flu-like signs and can progress to severe respiratory distress.
International organizations, including the Pan American Health Organization, are closely monitoring the situation in this South American country.
The yellow fever outbreak in the Republic of Colombia has intensified, with the latest data showing a continued rise in cases and fatalities in 2026.
As of February 8, 2026, Colombia's Ministry of Health confirmed 168 yellow fever cases, including 76 deaths, according to a Facebook post.
This new data represents an increase from earlier reports in late January 2026, when the cumulative total stood at 161 cases and 73 deaths.
Located on the northwestern coast of South America, the department of Tolima remains the epicenter, historically low-risk but now accounting for the majority of infections (previously reported at over 130 cases and dozens of deaths in the region alone).
Other Colombian departments include Caldas, Caquetá, Cauca, Guaviare, Huila, Meta, Nariño, Putumayo, and Vaupés.
The outbreak, which originated in late 2024 and escalated significantly through 2025, has been marked by a persistently high case-fatality rate, often exceeding 40-70% in various reporting periods, largely due to low vaccination coverage among affected populations in forested or rural areas where the mosquito-transmitted virus circulates.
With millions of travelers departing for Colombia from the U.S. each year, the Centers for Disease Control and Prevention's Travel Health Notice, Level 2, continues to recommend yellow fever vaccination for travelers to risk areas in Colombia at elevations generally below 2,300 meters, excluding major cities like Bogotá, Barranquilla, Cali, Cartagena, and Medellín.
Numerious health authorities urge residents and visitors in or traveling to endemic zones to get vaccinated at least 10 days before exposure, use mosquito protection, and seek immediate medical care if symptoms such as fever, headache, muscle pain, nausea, or jaundice appear.
When departing from the United States for Colombia, travel vaccination clinics offer the YF-Vax vaccine.